LUMBAR SPINAL FUSION SURGERY
Lumbar spinal fusion, a surgical procedure, fuses one or more of the lumbar or lower back spine vertebrae together permanently. This procedure will help minimize pain associated with numerous spinal problems.
At the Southwest Scoliosis and Spine Institute, our expert Lumbar Spinal Fusion Doctors and Surgeons are dedicated to diagnosing and treating spinal problems in children and adults to ensure comprehensive care tailored to each patient’s needs. With advanced techniques and a compassionate approach, our team diagnoses, treats, and cares for patients who need Lumbar Spinal Fusion Surgery.
The surgeons at the Southwest Scoliosis and Spine Institute are experts in conducting the Spinal Fusion procedure
Lumbar Spinal Fusion Surgery
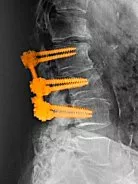 Stopping the pain caused by joints in the spine that have worn out constitutes the main goal of an operation on the skeletal system. Fusing joints in the spine reduced pain from degeneration. Specifically, a Lumbar Spinal Fusion Surgery fuses two bones, usually separated by a joint, together into one bone. To clarify, the medical term for this type of fusion procedure refers to arthrodesis.
Stopping the pain caused by joints in the spine that have worn out constitutes the main goal of an operation on the skeletal system. Fusing joints in the spine reduced pain from degeneration. Specifically, a Lumbar Spinal Fusion Surgery fuses two bones, usually separated by a joint, together into one bone. To clarify, the medical term for this type of fusion procedure refers to arthrodesis.
For your information, spinal fusion has been used for many years to treat painful conditions in the lumbar spine. Over the past decade, dramatic improvements have been implemented in the way that spinal fusion operations are performed. In addition, one major improvement has been the development of fixation devices.
Anatomy
In order to understand your symptoms and treatment choices, patients should understand the anatomy of the lower back. Also, this includes becoming familiar with the various parts that make up the lumbar spine and how these parts work together.
Computed Tomography (CT) Scans: Often combined with other imaging forms, CT scans provide a cross-sectional view of the spine, giving more in-depth insight into bone structure and any potential issues not visible in standard X-rays.
By analyzing these images, doctors can accurately diagnose the cause of spinal pain and determine if spinal fusion surgery appears as a suitable option.
Questions and Answers
The Definition of Lumbar Spinal Fusion
Lumbar spinal fusion refers to a surgical procedure that aims to stabilize the lower back (lumbar spine) by joining or “fusing” two or more vertebrae together. The procedure involves removing the damaged disc or bone tissue and using implants (such as screws, rods, or cages) and bone graft material to promote bone growth and fusion between the vertebrae. The fusion eliminates motion at the fused segment and provides stability to the spine.
Why do doctors perform Lumbar Spinal Fusion?
Surgeons perform lumbar spinal fusion to treat various conditions, including:
- Degenerative disc disease: When the intervertebral discs in the lower back become degenerated and cause instability or pain.
- Spinal instability: When it appears that excessive movement exists between the vertebrae, resulting in pain, nerve compression, or abnormal spinal alignment.
- Spondylolisthesis: When one vertebra slips forward in relation to the adjacent vertebra, causing spinal instability and nerve compression.
- Spinal fractures or tumors: In some cases, spinal fusion can stabilize the spine following fractures, or it can treat tumors affecting the lumbar region.
What recovery process do patients undergo after Spinal Fusion Surgery?
T
The recovery process following lumbar spinal fusion can vary depending on several factors, including the extent of the surgery, individual healing ability, and adherence to post-operative guidelines. However, some common aspects of the recovery process include:
- Hospital stay: Typically, patients stay in the hospital for a few days after surgery for close monitoring and pain management.
- Pain management: Doctors often prescribe medications to manage pain and discomfort during the initial recovery period.
- Physical therapy: Doctors may recommend physical therapy or rehabilitation to help regain strength, improve mobility, and promote healing. Doctors can tailor a structured exercise program to the individual’s needs and will gradually progress over time.
- Restrictions and precautions: Doctors advise patients to avoid heavy lifting, bending, twisting, or strenuous activities during the initial stages of recovery to protect the fusion site and facilitate proper healing.
- Follow-up appointments: Patients should schedule regular follow-up visits with the surgeon to monitor progress, evaluate the fusion’s success, and address any concerns or complications that may arise.
Types of Lumbar Interbody Fusion Approaches
The way a surgeon performs a lumbar interbody fusion can vary based on the route taken to reach the spine. These options offer different advantages and are selected according to the patient’s unique anatomy and the condition being treated. Here’s a closer look at the main approaches:
Anterior Lumbar Interbody Fusion (ALIF)
With the anterior approach, the surgeon works through the abdomen to access the spine. By reaching the spine from the front, doctors can remove a damaged disc and insert a bone graft or implant between the vertebral bodies. This route avoids disruption of the lower back muscles and spinal nerves, since the surgeon can gently move the abdominal contents aside, allowing a wide view of the disc space.
Posterior Lumbar Interbody Fusion (PLIF)
In the posterior approach, the surgeon makes the incision down the middle of the lower back. The surgeon moves the muscles aside and often removes a small portion of the vertebra (the lamina) to relieve nerve pressure and access the disc. The disc is taken out, and a bone graft or spacer goes in its place to join the vertebrae together. This method may also rely on screws and rods to secure the spine while fusion occurs.
Transforaminal Lumbar Interbody Fusion (TLIF)
A transforaminal approach is similar to PLIF but accesses the spine from a slightly angled path through one side of the back. By removing part of a facet joint, the surgeon can reach the disc space without moving nerve structures as much. After clearing away the disc, the surgeon will insert a bone graft or spacer to support fusion.
Lateral Lumbar Interbody Fusion (LLIF)
Unlike the front or back approaches, the lateral method comes in from the side of the body. Through a small incision over the patient’s flank, the surgeon can bypass major back muscles and other structures. This method avoids disturbing the spinal cord and is often used to address scoliosis, disc degeneration, or instability. The procedure is sometimes called “lateral access” or “direct lateral” fusion.
Oblique Lumbar Interbody Fusion (OLIF)
The oblique approach is a variation of the lateral method. Here, the surgeon reaches the spine at a diagonal angle, threading the way between the abdominal muscles and the psoas muscle (which runs alongside the spine). This technique helps to avoid both the back muscles and the nerves running near the psoas. Like LLIF, OLIF allows for the placement of an implant or graft between vertebrae while minimizing disruption to surrounding tissue.
Each of these surgical routes has its own indications, risks, and benefits. The best approach depends on your spine’s anatomy, the specific vertebrae involved, and the type of problem needing attention. Your surgeon will help determine which option is most likely to help you achieve a stable, pain-free spine.
When Do Surgeons Use Lumbar Spinal Fusion?
Only when all other conservative treatments have failed will your doctor suggest fusion surgery. This typically follows attempts with non-surgical interventions, such as physical therapy or injections, which have not successfully alleviated the pain.
To clarify, the following back conditions may require a spinal fusion, including:
- Scoliosis
- Degenerative disc disease
- Spinal instability
- Spine curvature
- Spondylolysis and spondylolisthesis
These conditions often result in chronic, severe back pain with known causes, such as age-related degenerative disc disease or a spinal tumor. Patients may experience pain anywhere in the spine, from the neck to the lumbar spine (lower back). The nature of this pain can vary significantly, presenting as sharp or dull pain, tingling, or numbness.
Understanding these symptoms and conditions helps determine when spinal fusion becomes a necessary intervention for restoring quality of life.
Scoliosis
By permanently connecting two or more vertebrae (spinal fusion) in your spine and eliminating motion between them, scoliosis and other types of spine conditions can become corrected. Spinal fusion surgery is a complex and intricate procedure; hence, the length of the surgery will vary by patient.
Degenerative Disc Disease
Degeneration of the discs between one or more vertebrae may require a spinal fusion of the vertebrae on both sides of the degenerative disc. The intervertebral discs look like flat, round “cushions” that act as shock absorbers between each vertebra in the spine. The disc allows motion to occur between each vertebra. Removing a degenerated disc and allowing the two vertebrae to fuse can reduce pain.
Learn more about degenerative disc disease.
Spinal instability
Each spinal segment is like a well-tuned part of a machine. All of the parts should work together to allow weight-bearing, movement, and support. When one segment deteriorates to the point of instability, it can lead to localized pain and difficulties. Segmental instability occurs when there is too much movement between two vertebrae.
To clarify, the excess movement of the vertebrae can cause pinching or irritation of nerve roots. Also, it can cause too much pressure on the facet joints, leading to inflammation. To further explain, it can cause muscle spasms as the paraspinal muscles try to stop the spinal segment from moving too much. The instability eventually results in faster degeneration in this area of the spine.
Spine Curvature
Surgeons use lumbar fusion for scoliosis and kyphosis — where the spine has an abnormal curve. These spine deformities may result from congenital or degenerative spine conditions. A lumbar fusion can stabilize the spine and correct the problem.
Learn more about degenerative adult scoliosis.
Spondylolysis and Spondylolisthesis
Spondylolisthesis, the term used to describe when one vertebra slips forward on the one below it, usually occurs when a spondylolysis (defect) exists in the vertebra on top. Two main parts of the spine keep each vertebra aligned with the disc and the facet joints. When spondylolisthesis occurs, the facet joint can no longer hold the vertebra back.
The intervertebral disc may slowly stretch under increased stress and allow the upper vertebra to slide forward. A surgeon may use fusion for both conditions to stop motion in the problem vertebrae.
Lumbar Spinal Fusion Surgery
During a spinal fusion, a bone graft joins two or more vertebrae. The vertebrae grow together during the healing process, creating a solid piece of bone. The bone graft helps the vertebrae heal together, or fuse. A bone from the pelvis can serve as a bone graft at the time of surgery. However, some surgeons prefer to use a bone graft from a bone bank (called an allograft).
Types of Bone Grafts
When considering spinal fusion, synthetic bone grafts are a valuable option. These grafts come in various forms, primarily using calcium and phosphate compounds that mimic natural bone properties.
- Autografts
Autografts are bone grafts taken from the patient’s own body, usually from the pelvis. This approach requires an additional incision during surgery, which can lead to longer procedure and recovery times, as well as increased discomfort during the healing process. - Allografts
Allografts are derived from donor bones. These grafts offer the benefit of eliminating the need for a second surgical site, potentially reducing recovery time. Additionally, laboratories can process allografts into demineralized bone matrices (DMBs), where the calcium is removed, and the bone is transformed into a putty. This putty is enriched with proteins that aid in healing. - Synthetic Options
Synthetic bone grafts are crafted from materials like calcium and phosphate. Doctors can tailor these options to suit specific needs and provide an alternative when natural grafts are not viable.
Choosing the Right Graft
During the decision-making process, a detailed discussion with your healthcare provider is essential. They’ll evaluate your specific condition and recommend the most suitable graft type that aligns with your body’s needs and the surgery’s requirements. The choice between these options will depend on various factors, including the specific medical situation and patient preferences. It’s important to discuss these possibilities with your doctor to determine the best approach for your spinal fusion procedure.
When considering bone graft options, understanding the potential benefits and drawbacks of autografts versus allografts is essential.
Autografts: Your Bone, Your Body
Benefits:
- Biocompatibility: Since autografts use bone from your own body, they are highly compatible and reduce the risk of immune rejection.
- Healing Potential: Autografts naturally contain living cells and growth factors that can enhance the healing process.
Drawbacks:
- Additional Surgery: Harvesting your bone typically requires an extra incision, often from the pelvis, leading to longer surgery and recovery times.
- Increased Discomfort: The additional procedure can lead to more pain and discomfort during the healing phase.
Allografts: Bone from a Donor
Benefits:
- No Additional Incisions: Using donor bone eliminates the need for a second surgical site, reducing immediate post-operative pain.
- Availability: Supplies of allografts remain readily available in various forms and sizes, offering flexibility for surgeons.
Drawbacks:
- Immune Response: There’s a slight risk of immune rejection since the graft comes from another person.
- Potential Infection Risk: Although carefully screened, donor tissue can carry a minimal risk of disease transmission.
Synthetic Grafts Man-Made:
For those considering alternatives, synthetic bones made from calcium and phosphate materials, or processed donor bones like demineralized bone matrices, can also be viable choices. Each type offers distinct advantages and considerations, making it crucial to consult with your doctor to determine the best option for your specific needs.
How Synthetic Bone Grafts Aid Healing
- Biocompatibility: Synthetic grafts are highly biocompatible, minimizing the risk of rejection or adverse reactions.
- Bone Regeneration: They encourage new bone growth, serving as a scaffold for natural bone cells to grow over time. This collaboration between graft and body promotes more effective fusion.
- Stability Improvement: By filling gaps between vertebrae, synthetic bone grafts provide stability, which is crucial for the healing process and eventual fusion of the spine.
- Reduced Harvesting Need: Unlike autografts, synthetic options eliminate the need for a secondary surgical site, preserving the patient’s natural bone.
Understanding the Difference: Minimally Invasive Spinal Fusion vs. Open Surgery
When considering spinal fusion, it’s crucial to understand the distinctions between minimally invasive techniques and traditional open surgery.
Incisions and Recovery:
- Minimally Invasive Spinal Fusion: This approach involves several small incisions, which means less trauma to the surrounding muscles and tissues. As a result, patients often experience reduced postoperative pain and a quicker recovery period.
- Open Surgery: In contrast, open surgery necessitates a larger incision. This allows for a direct view of the spine but typically leads to more extensive muscle disruption. Patients may encounter increased pain post-surgery and a longer healing time.
It’s important to note that recovery times can vary significantly, not just between minimally invasive and open techniques, but also depending on the specific type of spinal fusion performed. For instance, a minimally invasive lateral lumbar interbody fusion (LLIF) generally offers a shorter recovery compared to a posterior lumbar interbody fusion (PLIF).
Additionally, every patient’s experience should be considered as unique; individual factors like age, overall health, and the underlying spinal condition can influence healing. For the most accurate expectations, discuss your recovery timeline with your surgeon.
Precision and Technology:
- Minimally Invasive: Surgeons utilize advanced imaging and instruments to guide the procedure, allowing for precise operation with minimal impact on the body.
- Open Surgery: Surgeons have direct physical visibility of the spine, which can sometimes offer a broader perspective during complex procedures.
Hospital Stay:
- Minimally Invasive: Thanks to the less disruptive nature of the surgery, hospital stays are often shorter, and some patients can go home the same day.
- Open Surgery: The recovery period in the hospital can become longer due to the need for more extensive postoperative care.
In summary, while both procedures aim to achieve spinal stabilization, the choice may depend on the specific condition being treated and the surgeon’s recommendation based on the patient’s overall health and needs. Recovery varies by procedure and individual, so having an open conversation with your surgical team is the best way to set realistic expectations.
Learn more about the use of bone grafts.
Anterior, Posterior, or a Combined Approach for Lumbar Fusion Surgery.
Anterior Approach
In some cases, surgeons may consider placing the bone graft between the vertebral bodies. The anterior interbody approach allows the surgeon to remove the intervertebral disc from the front and place the bone graft between the vertebrae.
This operation begins by making an incision in the abdomen, just above the pelvic bone. The organs in the abdomen, such as the intestines, kidneys, and blood vessels, are moved to the side to allow the surgeon to see the front of the spine. The surgeon then locates the problem disc and removes it. The bone graft is placed into the area between the vertebrae where the disc has been removed.
This type of procedure, often referred to as an anterior lumbar interbody fusion (ALIF), is designed to restore the space between the vertebral bodies, which relieves pressure and creates more room for the spinal nerves to exit. Because this approach comes from the front, it avoids disrupting the low back muscles and reduces direct contact with sensitive nervous structures—an advantage over posterior (back) approaches.
Once the damaged disc is removed, an implant and bone grafting materials are placed between the vertebrae. Over time, the adjacent vertebral bodies fuse, creating a stable segment and helping to alleviate pain associated with the degenerated disc.
Posterior Approach
The posterior approach begins from the back of the patient. This approach can fuse the vertebral bones, or it can include removal of the problem disc. When the doctor removes a disc, a bone graft will replace it. Then the surgeon moves the spinal nerves to one side and inserts the bone graft between the vertebral bodies.
This is called a posterior lumbar interbody fusion. With a posterior approach, an incision starts in the middle of the lower back over the area of the spinal fusion. The surgeon moves the muscles to the side so that the surgeon can see the back surface of the vertebrae.
Once the spine is visible, the lamina of the vertebra is removed to take the pressure off the dura and nerve roots. This allows the surgeon to see areas of pressure on the nerve roots caused by bone spurs, a bulging disc, or a thickening of the ligaments. The surgeon can remove or trim these structures to relieve the pressure on the nerves. Once the surgeon sees that all pressure has been removed from the nerves, a fusion can proceed.
In many cases, fusion procedures are performed at the same time as spinal decompression surgeries to provide stability to the spine. For example, if the surgeon must remove a significant amount of bone to decompress the affected area, the resulting loss of support may make the spine unstable unless a fusion is also performed. By combining decompression and fusion, the surgeon both relieves nerve pressure and ensures the spine remains strong and properly aligned.
When operating from the backside of the spine, the most common method of performing a spinal fusion occurs when the surgeon places strips of bone graft over the back surface of the vertebrae.
Combined Approach
Working between the vertebrae from the back of the patient has limitations. Because of the fact that the spinal nerves are constantly in the way, the surgeon needs to proceed carefully. The movement of these nerves is limited. This limits the ability to see the area, and doctors do not have much room to use instruments and place implants.
For these reasons, many surgeons prefer to make a separate incision in the abdomen and actually perform two operations — one from the front of the spine and one from the back. The two operations occur at the same time, but they may happen several days apart.
Instrumentation
In the past, spinal fusions of the lumbar spine were performed without any internal fixation. The surgeon simply roughed up the bone, placed bone graft material around the vertebrae, and hoped the bones would fuse. Sometimes, patients were placed in a body cast to try to hold the vertebrae still while healing. The patient was lucky to have a 70 percent chance of successful fusion.
Spine surgery requires special knowledge, skills, and abilities to perform it well. The vertebrae are small, and there is not much room to place small instruments. Also, many nerves can get in the way of putting screws into the vertebral body. With the lower back sometimes getting a large amount of stress, it is difficult to find a metal device capable of holding the bones together. However, over the past two decades, some very inventive devices have changed the way surgeons perform spinal fusions.
Pedicle Screws and Rods
The surgeon may use some type of metal screws, plates, and rods to hold the vertebrae in place while the spine fusion heals. Designed to stabilize and hold the bones together while the fusion heals, these devices have greatly improved the success rate of fusion in the lower back.
Learn more about lumbar fusion using pedicle screws and rods.
Intervertebral Cages
A new type of device called an intervertebral fusion cage can assist in a spinal fusion between two or more vertebrae. These implants spread the two vertebrae apart while the fusion heals.
Learn more about spinal fusion using intervertebral cages.
Complications
Like all surgical procedures, operations on the spine may have complications. Because the surgeon operates around the spinal cord and nerves, back operations are always considered extremely delicate and potentially dangerous. Patients should take the time to review the risks associated with spine surgery with their doctor. Make sure you agree with both the risks and the benefits of the procedure planned for your treatment.
Learn more about possible complications of spine surgery.
Lumbar Spinal Fusion Surgery Recovery
The bones take a minimum of three months to fuse together and become solid. Yet the bone graft will continue to mature for one to two years. Your doctor may have you wear a rigid brace for up to three months to keep your spine still and make sure the bones fuse. You may not require a rigid brace after fusion with instrumentation.
Most patients return home when their medical condition stabilizes, usually within one week after fusion surgery. Limit your activities to avoid doing too much too soon. Avoid bending, lifting, twisting, and driving for at least six weeks.
Learn more about surgical aftercare.
Physical Therapy
Your doctor may have you attend physical therapy beginning a minimum of six weeks after surgery. A well-rounded rehabilitation program assists in calming pain and inflammation, improving your mobility and strength, and helping you do your daily activities with greater ease and ability. Patients may schedule Therapy sessions up to three times each week for eight to 12 weeks.
The goals of physical therapy provide the following to the patient:
- learn ways to manage your condition and control symptoms
- improve flexibility and core strength
- learn correct posture and body movements to protect the fusion
- return to work safely
The Expertise, Experience, Knowledge, and Trust are at Southwest Scoliosis and Spine Institute
For your information, our board-certified, fellowship-trained surgeons have diagnosed and treated more than 100,000 patients. In addition, we have successfully performed more than 16,000 surgeries and used spinal fusion surgery for many of those spine cases. If you are living with the pain of scoliosis or a spine condition, there is hope, and we want you to contact us. There is no reason to live in pain, and our doctors want to help. Appointments are available within 24 hours.
____________________
Citation: Healthline – Lumbar Spinal Fusion
The medical content on this page has been carefully reviewed and approved for accuracy by the Southwest Scoliosis and Spine Institute’s qualified healthcare professionals, including our board-certified physicians and Physician Assistants. Our team ensures that all information reflects the latest evidence-based practices and meets rigorous standards of medical accuracy, with oversight from our expert spine doctors to guarantee reliability for our patients.
If you or a loved one suffers from spinal pain, you owe it to yourself to call Southwest Scoliosis and Spine Institute at 214-556-0555 to make an appointment.


