HERNIATED DISC
A herniated disc, also known as a slipped or ruptured disc, occurs when the inner, softer portion of a spinal disc bulges out through a tear or crack in the outer, tougher portion of the disc. This can put pressure on the nerves in the spinal cord. This will cause pain, numbness, tingling, or weakness in the affected area of the body.
At the Southwest Scoliosis and Spine Institute, our expert Herniated Disc Doctors and Surgeons are dedicated to diagnosing and treating spinal problems in children and adults to ensure comprehensive care is tailored to each patient’s needs. With advanced techniques and a compassionate approach, our team diagnoses, treats, and cares for patients suffering from a Herniated Disc.
3 percent of individuals with progressive curvature may eventually experience severe problems that can include scoliosis and back pain, spinal problems, and nerve compression causing numbness, weakness, and leg pain.
Herniated Disc
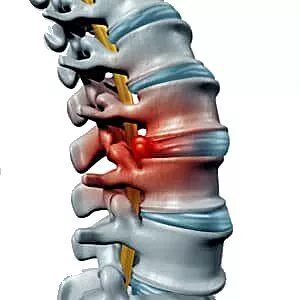 A herniated disc, also known as a slipped or ruptured disc, occurs when the inner, softer portion of a spinal disc bulges out through a tear or crack in the outer, tougher portion of the disc. This will put pressure on the nerves in the spinal cord. When that happens, a person will have pain, numbness, tingling, or weakness in the affected area of the body. Herniated discs most commonly occur in the lower back (lumbar region) and neck (cervical region). Treatment options include physical therapy, pain medication, and, in some cases, surgery.
A herniated disc, also known as a slipped or ruptured disc, occurs when the inner, softer portion of a spinal disc bulges out through a tear or crack in the outer, tougher portion of the disc. This will put pressure on the nerves in the spinal cord. When that happens, a person will have pain, numbness, tingling, or weakness in the affected area of the body. Herniated discs most commonly occur in the lower back (lumbar region) and neck (cervical region). Treatment options include physical therapy, pain medication, and, in some cases, surgery.
A herniated disc will cause pain. The disc or the rubbery cushions that sit between the vertebrae of the spine will have an issue. A herniated disc can occur anywhere in the spine, but it most commonly happens in the lower back. Depending on the location, it can cause pain, numbness, or weakness in an arm or leg.
Herniated Discs and Their Spine Locations
Herniated discs can occur in different regions of the spine, specifically the cervical (neck) region, the thoracic (mid-back) region, and the lumbar (lower back) region.
- Cervical disc herniation: This type of herniation occurs in the cervical region of the spine, involving seven vertebrae in the neck. A cervical herniated disc can cause symptoms such as neck pain, radiating pain or numbness in the arm and shoulder, and weakness in the arm or hand.
- Thoracic disc herniation: This type of herniation occurs in the thoracic region of the spine, consisting of up to twelve vertebrae in the mid-back. A thoracic herniated disc occurs less frequently than a cervical or lumbar herniated disc. The symptoms can vary depending on the location and size of the herniation.
- Lumbar disc herniation: This type of herniation occurs in the lumbar region of the spine, which consists of the five vertebrae in the lower back. A Lumbar herniated disc can cause symptoms such as lower back pain, radiating pain or numbness in the leg and foot, and weakness in the leg or foot.
It’s important to note that the location of the herniated disc can affect the symptoms and the treatment options. In general, cervical and lumbar herniated discs are more common than thoracic herniated discs. The lumbar herniated disc remains the most common type of herniated disc.
Questions and Answers
What is a Herniated Disc
A herniated disc, also known as a slipped disc or disc prolapse, occurs when the soft inner core of a spinal disc pushes through the tougher outer layer. This condition commonly affects the intervertebral discs of the spine, causing pain and discomfort. The herniation can occur due to age-related wear and tear, trauma, or repetitive stress on the spine.
What are the Symptoms of a Herniated Disc
The symptoms of a herniated disc can vary depending on the location and severity of the herniation. Common symptoms may include:
- Back or neck pain: Pain in the affected area of the spine provides doctors with a primary symptom. Patients may feel it in a localized area or feel it radiate to other parts of the body, such as the buttocks, legs, arms, or shoulders.
- Numbness and tingling: The herniated disc may compress nearby nerves, leading to sensations of numbness, tingling, or a “pins and needles” feeling in the affected area.
- Muscle weakness: Weakness or difficulty with certain movements may occur due to nerve compression. For example, a herniated disc in the lower back can lead to weakness in the legs or difficulty walking.
- Changes in reflexes: Reflexes may become diminished or exaggerated due to nerve involvement.
- Shooting pain: Certain movements or activities can trigger sharp, shooting pains that radiate down the arms or legs, known as radicular pain.
How is a herniated disc diagnosed and treated?
Diagnosing and treating a herniated disc typically involves the following:
- Diagnosis: A healthcare professional will evaluate the patient’s medical history, perform a physical examination, and may order diagnostic imaging tests such as MRI or CT scans. These imaging studies can provide detailed information about the location and extent of the herniation.
- Conservative treatment: Doctors use non-surgical treatments as the first line of approach for a herniated disc. These may include rest, pain medications, physical therapy, exercises to strengthen the surrounding muscles, hot or cold therapy, and lifestyle modifications.
- Epidural steroid injections: In some cases, corticosteroid injections into the space around the affected nerve root (epidural space) can help reduce inflammation and provide temporary pain relief.
- Surgery: If conservative treatments do not alleviate symptoms or if a severe nerve compression occurs causing significant weakness or loss of function, doctors may consider surgery. Surgical options include discectomy (removal of the herniated portion of the disc) or spinal fusion (stabilizing the spine with hardware and bone grafts).

The Different Types of Herniated Discs
A herniated disc occurs when the inner, softer portion of a spinal disc bulges out through a tear or crack in the outer, tougher portion of the disc. The following are different types of disc herniation:
- Protrusion: A protrusion herniation occurs when the disc bulges outwards but does not completely rupture. This type of herniation appears less severe than other types and may not put pressure on the nerves.
- Extrusion: An extrusion herniation occurs when the disc material ruptures and bulges outward. This type of herniation appears more severe than a protrusion and may put pressure on the nerves.
- Sequestered: A sequestered herniation appears as an extrusion — the disc material completely breaks off and migrates away from the main disc. This type of herniation appears as the most severe and can put significant pressure on the nerves.
- Central: Central herniations occur when the herniation occurs in the center of the disc. This type of herniation can compress the spinal cord, causing severe symptoms.
- Posterolateral: Posterolateral herniations occur when the herniation occurs on the back side of the disc and to the side. This type of herniation can compress the nerve root, causing radicular symptoms.
- Foraminal: Foraminal herniations occur when the herniation occurs in the foramen, a small opening where the nerve exits the spine. This type of herniation can compress the nerve root, causing radicular symptoms.
It’s important to note that doctors classify these types of herniations according to their degree of severity. However, the direction of the herniation is also used.
Causes
The causes of a herniated disc include:
- Age-related wear and tear: As we age, the discs in our spine can lose water content, making them more prone to injury.
- Trauma or injury: A traumatic injury to the spine, such as a car accident or fall, can cause a herniated disc.
- Repetitive motions: Repetitive motions, such as lifting heavy objects or performing the same movements over and over, can put stress on the discs in the spine and lead to a herniated disc.
- Poor posture: Poor posture can put extra pressure on the discs in the spine and lead to a herniated disc.
- Genetics: Some people may acquire herniated discs due to genetic factors that affect the structure and function of the spine.
- Obesity: Obesity can put extra stress on the spine and increase the risk of a herniated disc.
- Coughing: Chronic coughing and sneezing can cause a herniated Disc
- Nearby Nerve: Because spinal structures and nerves are near each other, irritation and pressure on the nerves do occur.
Leg Pain
A herniated lumbar disc compressing the sciatic nerve can produce sciatica, a type of nerve pain. There are two sciatic nerves, which appear on each side of the body. The sciatic nerve starts in the spine and extends down the leg. When a disc protrudes and presses on the sciatic nerve, pain can radiate down the leg. In some cases, the pain goes below the knee, and perhaps even into the foot.
It’s also worth noting that a herniated disc can also happen without any known cause. It’s important to see a doctor or specialist if you’re experiencing symptoms of a herniated disc. The doctor will determine the cause and the appropriate treatment.
Symptoms
Symptoms of a herniated disc can vary depending on the location of the disc and the severity of the injury. Some common symptoms include:
- Severe low back pain or neck pain that radiates to other areas of the body
- Numbness, tingling, or weakness in the affected area of the body, such as the legs, arms, or shoulders
- Muscle weakness, especially in the legs
- Loss of reflexes
- Difficulty walking or standing up straight
- Loss of bowel or bladder control (in severe cases)
It’s worth noting that many people possess herniated discs but do not display any symptoms. It’s only when the herniation presses on a nerve that symptoms appear. Also, some other conditions like spinal stenosis, arthritis, and osteoporosis may cause similar symptoms. So it’s important to get an accurate diagnosis from a doctor or specialist.
Diagnosis of a Herniated Disc: A Comprehensive Overview
A herniated disc, also known as a slipped or ruptured disc, occurs when the soft, gel-like center of an intervertebral disc (the nucleus pulposus) pushes through a tear or rupture in the outer fibrous layer (the annulus fibrosus). This condition can lead to compression of nearby spinal nerves, causing pain, numbness, and weakness. Diagnosing a herniated disc requires a multi-step process involving clinical evaluation, imaging studies, and differential diagnosis to confirm the condition and rule out other possible causes of the patient’s symptoms.
Clinical History
The diagnostic process typically begins with a thorough review of the patient’s medical history and presenting symptoms. Doctors see this step as critical for identifying the nature of the symptoms. Any information, including when and how it occurred, can help a doctor. Key aspects of the clinical history include:
- Nature of Pain: Patients with a herniated disc often report sharp, radiating pain that follows the path of the compressed nerve (radiculopathy). The pain may radiate down the arm (if the herniation occurs in the cervical spine) or down the leg (if in the lumbar spine, commonly known as sciatica).
- Onset of Symptoms: The patient may recall a specific incident, such as lifting a heavy object, which triggered the pain. However, in many cases, the herniation develops gradually due to degenerative changes in the disc.
- Location of Pain: The location and nature of the pain provide clues about the level of herniation. For example, a herniation at the L4-L5 level may cause pain that radiates down the side of the leg. However, a C6-C7 herniation may result in pain or tingling down the arm and into the fingers.
- Associated Symptoms: Numbness, tingling, muscle weakness, and loss of reflexes are common symptoms when nerve roots are compressed. The presence of bowel or bladder dysfunction may indicate a severe condition, such as cauda equina syndrome, requiring urgent evaluation.
Physical Examination
A focused physical examination helps in identifying signs of nerve compression and the specific level of the spine affected by the herniation. Some of the key elements of the physical examination include:
Neurological Assessment: A neurological exam evaluates motor strength, sensory function, and reflexes in areas supplied by the affected nerve root.
- Motor Testing: Muscle weakness in specific groups (e.g., quadriceps or dorsiflexion) may indicate nerve compression at particular spinal levels.
- Sensory Testing: Loss of sensation or altered sensation (paresthesia) in a dermatomal distribution can guide the clinician to the level of the herniation.
- Reflex Testing: Reflexes are often diminished in patients with a herniated disc due to nerve root compression. For example, the patellar reflex (knee jerk) may lessen in a patient with an L4 nerve root compression.
- Straight Leg Raise (SLR) Test: This test evaluates for lumbar disc herniation. The patient lies on their back while the clinician raises each leg individually. Pain that radiates down the leg when the leg raises between 30 and 70 degrees suggests nerve root irritation. This often occurs due to a herniated disc. A variation of this test, known as the crossed straight leg raise test, provides a more specific test for a herniated disc. Especially if lifting the unaffected leg causes pain in the affected leg.
- Spurling’s Test: This test assesses for cervical radiculopathy. The patient’s head gently rotates and tilts to the affected side while the examiner applies downward pressure. A positive test reproduces the patient’s arm pain, indicating nerve root compression from a cervical herniated disc.
Imaging Studies
Once the clinical evaluation suggests a herniated disc, imaging studies can confirm the diagnosis and assess the extent of the disc herniation. Common imaging modalities include:
- Magnetic Resonance Imaging (MRI): Doctors believe an MRI scan provides the gold standard for diagnosing herniated discs. It provides detailed images of the soft tissues, including the intervertebral discs, nerve roots, and spinal cord. MRI allows for visualization of the disc herniation, the level of herniation, and any compression of adjacent nerve structures. It also helps assess the severity of the herniation and whether other spinal conditions are present.
- Computed Tomography (CT): While doctors prefer MRI scans to see and evaluate soft tissue, CT scans can effectively evaluate bony structures. If patients possess pacemakers or metallic implants, Doctors will use a CT scan instead of an MRI. CT often combines with a myelogram (injection of contrast dye into the spinal canal). This enhances visualization of the spinal cord and nerve roots.
- X-rays: Although X-rays cannot directly visualize disc herniations. However, they are often used in the initial evaluation to rule out other causes of pain. For example, fractures, degenerative disc disease, or abnormal spinal alignment. They may also reveal indirect signs of a herniated disc.
- Electromyography (EMG) and Nerve Conduction Studies: These tests assess the electrical activity of muscles and the function of nerves. They can help confirm nerve root compression where the diagnosis appears unclear or when symptoms are inconsistent with imaging findings. EMG may detect signs of denervation or nerve injury. Nerve conduction studies assess the speed and strength of electrical signals in the affected nerves.
- Myelography: A myelogram consists of an X-ray and a contrast dye. The doctor injects the dye into the spinal canal before the X-ray. Doctors use this test when other imaging tests are not conclusive.
Differential Diagnosis
Doctors believe that a thorough diagnosis must be conducted, as other conditions can mimic the symptoms of a herniated disc. Therefore, doctors should consider the following conditions and rule out:
- Spinal Stenosis: Narrowing of the spinal canal can compress the spinal cord and nerves. Spinal Stenosis leads to similar symptoms as a herniated disc, including leg or arm pain and weakness. However, stenosis appears more common in older adults and tends to cause pain with standing or walking.
- Degenerative Disc Disease: While related to herniation, degenerative disc disease refers to the breakdown of the intervertebral disc. It leads to chronic pain. It often presents with persistent low back pain without the acute onset of radicular symptoms seen in herniations.
- Facet Joint Arthritis: Arthritic changes in the facet joints of the spine can cause localized pain and stiffness, sometimes radiating to nearby areas. However, unlike a herniated disc, facet joint pain does not typically follow a dermatomal pattern and lacks neurological deficits.
- Piriformis Syndrome (in the case of sciatica-like symptoms): This condition occurs when the piriformis muscle in the buttock compresses the sciatic nerve, leading to pain that mimics sciatica. However, piriformis syndrome does not involve true nerve root compression from the spine.
- Cauda Equina Syndrome: This medical emergency refers to the compression of the nerve roots at the lower end of the spinal cord. This condition normally stems from a large herniated disc. It presents with severe lower back pain, numbness in the groin area, and bowel or bladder dysfunction. This requires Immediate medical intervention to prevent permanent neurological damage.
Advanced Diagnostic Techniques
In certain cases, doctors will use more advanced diagnostic tools to further evaluate the severity or complexity of a herniated disc.
- Discography: This invasive test, which requires a technician to inject contrast dye into the intervertebral disc, will identify a disc as the source of pain. Doctors do not normally use Discography unless surgery is likely and the source of pain is unclear.
- Provocative Testing: These tests attempt to reproduce the patient’s symptoms by applying pressure to the suspected herniated disc or affected nerve root. For example, bending or extending the spine in specific ways during physical examination may help localize the site of compression.
Conclusion
Doctors diagnose a herniated disc using a meticulous and multi-faceted process that integrates the patient’s clinical history, a detailed physical examination, and a range of imaging studies. Proper diagnosis provides an essential guide for the treatment approach, which may range from conservative management (e.g., physical therapy and medications) to surgical intervention, depending on the severity of the condition and the level of nerve involvement. As with any spinal disorder, timely diagnosis and intervention are critical to improving outcomes and preventing long-term complications.
Medical Advice for A Herniated Disc
If you have been diagnosed by one of our doctors at the Southwest Scoliosis and Spine Institute with a herniated disc, it’s important to follow your doctor’s recommendations for treatment and management. However, some general tips can help to alleviate pain and improve your overall well-being:
- Rest: It’s important to rest the affected area of the body as much as possible. Avoid activities that put unnecessary stress on the spine, such as heavy lifting or repetitive motions.
- Exercise: Gentle exercise can help reduce pain and improve flexibility. Physical therapy can provide exercises that will alleviate pain and improve spinal function.
- Medications: Follow your doctor’s recommendations for taking pain medications or other medications as prescribed.
- Ice and heat: Applying ice or heat to the affected area can help reduce pain and inflammation.
- Good posture: Good posture can help reduce stress on the spine and alleviate pain.
- Maintain a healthy weight: Maintaining a healthy weight can help reduce stress on the spine and reduce the risk of a herniated disc.
- Avoid smoking: Smoking can decrease the blood flow to the discs in the spine, making it harder for them to heal.
Non-Surgical Treatments for a Herniated Disc:
While some herniated disc cases may eventually require surgical intervention, the majority of patients benefit significantly from non-surgical treatments. These treatments are aimed at relieving pain, reducing inflammation, restoring function, and preventing further injury. The list below provides a comprehensive breakdown of the different types of non-surgical treatments available for managing a herniated disc:
1. Physical Therapy (PT)
Physical therapy implements non-surgical treatment for a herniated disc. A tailored physical therapy program can help reduce pain, improve mobility, and strengthen the muscles around the spine to prevent further injury.
- Core Strengthening: Building strength in the muscles surrounding the spine, particularly the core muscles, helps to provide stability to the spine and reduces pressure on the intervertebral discs. This includes exercises like planks, bridges, and pelvic tilts.
- Flexibility Exercises: Stretching exercises targeting the hamstrings, lower back, and hip flexors are essential to improving the range of motion and relieving pressure on the spine. PT experts recommend gentle stretching of the piriformis and hip muscles in the treatment of lumbar disc herniations.
- Posture Training: Learning proper body mechanics and posture can help reduce the risk of further disc herniation. Therapists may teach ergonomic adjustments for sitting, standing, and lifting.
- Manual Therapy: Techniques such as massage, myofascial release, and spinal mobilization (not manipulation) will relieve tight muscles, reduce inflammation, and ease pressure on the affected nerve.
- Aquatic Therapy: For some patients, doctors will recommend exercises in a pool (aquatic therapy) as buoyancy reduces stress on the spine. This environment allows for a wider range of motion without exacerbating pain.
2. Medications
Medications play a key role in reducing inflammation, managing pain, and improving mobility during the recovery process.
- Non-Steroidal Anti-Inflammatory Drugs (NSAIDs): NSAIDs, such as ibuprofen (Advil, Motrin) or naproxen (Aleve), are commonly used to reduce inflammation and relieve pain caused by nerve irritation or inflammation around the herniated disc.
- Acetaminophen: While acetaminophen (Tylenol) doesn’t reduce inflammation, it helps with pain management, especially when NSAIDs are contraindicated due to gastrointestinal or cardiovascular risks.
- Muscle Relaxants: In some cases, herniated discs can cause muscle spasms in the back or neck. Muscle relaxants relieve these spasms.
- Oral Corticosteroids: A short course of oral corticosteroids, such as prednisone, may quickly reduce inflammation around the herniated disc and affected nerve roots.
- Neuropathic Pain Medications: For nerve-related pain, medications like gabapentin (Neurontin) or pregabalin (Lyrica) can help relieve neuropathic pain by calming irritated nerves.
- Opioids: In severe cases of acute pain, opioids will reduce and stop the pain. However, these medications are generally avoided due to the risk of dependence and side effects like sedation and constipation.
3. Epidural Steroid Injections
For patients who experience significant nerve pain from a herniated disc, doctors will recommend epidural steroid injections.
- Procedure: During an epidural steroid injection, a doctor injects a corticosteroid into the epidural space around the affected nerve. This happens under X-ray guidance (fluoroscopy) to ensure accurate placement.
- Effects: The steroid reduces inflammation and swelling around the herniated disc and nerve root, alleviating pain and allowing for greater mobility. Relief can last from weeks to months, depending on the individual case.
- Limitations: Epidural steroid injections are typically limited to a few treatments per year, as repeated use can lead to side effects such as weakened bones or immune suppression. They are often used in conjunction with other treatments like physical therapy.
4. Chiropractic Care
Chiropractic care can sometimes help with certain types of herniated discs, though this treatment needs a licensed professional familiar with spinal pathologies.
- Spinal Manipulation (Chiropractic Adjustments): Chiropractors may perform spinal adjustments (also known as chiropractic manipulation) to relieve pressure on the nerves and improve spinal alignment. However, adjustments must occur gently, especially when a herniated disc exists.
- Contraindications: Spinal manipulation is contraindicated in patients with significant neurological deficits, spinal instability, or cauda equina syndrome, as it may exacerbate symptoms or cause further injury. Chiropractic care will produce positive results in rare cases, and therefore, doctors must approve its use and the person who will conduct it.
5. Heat and Cold Therapy
Applying heat or cold to the affected area can help manage acute and chronic pain associated with a herniated disc.
- Cold Therapy: Cold packs reduce inflammation by constricting blood vessels and numbing the affected area. Cold therapy works well in the first 48 hours following an injury or flare-up of pain.
- Heat Therapy: Heat increases blood flow to the area, promoting healing and relaxing tight muscles. Heat packs, warm baths, or heating pads can provide relief from chronic pain or muscle stiffness.
- Alternating Heat and Cold: Some patients find that alternating heat and cold therapy provides the best relief, using cold therapy to reduce inflammation and heat therapy to relax the muscles.
6. Activity Modification and Rest
While doctors do not recommend prolonged bed rest for herniated discs, short-term rest and activity modification are often advised to prevent aggravation of symptoms.
- Rest: Short periods of rest, especially during acute flare-ups, can help to relieve pressure on the herniated disc. Patients are encouraged to rest in positions that minimize strain on the spine, such as lying with knees bent or using pillows for support.
- Activity Modification: Avoiding activities that put excessive strain on the spine is crucial. These activities include heavy lifting, prolonged sitting, and certain sports that involve twisting or bending. Gradual reintroduction of activity, guided by physical therapy, is important to prevent deconditioning and to support recovery.
7. Lifestyle Modifications
Certain lifestyle changes can aid in managing the symptoms of a herniated disc and prevent future episodes.
- Weight Management: Excess weight, especially around the abdomen, increases pressure on the spine and may exacerbate disc herniation. Achieving a healthy weight through diet and exercise can help relieve pressure on the discs and improve overall spinal health.
- Smoking Cessation: Smoking is known to reduce blood flow to the discs, accelerating the degenerative process. Quitting smoking can promote disc health and improve healing outcomes.
- Ergonomics: Adjusting posture and ergonomics in the workplace and at home is essential. Using lumbar support chairs, adjusting the height of computer screens, and taking frequent breaks from sitting can all help reduce spinal stress.
- Regular Exercise: After recovery, maintaining a routine of low-impact aerobic exercises like walking, swimming, or cycling can help strengthen the back and core muscles, improving spinal support and reducing the risk of future disc herniations.
8. Alternative Therapies
A variety of alternative therapies may also provide relief from herniated disc symptoms. While these treatments are not always supported by high-level scientific evidence, many patients report symptomatic relief.
- Acupuncture: Acupuncture involves inserting thin needles into specific points on the body to stimulate nerves, muscles, and connective tissues. It may help relieve pain and promote healing in patients with herniated discs.
- Yoga and Pilates: These practices focus on flexibility, core strength, and spinal alignment. Instructors experienced in working with individuals with spinal conditions can guide patients in gentle movements that avoid placing excess stress on the spine.
- Massage Therapy: Therapeutic massage may relieve muscle tightness and improve circulation, reducing pain and stiffness in patients with herniated discs.
9. Traction Therapy
Spinal traction therapy involves using mechanical forces to gently stretch the spine and create more space between the vertebrae. This may help relieve pressure on the herniated disc and compressed nerves.
- Manual or Mechanical Traction: Traction with the aid of a mechanical device that applies controlled pulling forces to the spine produces positive results.
- Effectiveness: While some patients report relief with traction therapy, its efficacy remains debated in the medical community. It is typically used as part of a broader treatment plan in conjunction with physical therapy and other interventions.
Conclusion
Non-surgical treatment options for a herniated disc are varied and can meet the needs of each patient. A combination of physical therapy, medications, lifestyle modifications, and other conservative therapies can often lead to significant pain relief and functional improvement without the need for surgery. For most patients, the key to successful treatment lies in adhering to a well-structured, interdisciplinary approach that addresses both the symptoms and the underlying causes of the herniated disc. Early intervention and a proactive approach to managing the condition can prevent the progression of symptoms and the need for more invasive treatments.
Long-Term Management and Prevention
Once the acute pain from a herniated disc subsides, long-term management focuses on preventing future disc herniations and maintaining spine health. The following measures are critical for preventing recurrence:
- Ongoing Physical Therapy: Continuing with exercises prescribed by a physical therapist can help maintain flexibility, core strength, and overall spinal stability. Patients should incorporate these exercises into their daily routine to prevent further injuries.
- Postural Awareness: Learning proper posture and movement mechanics, especially when lifting or carrying objects, is essential for reducing strain on the discs. Patients are encouraged to use their legs, not their back, when lifting heavy items, and to avoid twisting motions.
- Routine Low-Impact Exercise: Regular physical activity, such as swimming, walking, or cycling, helps improve circulation to the spine, keeping the discs and muscles healthy. Low-impact aerobic exercises are less likely to place excessive stress on the spine, making them ideal for long-term maintenance.
- Ergonomic Adjustments: Ensuring that workspaces, especially those involving prolonged sitting or standing, are designed with spinal health in mind can help reduce pressure on the discs. Using chairs with proper lumbar support and keeping computer monitors at eye level are simple changes that can make a significant difference.
Conclusion
Non-surgical treatments for a herniated disc offer a wide array of options, from physical therapy and medication to lifestyle adjustments and alternative therapies. The majority of patients with a herniated disc can experience significant pain relief and regain mobility through conservative care. A tailored, multidisciplinary approach not only addresses acute symptoms but also supports long-term spine health, enabling patients to lead active, pain-free lives. Early diagnosis and intervention, combined with a commitment to long-term management, are key to achieving the best possible outcomes in the treatment of herniated discs.
Surgical Treatments for a Herniated Disc: A Detailed and Explicit Overview
Surgical intervention for a herniated disc is typically considered after conservative treatments—such as physical therapy, medications, and injections—fail to alleviate the symptoms or when the condition is severe, causing significant pain, weakness, or neurological deficits. Surgery aims to relieve pressure on the affected nerve root, stabilize the spine, and restore function. While there are several surgical options, the choice of procedure depends on the location and severity of the herniated disc, the patient’s overall health, and the surgeon’s expertise.
This document provides a thorough and intricate examination of the different types of surgical treatments for herniated discs, detailing their techniques, benefits, and risks.
1. Microdiscectomy
Microdiscectomy is the most common surgical procedure used to treat herniated discs, particularly in the lumbar (lower back) region. It is a minimally invasive procedure that involves removing the portion of the disc that is compressing the nerve root.
Procedure:
- The surgeon makes a small incision (typically 1-1.5 inches) in the lower back.
- A special microscope or magnifying tool is used to enhance visibility.
- The muscles and tissues are gently retracted, and the removal of a small portion of the bone or ligament provides access to the herniated disc.
- The herniated portion of the disc that is pressing on the nerve is carefully removed.
- The remaining healthy part of the disc remains intact to maintain spinal stability.
Benefits:
- Microdiscectomy is highly effective in relieving leg pain (sciatica) caused by nerve compression.
- Because it is minimally invasive, patients typically experience quicker recovery times, less post-operative pain, and a lower risk of complications compared to traditional open surgery.
Risks:
- While the surgery is generally safe, potential risks include infection, nerve damage, bleeding, or the recurrence of the disc herniation.
- A small percentage of patients may experience continued pain if the nerve has been permanently damaged by the initial compression.
2. Laminectomy
Laminectomy, also known as decompression surgery, is a procedure often used when a patient has a herniated disc. If the herniated disc causes significant pressure on the spinal cord or nerves, this procedure will fix the problem.
Procedure:
- The surgeon removes part or all of the lamina, which is the bony structure at the back of the vertebra, to create more space for the spinal nerves.
- This relieves pressure by widening the spinal canal and reducing the nerve compression caused by the herniated disc or other conditions like bone spurs.
- In some cases, the surgeon will remove a portion of the herniated disc to decompress the nerve.
Benefits:
- Laminectomy provides relief from severe leg or arm pain, numbness, and weakness caused by nerve compression.
- It is particularly effective for patients with both a herniated disc and spinal stenosis or other degenerative changes in the spine.
Risks:
- Risks include infection, bleeding, and damage to the spinal cord or nerves.
- Laminectomy can lead to spinal instability in some patients, requiring additional stabilization procedures, such as spinal fusion.
3. Percutaneous Discectomy (Endoscopic Discectomy)
A percutaneous discectomy is a minimally invasive surgical option for patients with smaller disc herniations. This procedure is performed using a needle or an endoscopic device. This allows the surgeon to remove a portion of the herniated disc without the need for a large incision.
Procedure:
- A doctor inserts a thin needle or tube through the skin and guides it to the affected disc under X-ray or fluoroscopic guidance.
- Specialized instruments or lasers are used to remove the herniated portion of the disc.
- In some cases, a small amount of the nucleus pulposus is removed to reduce disc pressure.
Benefits:
- Because it is minimally invasive, percutaneous discectomy has a quicker recovery time and less post-operative pain than open surgery.
- It can occur on an outpatient basis, meaning patients may go home the same day.
Risks:
- The success rate is lower for percutaneous discectomy compared to microdiscectomy, especially for large or complex disc herniations.
- There is a risk of nerve or vascular injury during the procedure.
- The doctor may repeat the procedure if the herniation recurs or if the first procedure does not relieve the symptoms.
4. Artificial Disc Replacement (ADR)
Artificial disc replacement (ADR) is a motion-preserving surgery that replaces the damaged disc with an artificial one. This procedure is generally considered for patients with a single-level disc herniation and is an alternative to spinal fusion, especially in younger patients.
Procedure:
- The surgeon removes the damaged disc entirely through an anterior (front) approach to the spine, usually through the abdomen.
- An artificial disc made of metal and/or plastic is implanted in the space between the vertebrae.
- The artificial disc allows for continued movement of the spine, as it mimics the function of a natural disc.
Benefits:
- ADR preserves motion at the affected spinal level, which may reduce stress on adjacent discs and reduce the risk of future degeneration.
- Recovery time is often quicker compared to spinal fusion, as the spine remains more flexible.
Risks:
- As with any surgery, there are risks of infection, bleeding, and nerve or blood vessel damage.
- There is a risk that the artificial disc could shift or wear out over time, potentially requiring revision surgery.
- Not all patients are candidates for ADR, especially those with significant spinal instability or multi-level disc disease.
5. Spinal Fusion
Spinal fusion is a procedure that fuses two or more vertebrae to stabilize the spine. It is typically used in cases where a herniated disc causes significant instability or when multiple discs are damaged.
Procedure:
- The surgeon removes the damaged disc and places bone grafts or synthetic materials between the affected vertebrae.
- Surgeons will use metal rods, screws, or plates to hold the vertebrae together while the bone heals and fuses the two vertebrae into a single, solid piece of bone.
- Surgeons can implement fusion through the front (anterior), back (posterior), or side (lateral) of the spine, depending on the location of the herniated disc.
Benefits:
- Spinal fusion provides significant stabilization for patients with spinal instability or degenerative disc disease.
- It can effectively reduce pain and prevent further damage to the spinal nerves.
Risks:
- Fusion eliminates motion at the fused spinal segment, which can increase stress on adjacent discs, potentially leading to degeneration in other parts of the spine (adjacent segment disease).
- Recovery from spinal fusion can take several months, as it takes time for the bones to fuse completely.
- Other risks include infection, hardware failure, non-union (failure of the bones to fuse), and chronic pain at the fusion site.
6. Chemonucleolysis
Chemonucleolysis is a less common procedure that involves injecting an enzyme called chymopapain into the herniated disc to dissolve part of the nucleus pulposus. This reduces pressure on the affected nerve.
Procedure:
- Under local anesthesia, a needle is inserted into the herniated disc, and chymopapain is injected into the nucleus pulposus.
- The enzyme dissolves the disc material, reducing the size of the herniation and relieving nerve compression.
Benefits:
- It is a minimally invasive procedure with a quick recovery time.
- Chemonucleolysis avoids the need for a large incision or removal of bone or tissue.
Risks:
- There is a risk of an allergic reaction to the enzyme.
- Chemonucleolysis is not effective for all types of herniated discs and is rarely used today due to the availability of other, more effective surgical options.
7. Foraminotomy
Foraminotomy is a procedure used when a herniated disc causes narrowing of the foramen—the passage through which spinal nerves exit the spinal canal.
Procedure:
- The surgeon removes part of the bone or tissue that is compressing the nerve root within the foramen.
- Surgeons may partially remove the herniated disc to relieve nerve pressure.
Benefits:
- This procedure relieves nerve compression and helps improve pain, numbness, or weakness in the extremities.
- Surgeons can perform a foraminotomy as a minimally invasive surgery, which reduces recovery time.
Risks:
- There is a risk of spinal instability, particularly if too much bone is removed, which may require fusion surgery in the future. Other risks include infection, nerve damage, and blood loss.
Conclusion
Surgical treatments for herniated discs are varied, and surgeons can tailor the procedure to meet the specific needs of each patient. From minimally invasive procedures like microdiscectomy to more complex interventions like spinal fusion and artificial disc replacement, the choice of surgery depends on factors such as the severity of the disc herniation, the patient’s overall health, and the specific symptoms being experienced.
Each procedure carries its benefits and risks, and the patient’s decision to undergo surgery should take place in close consultation with a spine specialist who can assess the patient’s condition and recommend the most appropriate intervention.
For many patients, the goal of surgery for a herniated disc is to relieve pressure on the spinal nerves or spinal cord, reduce pain, and restore function. However, the decision to undergo surgery occurs only after exhausting non-surgical treatments or if the patient indicates a significant risk of permanent nerve damage or disability.
Factors to Consider When Choosing Surgical Treatment
- Severity of Symptoms: Patients with severe pain, weakness, or loss of bladder or bowel control (cauda equina syndrome) often require immediate surgery to prevent permanent damage.
- Location of the Herniation: The specific location of the herniated disc plays a significant role in determining the type of surgery. For example, microdiscectomy is most commonly used for lumbar herniated discs. On the other hand, anterior cervical discectomy and fusion (ACDF) occurs with cervical disc herniations.
- Age and Overall Health: Patients’ age, physical condition, and comorbidities can influence which surgical options are feasible. Older patients or those with multiple health issues may require a more conservative surgical approach. However, younger, healthier patients may choose procedures like artificial disc replacement, which preserves motion.
- Spinal Stability: If the herniated disc causes significant instability or if there are other degenerative changes in the spine, surgeons may recommend fusion surgery to stabilize the spinal segment. In contrast, minimally invasive procedures are more appropriate for patients without significant instability.
- Surgeon’s Expertise: The experience and specialization of the surgeon also influence the choice of surgery. Some surgeons may have extensive experience with minimally invasive techniques. Meanwhile, others may specialize in more complex reconstructive surgeries like fusion or artificial disc replacement.
- Patient’s Lifestyle and Goals: Doctors take the patient’s expectations, activity level, and desired outcomes into account. For example, athletes or individuals with physically demanding jobs may prefer motion-preserving procedures. For instance, artificial disc replacement, while patients with less demanding lifestyles may opt for fusion.
Postoperative Care and Recovery
Regardless of the type of surgery, postoperative care and rehabilitation are crucial for a successful outcome. After surgery, patients typically follow a recovery plan that includes:
- Physical Therapy: Physical therapy helps patients regain strength, flexibility, and range of motion after surgery. A structured rehabilitation program is often initiated within days or weeks of surgery, depending on the type of procedure performed.
- Pain Management: Pain is managed postoperatively through a combination of medications, such as NSAIDs, muscle relaxants, and sometimes short-term opioids. Ice, heat, and rest are also common strategies for managing discomfort.
- Activity Modification: Patients are often advised to avoid heavy lifting, bending, or twisting during the initial recovery period. Gradual reintroduction of daily activities and low-impact exercises is typically recommended to ensure a smooth recovery.
- Follow-up Care: Regular follow-up appointments with the surgeon are essential to monitor healing, check for complications, and assess the spine. Imaging tests (e.g., X-rays or MRIs) evaluate the success of the surgery.
Risks and Complications of Herniated Disc Surgery
Although surgical treatments for herniated discs are generally safe and effective, they carry potential risks and complications, including:
- Infection: Infection at the surgical site or deeper within the spine poses a risk with any surgical procedure, but is rare with proper sterile techniques.
- Nerve Damage: There exists a small risk of damage to the spinal nerves or spinal cord during surgery, which could result in numbness, weakness, or, in rare cases, paralysis.
- Recurrent Herniation: In some cases, the disc may herniate again, either at the same level or at a different spinal level. This may require additional surgery.
- Spinal Instability: Certain procedures, such as laminectomy or foraminotomy, can weaken the structural stability of the spine, potentially leading to the need for fusion surgery later on.
- Adjacent Segment Disease: After spinal fusion, the segments above or below the fused vertebrae may degenerate more rapidly, a condition known as adjacent segment disease.
- Chronic Pain: Some patients may experience chronic pain after surgery, particularly if pre-existing nerve damage exists or if complications arise during recovery.
Conclusion
Surgical treatment for a herniated disc offers several options, each with its unique advantages, risks, and considerations. From minimally invasive procedures like microdiscectomy and percutaneous discectomy to more complex surgeries like spinal fusion and artificial disc replacement, the appropriate surgical approach depends on the severity of the herniation, patient-specific factors, and the surgeon’s expertise.
Patients considering surgery should thoroughly discuss the matter with their surgeon to weigh the benefits and risks of the procedure. In most cases, surgery can provide significant pain relief, improved mobility, and protection against further nerve damage. However, successful outcomes depend not only on the surgical procedure but also on careful postoperative care. Our practice includes physical rehabilitation and long-term spinal health maintenance for our patients.
Herniated disc patients should work closely with their surgeon and adhere to a comprehensive recovery plan. When this happens, the patients can expect significant improvements in their symptoms and a return to their normal activities.
Herniated Disc Statistics:
Prevalence:
- 5-20 cases per 1,000 adults annually: This translates to roughly 1.25-5 million new cases in the U.S. each year.
- Most common between ages 30-50: The peak incidence occurs with increased use of the spine and age-related wear and tear.
- More common in men than women: The male-to-female ratio is roughly 2:1.
- Lower back (lumbar discs): Around 95% of symptomatic herniations occur at the L4-L5 or L5-S1 levels.
Outcomes:
- Most herniations resolve without surgery: Approximately 80-90% of cases improve within 6 weeks with conservative management like rest, physical therapy, and pain medication.
- Surgery is only needed in a small percentage: About 10-20% of patients require surgery due to persistent pain or neurological deficits.
Conclusion
It’s important to meet with your spine doctor, monitor your progress, and make any necessary adjustments to your treatment plan. We are experts in herniated disc diagnosis, treatment, and care. Southwest Scoliosis and Spine Institute’s board-certified, fellowship-trained orthopedic doctors, Richard Hostin, MD, Devesh Ramnath, MD, Ishaq Syed, MD, Shyam Kishan, MD, and Kathryn Wiesman, MD, with offices in Dallas, Plano, and Frisco, Texas, possess years of experience treating thousands of patients with complex spine conditions, including herniated discs. Please contact us for any questions or to make your next appointment.
___________________
Citations: Medical News Today: Herniated Disc
Statistical Information Source: National Center for Biotechnology Information:
The medical content on this page has been carefully reviewed and approved for accuracy by the Southwest Scoliosis and Spine Institute’s qualified healthcare professionals, including our board-certified physicians and Physician Assistants. Our team ensures that all information reflects the latest evidence-based practices and meets rigorous standards of medical accuracy, with oversight from our expert spine doctors to guarantee reliability for our patients.
We’re here to help STOP THE PAIN
If you are an adult living with scoliosis or have a child with this condition and need a doctor who specializes in orthopedic surgery,
call the Southwest Scoliosis and Spine Institute at 214-556-0555 to make an appointment today.


