Spinal Fusion is used by the Surgeons at the Southwest Scoliosis and Spine Institute
Spinal Fusion
The surgical procedure called Spinal fusion joins two or more vertebrae together to form a single structure. The purpose is to avoid back pain by stopping mobility between the two bones. They can’t move as they used to once they’ve fused. This prevents you from straining surrounding nerves, ligaments, and muscles, which might cause pain.
What can I do if I’m not sure if I need a Spinal Fusion?
The term “spinal fusion” conjures up images of a terrifying procedure. So, how can you know if this is the proper operation for you? I’m not sure what spinal fusion is or whether I need it. Three basic criteria answer this question.
- Scoliosis is a type of spine deformity that requires surgery to rectify.
- A spine that is weak or unstable: corrects instability caused by severe arthritis.
- After removing a damaged disc, a herniated disc restores spine stability.
While spinal fusion has been shown as an effective treatment for these three disorders, it has not been demonstrated in the treatment of non-specific back pain.
Questions and Answers
What is Spinal Fusion?
Spinal fusion is a surgical procedure performed to join two or more vertebrae together, creating a solid bridge between them. The procedure is typically done to stabilize the spine, alleviate pain, and improve spinal alignment. During the surgery, bone grafts, implants, or other materials are used to promote bone growth and fuse the vertebrae into a single, solid structure.
Why do doctors recommend Spinal Fusion?
Spinal fusion may be recommended for various reasons, including degenerative disc disease, spinal instability, herniated discs, spinal fractures, scoliosis, or other conditions that cause spinal instability or chronic pain. The procedure aims to reduce pain by immobilizing the affected segment of the spine, restoring stability, correcting deformities, and preventing further damage or progression of the underlying condition.
What is the recovery time after Spinal Fusion Surgery?
The recovery process following spinal fusion surgery can vary depending on several factors, including the individual’s overall health, the extent of the surgery, and the specific condition being treated. Generally, patients can expect to spend a few days in the hospital for initial recovery and pain management. Following discharge, they may need to wear a brace to provide support and restrict movement during the initial healing period. Physical therapy and rehabilitation are often recommended to help regain strength, mobility, and flexibility. Full recovery can take several months, and it is important to follow post-operative instructions, attend follow-up appointments, and engage in prescribed exercises to optimize healing and achieve the best outcome.
Fusion Surgery Patient, Randall Graham
Randall had pain and weakness and numbness in his leg. Randall needed a spinal fusion at L4 & L5 for instability. After surgery, his life was better and just kept getting better. Before surgery, he could not even walk a city block. Now he is walking Natural Bridge Caverns in San Antonio , 18 stories up and down! Dr. Richard Hostin helped him get his life back!
The Benefit of Spinal Fusion Surgery
 When two vertebrae become fused, one solid bone forms rather than two. The pain associated with the mobility or instability of the two vertebrae gets relieved since they can no longer move independently. This surgery also stops the nerves around the vertebrae from stretching, which can help the patient feel better. Because only a small section of the spine becomes fused, spinal fusion surgery normally does not limit a patient’s range of motion upon full recovery.
When two vertebrae become fused, one solid bone forms rather than two. The pain associated with the mobility or instability of the two vertebrae gets relieved since they can no longer move independently. This surgery also stops the nerves around the vertebrae from stretching, which can help the patient feel better. Because only a small section of the spine becomes fused, spinal fusion surgery normally does not limit a patient’s range of motion upon full recovery.
However, during the initial recovery phase, doctors will temporarily restrict certain activities to aid healing. Most children can return to school within three to four weeks post-surgery, but participation in gym class or sports is generally advised against for a period ranging from two to six months, depending on the surgeon’s guidance.
Once a patient receives clearance from their doctor, they can gradually return to the activities they enjoyed before surgery. Nonetheless, it is often recommended to avoid contact sports such as football and rugby to prevent potential injury. The key to a successful recovery is adhering to medical advice and gradually resuming activity, ensuring the spine heals properly and safely.
Why Are You Having This Surgery?
If medications, physical therapy, and other procedures (such as steroid injections) haven’t eased back pain, spinal fusion should.
Doctors normally only prescribe treatment if they are certain about the source of the problem. If your back problem is caused by one of the following, spinal fusion may help:
- Severe scoliosis or kyphosis
- Spinal instability due to trauma or degenerative conditions
- Persistent pain unresponsive to conservative treatments
However, orthopedic surgeons often delay spinal fusion surgery, especially in children, until after they have reached their mature height. This delay is crucial because performing the surgery too early can interfere with natural growth, potentially leading to further complications or the need for additional surgeries.
Evaluation and Waiting
By waiting, surgeons aim to ensure that the procedure aligns with the child’s developmental milestones, maximizing the benefits and minimizing risks. This careful timing is part of a broader strategy to achieve the best long-term outcomes for patients.
- Degenerative disc disease (DDD) – Degeneration of the space between discs; sometimes the discs will rub together.
- Fragmentation (broken spinal bone).
- Scoliosis – The Spine curves from one side or both.
- Spinal stenosis – The narrowing of the spinal column.
- Spondylolisthesis – one of your vertebrae slips out of place onto the vertebra below it.
- Tumors or infections in the spine.
What Facilities Does the Orthopedics and Sports Medicine Department Provide?
The Orthopedics and Sports Medicine Department offers a comprehensive range of facilities designed to cater to diverse patient needs. As one of the nation’s leading pediatric orthopedic programs, they provide state-of-the-art care tailored to both children and adolescents.
Specialized Treatment Areas:
- Advanced Surgical Suites: Equipped with cutting-edge technology for complex orthopedic surgeries, ensuring precision and optimal recovery outcomes.
- Rehabilitation Centers: These include therapy rooms with the latest equipment for physical and occupational therapy, designed to aid in quicker rehabilitation.
- Diagnostic Imaging Facilities: Featuring advanced MRI, CT, and X-ray machines that allow for detailed and accurate assessments of various orthopedic conditions.
Comprehensive Sports Medicine Resources:
- Performance Enhancement Labs: Facilities to assess and improve athletic performance using biomechanics and motion analysis.
- Injury Prevention Programs: Dedicated spaces for education and training to help young athletes avoid common sports injuries.
Patient-Centric Amenities:
- Family Consultation Rooms: Comfortable areas designed for families to meet with specialists and discuss treatment plans in detail.
- Child-Friendly Environments: Decor and facilities are adapted to create a welcoming atmosphere to ease the anxiety of young patients.
With these diverse offerings, the department ensures holistic and individualized care tailored to the unique needs of each patient.
How to Prepare for Surgery?
If you haven’t had any recent blood tests or spinal X-rays, you could have them the week before your operation. The doctors will discuss the specifics of your procedure with you and your healthcare team. If anything doesn’t make sense, patients should ask questions. Your surgeon wants you to be well-informed about your procedure. In the days leading up to your operation, keep the following in mind:
- Arrive at the surgical center on time. You’ll require transportation to and from your destination.
- Make a list of the medications you may and cannot take in the days leading up to your surgery. Some medications, such as aspirin and other anti-inflammatory treatments, may be dangerous. Do not ever take medications without first consulting your physician.
- Before your treatment, find out if you can eat or drink anything.
- Prepare your house. Raised toilet seats, shower chairs, slip-on shoes, reaching, and other help will be required.
How Long Should Children Avoid Sports After Spinal Fusion Surgery?
After undergoing spinal fusion surgery, children need adequate time to heal before participating in sports activities. While most children may return to school within three to four weeks post-surgery, engaging in sports or gym class requires a longer recovery period.
Guidelines for Resuming Physical Activities:
- Initial Rest Period: It’s generally recommended that children refrain from sports and vigorous physical activities for a few months following their surgery.
- Consult with Surgeons: The exact timeframe can vary significantly. Some surgeons may advise avoiding sports for anywhere from two to six months, depending on the child’s healing process and the specifics of the surgery.
- Gradual Reintroduction: Once cleared by the medical professional, children should gradually ease back into physical activities. This gradual approach helps ensure their spine and body are ready to handle the strains of sports safely.
Overall, the key to a successful recovery and return to sporting activities lies in following the surgeon’s advice and ensuring that each step of the process prioritizes the child’s health and safety.
What is Spinal Instrumentation and How is it Used in Spinal Fusion Surgery?
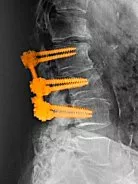
Spinal instrumentation is a crucial component in the field of spinal fusion surgery. It involves the use of metal rods, hooks, screws, and other devices that are strategically attached to the spine. These tools play a vital role in correcting abnormal spinal curvatures and ensuring the spine is stabilized in its correct position.
Role in Spinal Fusion Surgery
During spinal fusion surgery, the primary objective is to solidify two or more vertebrae, so they heal into a single, stable unit. Here’s how instrumentation contributes to this process:
- Stabilization: The metal hardware holds the spine in alignment, preventing it from shifting during the healing phase.
- Support: By maintaining proper positioning, the instrumentation allows the bone grafts placed during surgery to fuse correctly.
- Safety: The use of these devices helps reduce the risk of further deformity as the spine heals.
The Process
- Attachment: Surgeons first attach the instruments to the vertebrae needing correction.
- Alignment: The devices are adjusted to achieve the desired spinal alignment.
- Fusion: Bone grafts are placed to promote natural fusion, and the instrumentation ensures they remain in place as the bones grow together.
This combination of mechanical support and biological healing enables patients to regain improved posture and reduced discomfort, leading to better overall outcomes in spinal health.
The Operation
Spinal Fusion is conducted in two areas:
- Cervical Spinal Fusion (posterior)
- Cervical Spinal Fusion (anterior)
- Lumbar Spinal Fusion
There are two methods for spinal fusion:
- Anterior lumbar interbody fusion involves your surgeon entering your body through your stomach.
- Posterior fusion involves your surgeon entering your body from behind.
Posterior Fusion Surgery
Posterior fusion is the most common approach for treating idiopathic and neuromuscular scoliosis. During the procedure, after the patient receives anesthesia and is asleep, they are gently rolled onto their stomach. The surgeon makes an incision on the back, allowing access to the spine.
Once the incision is made, the muscles and tissues are moved aside to view the spine. The damaged or painful discs’ joint(s) are removed. To stabilize and join the discs, the surgeon may use screws, rods, or bone grafts. Surgeons will harvest these grafts from the patient’s hip or pelvis, or sourced from a donor. Some surgeons opt for bone morphogenetic protein (BMP) to stimulate bone growth.
Most patients with idiopathic scoliosis do not require a brace after surgery, while those with congenital scoliosis or spondylolisthesis typically have bone grafts without instrumentation and need to wear a brace during the healing process. Depending on the complexity, the surgery can take several hours.
Both anterior and posterior fusion surgeries
Surgeons may perform both anterior and posterior fusion procedures in specific complex cases to ensure spinal stability and alignment. These surgeries address different parts of the spine; the anterior targets the front and the posterior targets the back.
- Complicated spinal conditions: When there are intricate issues, such as severe curvature or deformities, addressing both the front and back of the spine can provide a more secure fusion.
- Stability requirement: Some patients need additional reinforcement from both sides to achieve the desired stability.
- Improved outcomes: Performing both surgeries can potentially enhance the overall outcome and speed up the recovery process by addressing issues comprehensively.
Often, these two procedures can occur on the same day, streamlining the treatment process. However, in some instances, scheduling will occur separately, typically one to two weeks apart, to ensure safety and optimal recovery.
What You Can Expect During Spinal Fusion
Surgeons execute spinal fusions while you’re asleep, so you’re completely unaware of what’s going on. Various procedures for conducting spinal fusion surgery have been devised by surgeons. The procedure employed by the surgeon determines the position of the fused vertebrae, the cause for the fusion, and, in certain cases, your overall health and body form.
The Following are Included in an Operation:
Incision. The surgeon creates an incision in one of three places to obtain access to the vertebrae that will be fused: directly over your spine in your neck or back, on either side of your spine, or in your belly or throat to reach the spine from the front.
Bone graft preparation. Bone grafts that join two vertebrae together might originate from a bone bank or your own body, generally your pelvis. If your bone is utilized, the surgeon will create an incision above your pelvic bone, extract a small amount of it, and then close it.
Fusion. The surgeon implants the bone graft material between the vertebrae to firmly fuse them. To keep the vertebrae together while the bone transplant cures, doctors will use metal plates, screws, or rods. Some surgeons employ synthetic material instead of bone transplants in certain circumstances. These synthetic chemicals aid in increasing bone development and accelerate vertebral fusion.
Recovering From Spinal Fusion:
You’ll remain in the hospital for many days following surgery. How much time it takes depends on a lot of factors, including your overall fitness level and whether you have any underlying medical concerns. The vast majority of visitors stay for at least four days. You may go home sooner, or you may have to stay for approximately a week.
Milestones for Discharge
As you recover, there are certain milestones you’ll need to meet before being discharged. Your doctor will assess your ability to:
- Walk independently: Getting up and moving is crucial for recovery.
- Shower and dress on your own: Demonstrating self-care capabilities is a key step.
Once these milestones are achieved, your doctor will discharge you with instructions to continue your recovery at home.
Monitoring and Equipment
During your stay, machines will monitor your heart and make sure your body remains healthy. You’ll also see a lot of tubes:
- An IV: Insertion of a very small line into your arm to provide fluids, antibiotics, and pain relievers.
- Epidural catheter: Some patients receive pain medication through a back tube.
- Urinary catheter: Another tube, sometimes known as a catheter, attaches to the area of your body where urine typically exits. For the first few days, you’ll have this, so you don’t have to get up to use the restroom. You may find it unpleasant, or you may not notice it at all. However, you must remain motionless so that your back can recover.
Recovery and Follow-Up
Occupational and physical therapists will teach you how to get out of bed, into a chair, and walk again during your stay. You’ll undergo spinal X-rays before your doctor sends you home to ensure that the fusion is working well.
In around ten days, you’ll return to remove the sutures. Following that, you’ll make follow-up appointments every four to six weeks, six months, twelve months, and twenty-four months. It takes time and effort to recover after back surgery. Your back may take anywhere from 6 months to a year to fully recover. After you leave the hospital, you should continue with physical therapy.
After Spinal Fusion:
Following spinal fusion, a two- to three-day hospital stay is commonly necessary. You may suffer some pain and pain depending on the location and degree of your operation, but the pain is typically effectively controlled with drugs. If you have any of the following symptoms after returning home, consult your doctor:
- Redness, tenderness, or swelling
- Wound drainage
- Shaking chills
- Fever greater than 100.4 F (38 C)
Post-Surgery Changes in the Spine: Months 6 to 12
Between six months and a year after spinal fusion surgery, significant healing occurs in the spine. The once-separated vertebrae meld together, forming a solid and stable bone structure. This transformation means that the fused section of the spine loses its ability to bend or increase in size.
Because of this rigidity, orthopedic surgeons often recommend waiting to perform spinal fusion until a child reaches their full height. This ensures that the fusion does not restrict natural growth prematurely. However, the vertebrae surrounding the fused area retain their flexibility and continue to grow and adapt, maintaining some overall spinal movement and function.
Surgery Results:
For fractures, abnormalities, or instability in the spine, spinal fusion is usually a successful procedure. When the reason for back or neck pain is unknown, however, study results are more mixed. In many situations, nonsurgical therapies for nonspecific back pain are just as successful as spinal fusion. Even if your X-rays reveal a herniated disc or bone spurs, doctors may find it difficult to pinpoint the particular cause of your back pain. Many people have X-ray evidence of back problems that they have never had pain from. As a result, your pain might not relate to any issues shown in your imaging scans.
When Can Children Typically Return to School After Spinal Fusion Surgery?
Recovering from spinal fusion surgery is a crucial period for children, and when they can return to school often depends on individual healing progress.
Timeframe for School Return:
Most children can resume attending school approximately three to four weeks following the procedure. However, this timeline can vary slightly based on the child’s health and the surgeon’s recommendations.
Physical Activities:
While returning to school is generally possible within a month, participation in gym classes or sports activities is another matter. Children should abstain from these physical activities for a period ranging from two to six months. The exact duration is best advised by the child’s surgeon, who will consider numerous factors related to recovery.
Ultimately, each case is unique, and following the surgeon’s guidelines ensures the best path to healing.
Why Choose Southwest Scoliosis and Spine Institute
Southwest Scoliosis and Spine Institute< doctors and surgeons are spine experts offering cutting-edge technology, comprehensive care, and dedicated nurses and technicians to ensure the best possible care for our patients. Our team specializes in treating a wide range of spinal conditions, providing comprehensive care not only for scoliosis but also for other complex spinal disorders. This means:
- Personalized treatment plans tailored to each patient’s unique needs.
- Advanced surgical and non-surgical options to address a variety of spinal issues.
- A collaborative approach involving expert physicians, surgeons, and support staff who are committed to delivering exceptional results.
- Comprehensive Pediatric Care: Focused on addressing the unique medical needs of children with cervical spine issues.
- Surgical Expertise: Access to a team of accomplished surgeons proficient in advanced procedures, ensuring the highest quality of surgical intervention.
- Compassionate Support: A commitment to caring for each patient with empathy and understanding, aiming to make their healthcare journey as smooth as possible.
- Tailored Treatment Plans: Customized care regimens designed to meet the specific health requirements of each child, promoting both safety and effectiveness.
With our state-of-the-art facilities and a focus on patient-centered care, we ensure that every individual receives the specialized attention and treatment they deserve.
Southwest Scoliosis and Spine Institute doctors and surgeons are spine experts with offices in Dallas, Plano, and Frisco, Texas, and offer cutting-edge technology, comprehensive care, and dedicated nurses and technicians to ensure the best possible care for our patients. Call today to make an appointment.
____________________
Citation: Orthoinfo – Spinal Fusion
The medical content on this page has been carefully reviewed and approved for accuracy by the Southwest Scoliosis and Spine Institute’s qualified healthcare professionals, including our board-certified physicians and Physician Assistants. Our team ensures that all information reflects the latest evidence-based practices and meets rigorous standards of medical accuracy, with oversight from our expert spine doctors to guarantee reliability for our patients.


