DEGENERATIVE SCOLIOSIS
Degenerative scoliosis describes a sideways curvature of the spine that results from the degeneration of the joints and discs in the spine. Also, this condition and the resulting problems of the spine usually occur gradually as a person ages.
At the Southwest Scoliosis and Spine Institute, our expert Scoliosis Doctors and Surgeons are dedicated to diagnosing and treating spinal problems in children and adults to ensure comprehensive care is tailored to each patient’s needs. With advanced techniques and a compassionate approach, our team diagnoses, treats, and cares for patients suffering from Degenerative Scoliosis.
“At Southwest Scoliosis and Spine Institute, we see adult patients in pain or embarrassed by the curves. Our expertise and experience with complex adult scoliosis make the difference in improving lives.”
Richard Hostin, MD
Reba Dawson
Sadly, Reba’s curves were 65 degrees and causing bone on bone, and therefore, she was in constant pain. In view of this, she opted for surgery. Because of the skill of her surgeon, her pain was gone when she woke up from surgery. Fortunately, the pain never returned and she lives life to the fullest. In her youth, Reba was diagnosed with Scoliosis. As she got older, she learned that she had a double curve and in her 40s she started having a lot of pain. In 2017, she realized that the pain was taking over her life, day and night. Then she found Dr. Richard Hostin. And after that, she made an appointment and started her healing journey. So, “I’m pain-free and feeling amazing!”- Reba Dawson
Degenerative Scoliosis
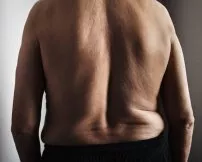 Degenerative Scoliosis occurs in adults and can cause a particularly debilitating condition, which produces terrible pain and progressive curvature of the spine. Untreated cases may manifest as a disfiguring S or C-shaped curve and often a large hump in the back. As they age, patients with this form of scoliosis have increasing difficulty exercising, and their lifestyles are changed and impacted by pain. As the disease progresses, some may experience difficulty breathing and walking.
Degenerative Scoliosis occurs in adults and can cause a particularly debilitating condition, which produces terrible pain and progressive curvature of the spine. Untreated cases may manifest as a disfiguring S or C-shaped curve and often a large hump in the back. As they age, patients with this form of scoliosis have increasing difficulty exercising, and their lifestyles are changed and impacted by pain. As the disease progresses, some may experience difficulty breathing and walking.
When working to provide a diagnosis for a patient’s pain and discomfort, we closely examine each patient’s specific curvature and entire body. So we conduct a thorough physical examination of the back and extensive testing, including specialized low-dose X-rays.
Definition of Degenerative Scoliosis
Degenerative scoliosis generally develops after the age of 50 and is associated with other spinal conditions such as arthritis, disc degeneration, and osteoporosis. The condition is characterized by a side-to-side curvature of the spine, typically in the lumbar (lower back) region. As the spine degenerates, the vertebrae and discs become less stable, which can exacerbate the curvature and lead to nerve compression, causing pain and neurological symptoms.
- Pure degenerative – Scoliosis patients who had straight spines earlier in life but developed curvatures from wear and tear of the aging spine.
- Old idiopathic curves with degenerations – Scoliosis patients who had curves in childhood that increased in curvature later in life.
- Secondary – Scoliosis patients who experienced curves caused by other conditions, such as tumors and fractures.
Causes of Degenerative Scoliosis
The precise causes of degenerative scoliosis or associated spinal osteoarthritis are not known, but the condition is clearly aggravated by daily wear and tear, microtraumas, and repetitive activities that jar the spine, such as using a jackhammer. Less frequently, it is caused by a fall or other trauma. While age-related degeneration is a primary factor, these additional elements can significantly contribute to the onset and progression of the condition.
Symptoms
Upon looking for the cause of pain or discomfort, patients can have a range of symptoms, depending on what causes the condition. Some patients with this condition experience no symptoms, while others experience pain and disability. Degenerative scoliosis symptoms may include:
- Back pain that gets worse while standing (and may get better while lying down)
- Pain in one or both legs
- Numbness and/or weakness in one or both legs.
Why Precise Diagnosis Matters
Degenerative scoliosis is different from adolescent idiopathic scoliosis, and the treatment approach is also different. Understanding the exact type of adult scoliosis is crucial because it helps determine the most effective treatment options. For instance, doctors may recommend surgery in cases where the curvature is severe and causing pain or other complications. By identifying the specific characteristics of scoliosis, healthcare providers can tailor treatment plans to address the individual needs of each patient, ultimately improving outcomes and quality of life. Understanding the patient’s exact type of adult scoliosis is critical for determining an effective treatment plan. This precise identification is essential because:
- Targeted Treatments: It allows for the development of targeted and effective treatments.
- Avoiding Unnecessary Procedures: Accurate diagnosis prevents the application of unnecessary general treatments that may not provide successful outcomes.
- Improving Patient Outcomes: Tailored treatments enhance the quality of life by directly addressing the unique aspects of the condition.
Incorporating a precise diagnostic approach ensures that each patient receives the most appropriate and effective care, designed to mitigate their specific symptoms and challenges.
Questions and Answers
What is Degenerative Scoliosis
Degenerative scoliosis, also known as adult-onset scoliosis, characterizes an abnormal sideways curvature of the spine that occurs in adulthood. Unlike adolescent idiopathic scoliosis, which typically develops during adolescence, the cause of degenerative scoliosis happens with the degeneration of the spinal discs and joints that occurs naturally with age. It often affects older individuals and doctors find it associated with osteoarthritis and spinal stenosis.
What are the Symptoms of Degenerative Scoliosis
The symptoms of degenerative scoliosis can vary from person to person. Common symptoms include back pain, stiffness, and a noticeable curvature of the spine. The pain may worsen with prolonged standing or walking and may be relieved by sitting or lying down. Some individuals may experience leg pain or numbness if the scoliosis is compressing nerve roots or the spinal cord. In severe cases, degenerative scoliosis can lead to spinal instability, balance problems, and difficulty with daily activities.
What are the Treatment Options for Degenerative Scoliosis
The treatment options for degenerative scoliosis depend on the severity of the curvature and the presence of symptoms. Non-surgical treatments such as pain medication, physical therapy, and exercise are often recommended initially to manage symptoms and improve mobility. In cases where conservative measures are not effective, surgical intervention may be considered. Surgery aims to correct the spinal curvature, stabilize the spine, and relieve pressure on nerves or the spinal cord. The specific surgical approach will depend on various factors, including the location and severity of the scoliosis, as well as the overall health and preferences of the individual.
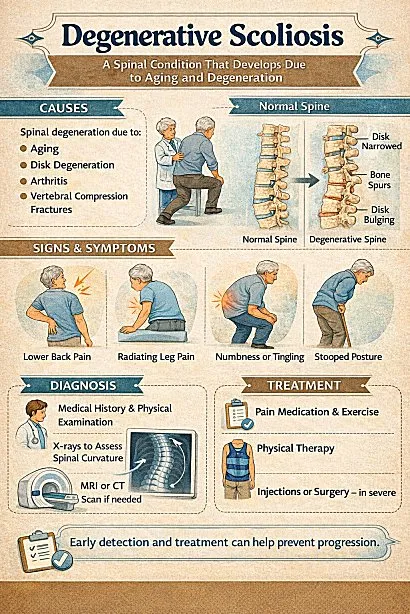
Future Directions in the Treatment of Degenerative Scoliosis
To enhance treatment outcomes for degenerative scoliosis, research is focusing on optimizing bone tissue. One promising area involves bone morphogenic proteins (BMPs), which can aid in bone formation and are already utilized in spinal fusions. Ensuring patients maintain adequate levels of Vitamin D and calcium is also crucial, as these nutrients are vital for bone strength. This can improve the patient’s ability to handle surgical interventions like the insertion of rods and screws. Additionally, researchers are looking at systemic bone-building agents as potential enhancements to spinal fusion success rates.
Advancements in Minimally Invasive Techniques
Minimally invasive spine surgery has gained significant traction over the past decade, particularly for implant cages and lumbar interbody fusions (LIFs). These procedures include:
- Anterior LIF (ALIF)
- Lateral LIF (LLIF)
- Transforaminal LIF (TLIF)
- Posterior LIF (PLIF)
Recent advancements like computer-assisted navigation have revolutionized how surgeons place rods and screws, making procedures more accurate and safer. Robotic-assisted surgeries have further refined these techniques, reducing soft tissue trauma and promoting quicker patient mobility post-surgery. These innovations make minimally invasive approaches preferable for short or straightforward fusions.
Traditional ‘Open’ Approaches
Despite the benefits of minimally invasive techniques, doctors may recommend traditional open surgeries for more complex cases involving extensive spinal decompressions and fusions. These approaches can address the intricate needs of severe degenerative scoliosis cases better than their minimally invasive counterparts.
By integrating these cutting-edge techniques and optimizing overall bone health, the treatment of degenerative scoliosis is poised for significant improvements, enhancing patient outcomes and recovery times.
Diagnosing Degenerative Scoliosis
The diagnosis of Degenerative Scoliosis occurs by combining a physical exam and specialized X-rays. During the physical exam, Dr. Hostin will look at the degree of rotation in the curvature of the spine, as well as other changes in other parts of the body, such as:
- Uneven shoulders
- Rib hump or asymmetry
- Low back hump or asymmetry
- Change in the shape of the waist
- Uneven pelvic bones or hips
Often, these changes do not get noticed while standing and only become visible when the person bends forward. Meanwhile, X-rays provide an important tool for pinpointing the shape and location of the curves, as well as for measuring the degree of the curvature. For instance, the Southwest Scoliosis and Spine Institute uses the revolutionary EOS X-ray imaging system, which allows us to quickly take full-body images of patients in multiple positions while having the lowest possible dose of radiation.
When Does Degenerative Scoliosis Become Serious?

If degenerative scoliosis causes the spinal cord or a nerve root to become impinged, either through stenosis (narrowing of the spinal canal) or severe bending of the spine, nerve function could become jeopardized. Initially, this often feels like a sharp or shock-like pain in the back that radiates down the buttock and/or into the leg, or as tingling or numbness that can radiate down into the leg. Doctors refer to this as sciatica or sciatic pain, and the medical term for this type of radiating pain is radiculopathy. While uncommon, this condition can cause weakness in the legs and/or problems with bladder and bowel control.
Potential Long-Term Complications
Degenerative scoliosis may lead to more severe, long-term complications if not managed effectively:
- Permanent Leg Weakness: Over time, persistent nerve impingement can lead to irreversible damage, significantly affecting mobility and quality of life.
- Bladder/Bowel Control Issues: In some severe cases, nerve damage may disrupt the normal functioning of the bladder and bowels, leading to incontinence.
Understanding these risks highlights the importance of early diagnosis and intervention. It is crucial to address symptoms promptly to minimize the potential for these serious, irreversible complications.
Understanding the Source of Pain in Degenerative Scoliosis
Degenerative scoliosis, a condition characterized by an abnormal, side-to-side curvature of the spine that develops in adulthood, can lead to a variety of symptoms. While it’s easy to assume that the curvature itself is the primary source of discomfort, the main source of degenerative scoliosis pain stems from other factors associated with the condition, not just the physical curvature.
Common Symptoms
- Back Pain and Stiffness: The most noticeable symptoms include persistent back pain and general stiffness in the spinal area. This discomfort often worsens with activities like prolonged standing or walking, and may find relief when sitting or lying down.
- Spinal Curvature: A visible curvature of the spine is a hallmark of degenerative scoliosis, but it is not typically the direct cause of pain.
- Nerve Compression: In some cases, the altered shape of the spine can compress nerve roots or even the spinal cord. This compression can lead to leg pain or numbness, which significantly contributes to the overall pain experienced by the individual.
- Spinal Instability and Balance Issues: In severe cases, the condition can lead to spinal instability. This instability not only exacerbates pain but also creates balance problems, complicating daily activities and mobility.
Each of these symptoms plays a role in the overall experience of pain in degenerative scoliosis. By understanding that the curvature itself is not the primary pain source, individuals and healthcare providers can better target treatments and manage the condition more effectively.
What Factors Can Lead to Increased Surgical-Related Risks In Older Adults With Degenerative Scoliosis
Degenerative scoliosis often occurs in older adults as the spine degenerates over time. The cause points to degenerative disc disease, arthritis of the facet joints, or osteoporosis. This type of scoliosis usually starts after age 50 and is technically known as adult-onset scoliosis. However, it is frequently referred to simply as adult scoliosis. Symptoms of degenerative scoliosis may include back pain and stiffness. Treatment for this condition may involve physical therapy, pain management, and in some cases, surgery.
Idiopathic scoliosis, on the other hand, typically develops in adolescents, and its cause is unknown. It is characterized by an abnormal sideways curvature of the spine. Although it begins during adolescence, doctors may not diagnose idiopathic scoliosis until the individual is an adult, especially if the curvature becomes problematic later. When this happens, doctors may still refer to it as adult scoliosis, even though the correct term is adolescent idiopathic scoliosis. Depending on the severity of the curvature, treatment may involve bracing or surgery.
Understanding Degenerative Scoliosis
Understanding the differences between different types of scoliosis is crucial, especially in terms of their onset and progression. Degenerative scoliosis is associated with the aging process and typically affects individuals over 50, while idiopathic scoliosis is generally observed in adolescents but can go unnoticed until adulthood. This distinction helps in diagnosing and managing the conditions effectively, ensuring that patients receive appropriate and timely care.
Older adults with degenerative scoliosis facing surgery may encounter heightened risks due to several factors:
- Advanced Age
- History of Smoking
- Excess Body Weight
- Existing Health or Medical Issues
Non-Surgical Treatments
When considering treatment for degenerative scoliosis, it’s important to evaluate all options, both surgical and nonsurgical. Nonsurgical treatment options—such as physical therapy, medications, or avoiding strenuous activities—are usually sufficient for managing symptoms and improving the quality of life in many patients. These methods can reduce pain and enhance mobility without the need for surgical intervention.
When deciding on the best course of action for treating degenerative scoliosis, it’s critical to thoroughly discuss all available options with healthcare professionals to determine the most appropriate approach tailored to the individual’s specific condition and needs. As a result of our experience, we use conservative treatments for degenerative scoliosis, and they include medication, exercise, and bracing to support the spine.
If the doctor finds osteoporosis present, then treatment of this disease may also slow the progression of scoliosis. In addition, the current treatment includes increasing calcium and vitamin D intake and weight-bearing exercises.
Medication
Our doctors prescribe mild pain medicines to use as needed. Usually, we do not prescribe strong pain medications. In many cases, we treat degenerative scoliosis by combining physical therapy and pain management. However, if these measures are insufficient, our doctors may recommend oral medications to manage pain and inflammation. Your doctor will prescribe the correct medication based on your professional evaluation and include:
- Anti-Inflammatory Drugs that are sold over the counter or by prescription
For patients experiencing radicular symptoms (pain that radiates along a nerve due to inflammation or injury), doctors will prescribe medications to help reduce nerve inflammation or “overactivity”. These include:
- Managing nerve pain with drugs.
In rare cases where pain becomes extreme, doctors may prescribe stronger pain medications. These are typically prescribed for only a brief period, such as the week leading up to surgery or a few weeks following surgery. If the patient’s curve progresses to the point that they feel pain or have difficulty breathing, doctors may recommend surgery as the best option.
Physical Therapy and Exercise
A physical therapist or another qualified medical professional can help develop an exercise and stretching routine to meet the patient’s specific needs. Physical therapy can help keep the soft tissues and joints limber as well as strengthen the targeted muscles.
The goal of physical therapy is to help
- learn ways to manage the symptoms of the condition
- improve spine posture
- Stabilize the spine
Exercise does not help to stop scoliosis. However, it can help by addressing pain, posture, and spine stability. Your doctor may schedule therapy sessions for four to six weeks.
Bracing
The use of a spinal brace may provide some pain relief, but in adults, the brace will not cause the spine to straighten. Once you have reached skeletal maturity, bracing is used for pain relief rather than prevention. If the doctor finds a difference in the length of your legs (or if scoliosis causes you to walk somewhat crooked), special shoe inserts, called orthotics, or a simple shoe lift may reduce your back pain.
Learn more about braces used to treat back problems.
Injections
Epidural steroid injections can reduce inflammation, and facet-block injections can prevent pain signals from reaching the brain. These types of injections deliver anti-inflammatory medication directly to the affected area in the spine.
Surgery for Degenerative Scoliosis
Degenerative scoliosis, also known as adult-onset scoliosis, is a condition that typically develops in older adults due to the wear and tear of the spine over time. Unlike adolescent scoliosis, which is often idiopathic (without a known cause), degenerative scoliosis arises from the degeneration of the spinal discs and joints, leading to a curvature of the spine. This condition can cause significant pain, discomfort, and functional limitations, prompting some individuals to consider surgical intervention when conservative treatments fail to provide relief.
Indications for Surgery
Surgery for degenerative scoliosis is typically considered when:
- Pain is Severe and Debilitating: Persistent pain that does not respond to non-surgical treatments like physical therapy, medication, or injections.
- Progressive Neurological Symptoms: Symptoms such as numbness, weakness, or loss of bowel/bladder control due to nerve compression.
- Spinal Instability: Significant spinal instability that may lead to worsening of the curve or further complications.
- Cosmetic Concerns: Although less common, some patients may seek surgery for cosmetic reasons if the curvature is severe and noticeable.
Types of Surgical Procedures for Degenerative Scoliosis
Decompression Surgery
- Purpose: Relieves pressure on the spinal nerves.
- Procedure: Surgeons remove parts of the vertebrae (such as the lamina or bone spurs) to create more space for the spinal nerves.
- Use Case: Often used in patients where nerve compression (leading to pain, numbness, or weakness) is a primary concern.
- Outcome: Decompression alone may not correct the curvature, but can significantly reduce pain caused by nerve compression.
Spinal Fusion Surgery
- Purpose: Stabilizes the spine and prevents further curvature progression.
- Procedure: Involves joining two or more vertebrae together using bone grafts and metal hardware (such as rods and screws). Over time, the bones fuse into a single solid mass.
- Use Case: This is the most common surgery for correcting degenerative scoliosis, particularly in cases with significant curvature or instability.
- Outcome: Spinal fusion aims to correct the deformity, reduce pain, and stabilize the spine, preventing further degeneration.
Instrumented Fusion
- Purpose: Corrects spinal alignment and maintains correction over time.
- Procedure: Similar to spinal fusion but includes the use of metal implants (rods, screws, cages) to hold the spine in the correct position while the bones fuse.
- Use Case: Often used in conjunction with decompression surgery when both nerve compression and spinal instability are present.
- Outcome: This procedure provides immediate stability and allows for better correction of the spinal curve.
Osteotomy
- Purpose: Corrects rigid or severe curves by removing a wedge-shaped section of bone from a vertebra.
- Procedure: The osteotomy allows for the realignment of the spine to a more natural position. The remaining vertebrae are then fused to maintain this correction.
- Use Case: Utilized in patients with rigid curves or when previous surgeries have resulted in a loss of flexibility.
- Outcome: Provides significant correction in severe or rigid deformities, but is more complex and carries a higher risk.
Interbody Fusion
- Purpose: Restores disc height and alignment between vertebrae.
- Procedure: Involves removing a damaged intervertebral disc and replacing it with a bone graft or synthetic spacer. The fusion occurs between the vertebral bodies rather than just at the back of the spine.
- Use Case: Often combined with other fusion techniques, particularly in cases where disc degeneration has significantly contributed to scoliosis.
- Outcome: Helps to restore spinal alignment and relieve nerve compression while contributing to overall spinal stability.
Minimally Invasive Spinal Surgery (MISS)
- Purpose: Reduces the invasiveness of traditional open surgeries.
- Procedure: Surgeons use specialized instruments and small incisions to access the spine. Techniques like minimally invasive spinal fusion and decompression fall under this category.
- Use Case: Ideal for patients who may not tolerate extensive surgery due to age or other health conditions.
- Outcome: Shorter recovery times, less blood loss, and reduced risk of infection compared to open surgery, with similar outcomes in terms of pain relief and stability.
Risks and Considerations
While surgery can provide significant relief from pain and correct spinal deformity, it is not without risks. Potential complications include:
- Infection: Surgical site infections, though minimized by modern techniques and antibiotics.
- Hardware Failure: The metal rods and screws used in fusion surgeries can sometimes loosen or break.
- Non-Union: In some cases, the bones may not fuse properly, requiring additional surgery.
- Adjacent Segment Disease: Degeneration can occur above or below the fused segments, potentially leading to additional problems.
- Nerve Damage: Although rare, there is a risk of nerve injury leading to weakness, numbness, or even paralysis.
Recovery and Rehabilitation
Post-surgery, patients typically require a period of rehabilitation to regain strength and mobility. Physical therapy plays a crucial role in recovery, focusing on exercises that strengthen the core muscles and improve overall spinal alignment. The recovery period can vary widely depending on the type and extent of surgery, with full recovery often taking several months.
Conclusion
Surgery for degenerative scoliosis is a major decision that requires careful consideration of the potential benefits and risks. It is typically reserved for cases where conservative treatments have failed, and the patient’s quality of life is significantly impacted by pain or neurological symptoms. The choice of surgical procedure depends on various factors, including the severity of the curvature, the presence of nerve compression, and the overall health of the patient. Advances in surgical techniques have made it possible to achieve better outcomes with fewer complications, offering hope to those affected by this debilitating condition.
Results for Degenerative Scoliosis Treatments
For the majority of patients with degenerative scoliosis, pain relief can occur through nonsurgical approaches. These might include physical therapy, medications, and injections. However, when surgery becomes necessary, outcomes can vary depending on the specific underlying issues. Patients who undergo decompression for conditions like spinal stenosis or radicular symptoms often see significant improvement. Those experiencing intermittent pain, numbness, or weakness before surgery typically benefit the most.
On the other hand, individuals who have back pain and receive spinal fusion tend to achieve results similar to those with degeneration but without curvature in their spines. A thorough evaluation is crucial, particularly for older adults. Factors such as pre-existing medical conditions and current medications must be carefully considered. This ensures that patients can tolerate surgery and participate in rehabilitation effectively.
The Southwest Scoliosis and Spine Institute specializes in helping patients with Scoliosis and complex Spine Conditions.
If you think you or a loved one might need surgery to correct scoliosis or any other kind of complex spine surgery, you should contact a surgeon who performs these kinds of complicated and specialized procedures all the time. Finally, the Southwest Scoliosis and Spine Institute’s board-certified, fellowship-trained orthopedic surgeons, Richard Hostin, MD, Devesh Ramnath, MD, Ishaq Syed, MD, Shyam Kishan, MD, and Kathryn Wiesman, MD, should be your first choice as they are scoliosis and spine doctors who are very frequently recommended by other doctors.
They’ve performed more than 16,000 successful spine surgeries. Significantly, they have also helped more than 100,000 patients get back to living a normal, pain-free life. So, if doctors advise you that nothing can help, please call us at Southwest Scoliosis and Spine Institute. We have offices in Dallas, Plano, and Frisco, Texas. Finally, with our skills, knowledge, abilities, expertise, and experience, we can offer hope, remove pain, and provide better health. If you need help, call us for an evaluation at 214-556-0555 or visit our contact page today!
____________________
Citation: Health Central – Degenerative Scoliosis
The medical content on this page has been carefully reviewed and approved for accuracy by the Southwest Scoliosis and Spine Institute’s qualified healthcare professionals, including our board-certified physicians and Physician Assistants. Our team ensures that all information reflects the latest evidence-based practices and meets rigorous standards of medical accuracy, with oversight from our expert spine doctors to guarantee reliability for our patients.
“After surgery, patients go to the intensive care unit to obtain focused nursing care,” says Dr. Hostin. “It really is very comforting for both the patient and their family to know that there’s one nurse assigned to take care of the patient’s needs.”
If you experience pain from scoliosis, we can help. Call the Southwest Scoliosis and Spine Institute at 214-556-0555.


