DEGENERATIVE DISC DISEASE
Degenerative Disc Disease is normally caused by aging, wear and tear on the discs in your spine. Not everyone’s discs wear out at the same rate. When your discs lose their cushioning, fragment, or herniate, this can cause limited movement and pain.
At the Southwest Scoliosis and Spine Institute, our expert Degenerative Disc Disease Doctors are dedicated to diagnosing and treating spinal problems and ensuring comprehensive care tailored to each patient’s needs. With advanced techniques and a compassionate approach, our team is here to diagnose, treat and care for patients suffering from Degenerative Disc Disease
The Southwest Scoliosis and Spine Institute has expert doctors and surgeons to treat degenerative disc disease.
Degenerative Disc Disease
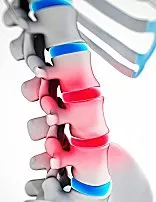 Degenerative disc disease (DDD) is a common condition affecting the spine, particularly in the lower back and neck. Also, it occurs when the discs between the vertebrae (spinal bones) wear down over time, causing pain, stiffness, and other symptoms. While aging is the most significant contributing factor, genetics, injuries, and other lifestyle factors can also cause DDD.
Degenerative disc disease (DDD) is a common condition affecting the spine, particularly in the lower back and neck. Also, it occurs when the discs between the vertebrae (spinal bones) wear down over time, causing pain, stiffness, and other symptoms. While aging is the most significant contributing factor, genetics, injuries, and other lifestyle factors can also cause DDD.
As individuals age, spinal discs lose hydration and elasticity. This is primarily due to a decrease in proteoglycan content, the component responsible for retaining water within the disc. According to the National Institutes of Health (NIH), this loss of structural integrity reduces the disc’s ability to absorb shock, leading to gradual “shrinking” of the spinal column.
What Happens in Degenerative Disc Disease
As a consequence, the spine may become less flexible, leading to stiffness, pain, and potential complications such as nerve compression or spinal instability. Despite its name, this condition is not actually a disease. Factors such as genetics, lifestyle choices, and repetitive stress on the spine can also contribute to the development and progression of degenerative disc disease. Proper management, including exercise, lifestyle modifications, and sometimes surgical intervention, can help alleviate symptoms and improve the quality of life for individuals affected by this condition.
Unfortunately, this degeneration can lead to various problems, including:
- Bulging Discs: As the pressure increases within the disc, it may bulge outward, putting pressure on the surrounding nerves.
- Slipped Discs: In severe cases, the inner core of the disc can push through a tear in the outer ring, causing a herniated disc. This can severely compress the nerves, leading to pain, weakness, and numbness.
- Spinal Stenosis: The narrowing of the spinal canal, which the American Academy of Orthopaedic Surgeons (AAOS) identifies as a leading cause of leg pain and weakness in older adults.
Questions and Answers
What is Degenerative Disc Disease
Degenerative disc disease refers to a condition characterized by the gradual breakdown of intervertebral discs in the spine, leading to pain, stiffness, and reduced flexibility in the affected area.
What are the Symptoms of Degenerative Disc Disease
The symptoms of degenerative disc disease can vary, but often include back pain, stiffness, and reduced flexibility. Some individuals may also experience nerve pain, tingling, or weakness in the arms or legs.
What are the Treatment Options for Degenerative Disc Disease
Treatment for degenerative disc disease typically begins with conservative measures such as pain medication, physical therapy, or chiropractic care. In some cases, our doctors with offices in Dallas, Plano, and Frisco, TX, may recommend surgery to address severe pain or other symptoms. At present, a cure for degenerative disc disease does not exist, so treatment is typically focused on managing symptoms and improving quality of life.
What causes Degenerative Disc Disease?
Firstly, aging primarily triggers Degenerative Disc Disease. Spinal discs lose water content and flexibility after age 40. This reduces shock absorption between vertebrae. Next, tears or cracks may form in discs. Additionally, genetics play a role. Certain biomarkers affect disc structure and inflammation. Moreover, traumatic injuries like falls can damage discs. Furthermore, lifestyle factors increase risk. Smoking, obesity, diabetes, or low estrogen in postmenopausal women accelerate degeneration. Also, environmental stressors contribute. Heavy lifting, repetitive motions, or contact sports strain discs. Lastly, while aging starts the process, these factors worsen it faster.
Prognosis of Degenerative Spine Disease
Degenerative disc disease (DDD), despite its ominous-sounding name, offers hope for effective management and improved quality of life. The following are the positive aspects of treating this condition:
- Conservative Approaches: Physical therapy, rest, and activity modification form the initial line of defense. These strategies help strengthen core muscles, enhance mobility, and alleviate pain.
- Pain Management: Medications such as Ibuprofen and Acetaminophen have crucial roles in managing discomfort. These analgesics provide relief and allow individuals to resume daily activities more easily.
- Innovative Techniques: For those who need more targeted intervention, procedures like facet joint injections — where steroids and local anesthetics are injected near the damaged disc — can effectively relieve pain
- Hope for Mobility: While DDD is a natural part of aging, it need not be debilitating. With the right care, individuals can continue to move, bend, and twist comfortably. Devesh Ramnath, MD
Understanding Degenerative Disc Disease
Before we talk more about this condition, please know that almost everyone’s discs break down over time, but not everyone will undergo pain because of it. If worn-out spinal discs are the reason that a person is suffering from pain, then that person has degenerative disc disease.
Anatomy
To better understand DDD, let’s define the two affected parts of the body:
- Vertebrae: The spine is made up of 24 individual bones called vertebrae, stacked on top of each other. Particularly, they provide structure, support, and protection for the spinal cord and nerves.
- Spinal Discs: Between each vertebra lies a disc, acting as a cushion and shock absorber for the spine. Overall, these discs are composed of a tough outer ring (annulus fibrosus) and a soft inner core (nucleus pulposus).
Causes of Degenerative Disc Disease
A healthy intervertebral disc has a great deal of water in the nucleus pulposus (the center portion of the disc). Furthermore, the water content gives the nucleus a spongy quality, allowing it to absorb spinal stress. Excessive pressure or injuries to the disc can cause injury to the annulus (the outer ring of tough ligament material). Usually, the annulus gets injured first, causing small tears in the ligament material. Upon the healing of the tear, they form scar tissue, which does not have the strength of normal ligament tissue. As more scar tissue forms, the annulus becomes weaker over time. Unfortunately, this can lead to damage to the nucleus pulposus. Thus, it begins to lose its water content and dry up.
As the nucleus loses its water content, it collapses, allowing the two vertebrae above and below to move closer to one another. Then, this results in a narrowing of the disc space between the two vertebrae. As this shift occurs, the facet joints (located at the back of the spine) are forced to shift. Shifting changes the way the facet joints work together and can cause problems as well.
Degenerative Disc Disease Risk Factors
Several risk factors contribute to the development of degenerative disc disease (DDD), a common condition affecting the spinal discs. Age is the primary risk factor, as DDD typically progresses with advancing years due to the natural wear and tear on the spine. Genetics also plays a significant role, as individuals with a family history of DDD may develop this condition. Lifestyle factors such as smoking, obesity, and poor posture can accelerate disc degeneration. This occurs by impairing blood flow to the discs and increasing mechanical stress on the spine. Certain occupations or activities that involve repetitive lifting, bending, or twisting motions may also contribute to disc degeneration over time.
Additionally, trauma or injury to the spine, such as from car accidents or sports injuries, can accelerate the degenerative process. Overall, a combination of age, genetics, lifestyle factors, and environmental influences contributes to an individual’s risk of developing degenerative disc disease. Understanding these risk factors can help guide preventive measures and interventions to mitigate the progression of the condition and improve spinal health.
Types of Degenerative Disc Disease
The following are the different types of Degenerative Disc Disease
Lumbar Degenerative Disc Disease:
Lumbar degenerative disc disease is a condition characterized by the deterioration of the intervertebral discs in the lower back region, specifically in the lumbar spine. These discs act as shock absorbers between the vertebrae, providing flexibility and cushioning during movement. With age or due to wear and tear, the discs can lose hydration and elasticity, leading to a reduction in disc height and integrity. As a result, individuals may experience symptoms such as lower back pain, stiffness, radiating pain into the buttocks or legs (sciatica), numbness or tingling sensations, and sometimes weakness in the legs. Lumbar degenerative disc disease can significantly impact the quality of life, limiting mobility and causing discomfort during daily activities.
Cervical Degenerative Disc Disease:
Cervical degenerative disc disease is a condition characterized by the deterioration of the intervertebral discs in the neck region. Specifically, this means in the cervical spine. These discs serve as cushions between the vertebrae, providing support and allowing for smooth movement of the neck. Over time, the discs may lose hydration and elasticity, leading to a decrease in disc height and function. The Scoliosis Research Society (SRS) notes that cervical degeneration can lead to radiating pain or numbness in the arms and hands. Cervical degenerative disc disease can also cause limitations in neck movement and may contribute to the development of cervical osteoarthritis or spinal stenosis. Proper diagnosis and management are essential to alleviate symptoms and prevent further progression of the condition.
Common Symptoms and Associated Conditions of Degenerative Disc Disease
The most common early symptom of degenerative disc disease usually occurs in patients with back pain or neck pain. Common areas affected are the cervical and lumbar spine. The pain often spreads to the buttocks and upper thighs, as well. When doctors refer to degenerative disc disease, they are usually referring to a combination of problems in the spine that “start” with damage to the disc, but eventually begin to affect all parts of the spine. Problems thought to arise from the degenerating disc itself include discogenic pain and bulging discs.
Discogenic Pain
Discogenic pain refers to a term that back specialists use when referring to pain caused by a damaged intervertebral disc. A degenerating disc may cause mechanical (or structural) pain. As the disc begins to degenerate, the disc itself becomes painful. Movements that place stress on the disc can result in back pain that appears to come from the disc. This occurs with other body parts that become injured, such as a broken bone or a cut in the skin. When these types of injuries occur and there is no movement, the pain will not occur. However, if you move them, they will hurt.
Discogenic pain usually causes pain felt in the lower back. It may also feel like the pain comes from your buttock area and even down into the upper thighs. The experience of feeling pain in an area away from the real cause is common in many areas of the body, not just the spine. For instance, a person with gallstones may feel pain in the shoulder, or a person experiencing a heart attack may feel pain in the left arm. This refers to the radiation of the pain. When pain comes from spine problems, it can occur in different areas of the body, including the back.
Bulging Discs
Bulging discs are fairly common in both young adults and older people. They are not the cause of panic. Abnormalities, such as bulging or protruding discs, are seen at high rates on MRIs in patients both with and without back pain. Some discs most likely begin to bulge as a part of both the aging process and the degeneration process of the intervertebral disc. A bulging disc does not necessarily indicate that a person has a medical emergency.
A bulging disc only becomes serious when it bulges enough to cause a narrowing of the spinal canal. If there are bone spurs present on the facet joints behind the bulging disc, the combination may cause a narrowing of the spinal canal in that area. This often refers to segmental spinal stenosis.
Diagnosis of Degenerative Disc Disease
Before your doctor can diagnose your condition and design a treatment plan, he or she must obtain a complete health history and conduct a physical exam. However, there are so many possible causes of pain that doctors need to determine the root of the problem.
You may take a variety of diagnostic tests. For instance, the tests are chosen based on what your doctor suspects is causing your pain. Your doctor may order an X-ray and or a magnetic resonance imaging MRI scan to help him diagnose you correctly. If your doctor suspects disc degeneration, X-rays can verify a decrease in the height of the space between vertebrae, bone spurs, facet hypertrophy (enlargement), and instability during flexion or extension of limbs. An MRI can verify the loss of water in a disc, facet joint hypertrophy, stenosis, or a herniated disc. Our expert spine doctors will identify the stage of degenerative disc disease.
The four stages of degenerative disc disease:
Initial Stage
- This is the initial stage and often shows no symptoms.
- The discs begin to lose some of their height and flexibility, but the overall structure remains intact.
- Some people may experience mild back pain or stiffness, especially after prolonged sitting or physical activity.
Second Stage: Dehydration
- In this stage, the discs start to lose water content, causing them to become thinner and less effective at cushioning the vertebrae.
- This can lead to increased pain and stiffness in the back or neck.
- The pain may worsen with activity and improve with rest.
Third Stage: Stabilization
- The body attempts to repair the damaged discs by forming tiny bony growths (osteophytes) around the vertebrae, which can cause
- These osteophytes can narrow the spinal canal and put pressure on nerves, causing pain, numbness, and weakness in the arms or legs (radiculopathy).
- The pain may be constant or come and go.
Fourth Stage: Collapse
- This is the most advanced stage of DDD.
- The discs become severely damaged and lose most of their height.
- The vertebrae may rub together, causing significant pain and disability.
- In some cases, the spinal cord or nerves may become severely compressed, leading to muscle weakness, numbness, and even bowel or bladder dysfunction.
It’s important to note that not everyone with DDD will progress through all four stages. The rate of progression can vary depending on individual factors such as genetics, lifestyle habits, and severity of the initial disc damage. Early diagnosis and treatment can help slow the progression of DDD and manage the symptoms.
Treatment Options for Degenerative Disc Disease
Treatment options will depend on the seriousness of your condition, and some problems need immediate attention — even surgery. For the vast majority of back problems, surgery is not considered, and in some instances, doing nothing will make it better. In most cases, simple conservative therapies, such as mild pain medications and rest, are effective in relieving the immediate pain.
The overall goal of Degenerative Disc Treatment:
- Make you comfortable as quickly as possible
- Design a spine-care program to reduce further degeneration
- Get you back to normal activity promptly
Consequently, the more you know about how your back works and what you can do to prevent further injury, the less likely it is that further injuries will occur.
Medications
Your doctor will most likely recommend over-the-counter pain relievers. These medications are typically recommended for mild pain, and they also help with swelling and inflammation. For severe pain, the doctor may prescribe narcotics. Prescription pain medicine is usually prescribed for short-term pain. Patients must take pain medicine as directed by their doctor.
In addition to these general pain relief options, here’s a detailed breakdown of some of the specific medications commonly used to manage symptoms of DDD:
- Non-steroidal anti-inflammatory drugs (NSAIDs) such as aspirin are particularly effective for reducing inflammation that can cause pain.
- Acetaminophen (e.g., Tylenol) relieves pain without the anti-inflammatory effects.
- Antidepressants can be prescribed not only for their mood-stabilizing properties but also for their effectiveness in pain relief in some chronic conditions.
- Muscle relaxants help alleviate muscle spasms that are often a symptom of DDD.
Each medication type serves a specific function in managing the disease, and your doctor will provide guidance on which medication or combination of medications will become most effective for your specific symptoms.
Specific Rest
Immediately after a back injury, you should rest because it takes the pressure off your spine. Also, it provides all you need to feel better. Of course, you should rest in a comfortable position on a firm mattress. When you place a pillow under your knees, it can also help relieve pain. Then do not stay in bed for several days. However, bed rest for more than two or three days can weaken the back muscles, making the problem worse instead of better.
Even though you may still feel some pain, a gradual return to normal activities is good for your muscles. In most cases of sudden back pain, the sooner you start moving again, the sooner your back pain will improve. If you are sent to see a physical therapist, the first part may teach you methods to take the stress off your back while remaining as active as possible. Taking short periods of rest, combined with brief exercises designed to reduce your pain, does help.
Physical Therapy and Exercise
 Your doctor may have you work with a physical therapist. A well-rounded rehabilitation program assists in calming pain and inflammation, improving your mobility and strength, and helping you do your daily activities with greater ease and ability.
Your doctor may have you work with a physical therapist. A well-rounded rehabilitation program assists in calming pain and inflammation, improving your mobility and strength, and helping you do your daily activities with greater ease and ability.
Therapy visits are designed to help control symptoms, enabling you to begin moving and exercising safely and easily. Regular exercise is the most basic way to combat back problems. Consider it part of a long-term health management and risk reduction program. Exercises focus on improving the strength and coordination of the lower back and abdominal muscles. The emphasis of therapy helps you learn to take care of your back through safe exercise and self-care when symptoms flare up. Scheduling of therapy sessions can occur two to three times each week for up to six weeks.
The goals of physical therapy are to help you:
- Learn ways to manage your condition and control symptoms
- Maintain appropriate activity levels
- learn correct posture and body movements to reduce back strain
- Maximize your flexibility and strength
Learn more about spinal rehabilitation.
Epidural Steroid Injection
An epidural steroid injection (ESI) can relieve the pain of stenosis and irritated nerve roots, as well as decrease inflammation. Injections can also help reduce swelling from a bulging or herniated disc. The steroid injections are a combination of cortisone (a powerful anti-inflammatory steroid) and a local anesthetic/ The ESI is administered through the back into the epidural space. ESIs are not always successful in relieving symptoms of inflammation. They are used only when conservative treatments have failed.
Learn more about spinal injections.
Radiofrequency Neurotomy
Radiofrequency neurotomy, also known as radiofrequency ablation, is a minimally invasive procedure used to alleviate chronic back pain associated with degenerative disc disease (DDD). During the procedure, a specialized needle is inserted near the affected spinal nerves under fluoroscopic guidance. Radiofrequency energy is then delivered through the needle to create a lesion on the nerve, disrupting its ability to transmit pain signals to the brain. By targeting the nerves responsible for transmitting pain from the degenerated discs, radiofrequency neurotomy can provide significant pain relief and improve overall function and mobility. While not a cure for DDD, radiofrequency neurotomy can offer long-lasting relief from symptoms, allowing patients to participate in physical therapy and other rehabilitative measures more effectively. It is often considered when conservative treatments such as medication and physical therapy have been unsuccessful in managing DDD-related back pain.
Surgery
There are several surgical procedures that doctors use to help patients with degenerative disc disease, depending on the severity and location of the disease. Some common surgical procedures include:
- Spinal Fusion: The Spinal fusion procedure combines two or more vertebrae in the spine by fusing them using bone grafts, metal plates, or screws. This procedure can help stabilize the spine and relieve pain caused by degenerative disc disease.
- Artificial Disc Replacement: Artificial disc replacement is a procedure in which a damaged disc in the spine is replaced with an artificial disc. This procedure can help restore mobility and reduce pain caused by degenerative disc disease.
- Discectomy: Discectomy is a surgical procedure in which the damaged portion of a disc in the spine is removed. This procedure can help relieve pressure on the nerves and reduce pain caused by degenerative disc disease.
- Foraminotomy: Foraminotomy is a surgical procedure in which the opening in the vertebrae where the nerves exit the spinal column is enlarged to relieve pressure on the nerves. This procedure can help reduce pain caused by degenerative disc disease.
It is important to note that surgery is typically considered a last resort for treating degenerative disc disease. Conservative measures such as pain medication, physical therapy, and lifestyle modifications are often recommended first. Additionally, each case is unique and requires a thorough evaluation by a doctor to determine the most appropriate treatment plan.
Patient Management and Lifestyle Adjustments
While DDD is a chronic condition that cannot be completely cured, effective strategies can help alleviate symptoms. By making good choices, people can improve their overall spinal health. Here, we explore a comprehensive approach to patient management, encompassing various lifestyle modifications, therapies, and preventive measures.
Managing Weight:
Excess weight places additional stress on the spine, exacerbating DDD symptoms. Therefore, maintaining a healthy weight through a balanced diet and regular exercise is essential. Focus on eating nutrient-rich foods, such as fruits, vegetables, lean proteins, and whole grains. Limit processed foods and sugary beverages.
Getting Massages:
Massage therapy can provide temporary relief by reducing muscle tension, improving circulation, and promoting relaxation. Targeted massage techniques can help alleviate pain and stiffness associated with DDD. This makes massage a valuable adjunct to other treatment modalities.
TENS Machines:
Transcutaneous electrical nerve stimulation (TENS) machines deliver low-voltage electrical impulses to the affected area, effectively blocking pain signals from reaching the brain. TENS therapy can provide symptomatic relief for individuals with DDD, offering a non-invasive and drug-free option for pain management.
Improving Posture:
Maintaining proper posture is crucial for reducing strain on the spine and preventing further degeneration of the discs. Practice good posture habits, such as sitting up straight, avoiding slouching, and supporting the lower back while sitting or standing.
Exercises:
Regular exercise is vital for strengthening the muscles that support the spine, improving flexibility, and enhancing overall spinal health. Low-impact activities such as walking, swimming, and cycling are excellent choices for individuals with DDD. Additionally, targeted exercises focusing on core strength, flexibility, and posture can help alleviate symptoms and prevent further deterioration of the discs.
Hot and Cold Therapy:
Alternating between hot and cold therapy can provide relief from DDD-related pain and inflammation. Apply heat packs or warm compresses to the affected area to relax muscles and increase blood flow. Cold therapy, such as ice packs or cold packs, can help reduce swelling and numbness.
Not Smoking:
Smoking has been linked to accelerated disc degeneration and impaired healing of spinal tissues. Quitting smoking can significantly improve outcomes for individuals with DDD, as it reduces inflammation, improves blood flow, and promotes tissue repair.
Not Lifting Heavy Things:
Avoid lifting heavy objects or engaging in activities that require repetitive bending and twisting of the spine. Use proper lifting techniques, such as bending at the knees and keeping the back straight, to minimize strain on the spine.
Not Drinking Alcohol:
Excessive alcohol consumption can contribute to dehydration and inflammation, exacerbating DDD symptoms. Limit alcohol intake or avoid it altogether to support spinal health and overall well-being.
Not Sitting for Long Periods:
Prolonged sitting can place excessive pressure on the spinal discs and contribute to worsening DDD symptoms. Take frequent breaks to stand, stretch, and walk around, especially if you have a desk job or spend long hours sitting.
Avoiding High-Impact Sports:
Engaging in sports or activities that involve running, jumping, twisting, and other high-impact movements can exacerbate DDD symptoms and increase the risk of injury. Choose low-impact exercises and activities that are gentle on the spine, such as swimming, yoga, or tai chi.
In conclusion, effective DDD management requires a comprehensive approach that addresses various aspects of lifestyle, therapy, and prevention. By implementing these strategies, individuals with DDD can alleviate symptoms, improve spinal health, and enhance their overall quality of life. It is essential to consult with one of the Degenerative Disc Disease Doctors at the Southwest Scoliosis and Spine Institute to develop a personalized treatment plan tailored to your specific needs. With dedication and commitment to self-care, individuals with DDD can effectively manage their condition and enjoy life. So call our office and make an appointment at either the Dallas, Plano, or Frisco, Texas offices.
Prevention of Degenerative Disc Disease
Degenerative disc disease (DDD) is a condition that affects the intervertebral discs, which are the cushions that sit between the vertebrae in the spine. As we age, the discs naturally lose water and flexibility, which can lead to several problems, including:
- Reduced disc height
- Disc herniation
- Bone spur formation
- Narrowing of the spinal canal (spinal stenosis)
The above changes can put pressure on the spinal nerves, causing pain, numbness, and weakness. While there is no cure for DDD, there are several things you can do to prevent or slow the progression of the disease.
Here are some tips:
- Maintain a healthy weight. Excess weight puts additional stress on the spine, which can accelerate the degeneration of the discs.
- Exercise regularly. Exercise helps to strengthen the back muscles and improve flexibility. Certainly, people should aim for at least 30 minutes of moderate-intensity exercise most days of the week.
- Practice good posture. Poor posture can put a strain on the spine and increase the risk of injury. When standing, keep your shoulders back and your chest high. When sitting, make sure your feet are flat on the floor and your back is supported.
- Avoid smoking. Smoking can damage the discs and make them more susceptible to degeneration.
- Lift heavy objects properly. When lifting heavy objects, bend at the knees and keep your back straight. Lastly, avoid twisting your back while lifting.
If you have a job that requires you to sit or stand for long periods, take breaks to move around and stretch your back. You may also want to consider using a lumbar support pillow to help maintain your spinal curve.
If you experience any of the symptoms of DDD, such as back pain, stiffness, numbness, and weakness in the arms or legs, it is important to see a doctor to get a diagnosis and discuss treatment options.
Here are some additional tips for preventing DDD:
- Eat a healthy diet. Eating a healthy diet can help to maintain your overall health and well-being, and it may also help to reduce inflammation and protect your discs. Make sure to eat plenty of fruits, vegetables, and whole grains.
- Get enough sleep. Sleep is essential for healing and repair. Aim for 7-8 hours of sleep per night.
- Manage stress. Stress can contribute to muscle tension and pain. Find healthy ways to manage stress, such as exercise, yoga, or meditation.
By following the above-mentioned tips, you can help prevent or slow the progression of DDD and maintain a healthy spine.
Degenerative Disc Disease Statistics:
Prevalence:
- Incredibly common, especially with age:
- Roughly 40% of adults over 40 have at least one degenerated disc.
- By age 80, this jumps to 80%.
- Degeneration is considered a natural part of aging, similar to wrinkles.
- Increases globally: Affects 266 million individuals worldwide each year.
- Varies geographically: Highest prevalence in Europe (5.7%), lowest in Africa (2.
- Gender differences: Generally affect women more than men. One study showed a 34.7% prevalence in women vs. 18.1% in men.
Impact:
- Leading cause of back pain: Estimates suggest up to 80% of low back pain stems from disc degeneration.
- Significant economic burden: Costs billions of dollars annually in healthcare and lost productivity.
- Reduced quality of life: Can limit mobility, daily activities, and overall well-being.
Specific Conditions:
- Spinal stenosis: A narrowing of the spinal canal due to disc degeneration, affecting 103 million people globally annually.
- Spondylolisthesis: When a vertebra slips forward on another, it impacts 39 million individuals worldwide each year.
Other statistics:
- Disc degeneration often starts before symptoms appear, even in adolescents.
- Degeneration may progress slowly or more rapidly, depending on individual factors.
- Not everyone with degenerative discs experiences pain or limitations.
- Various risk factors contribute, including genetics, age, smoking, and obesity.
Statistic sources:
Why Choose a Degenerative Disc Disease Doctor at the Southwest Scoliosis and Spine Institute
 The spine is the specialty of our doctors and surgeons at the Southwest Scoliosis and Spine Institute. The physicians understand your concerns, can answer your questions regarding your condition, and know how to use their specialized knowledge and advanced training to assist you with Degenerative Disc Disease.
The spine is the specialty of our doctors and surgeons at the Southwest Scoliosis and Spine Institute. The physicians understand your concerns, can answer your questions regarding your condition, and know how to use their specialized knowledge and advanced training to assist you with Degenerative Disc Disease.
Please meet our Specialists: Richard Hostin, MD, Devesh Ramnath, MD, Ishaq Syed, Shyam Kishan, MD, and Kathryn Wiesman, MD. They are all board-certified in spinal conditions, have many years of training and experience in Spine and Back Pain for kids, adolescents, and adults, and can help their patients get back to living the life they enjoy.
A few of the many reasons why patients choose the Southwest Scoliosis and Spine Institute.
- Expertise in the spine: The team of specialists is recognized as spine experts. They specialize in the diagnosis and treatment of spinal conditions, ensuring the best possible care for their patients.
- Cutting-edge technology: Our practice uses advanced imaging technology and techniques to diagnose and treat a wide range of conditions. In addition, we use minimally invasive procedures that reduce pain and promote faster recovery.
- Comprehensive care: Our practice offers a full range of services, from diagnostic imaging and physical therapy to surgery. We ensure that patients receive complete, seamless care for their spinal conditions.
- Dedicated facilities: Southwest Scoliosis and Spine Institute is dedicated to providing patients with a safe and comfortable environment.
Finally, our board-certified physicians and fellowship-trained orthopedic surgeons use the full range of treatments to treat spine patients. Southwest Scoliosis and Spine Institute doctors and surgeons are experts with offices in Dallas, Plano, and Frisco, TX. They offer cutting-edge technology, comprehensive care, and dedicated facilities to ensure the best possible care for their patients. Call today at 214-556-0555 to make an appointment.
____________________
Clinical References & Corroboration Citations
To ensure medical accuracy, the facts on this page are corroborated by the following authoritative sources:
- Clinical Review: Degenerative Disk Disease. StatPearls [Internet]. National Library of Medicine / NIH.
- Practice Standards: Diagnosis and Treatment of Lumbar Disc Herniation. North American Spine Society (NASS).
- Patient Resources: Spondylosis (Arthritis of the Spine). American Academy of Orthopaedic Surgeons (AAOS).
- Epidemiology: Global prevalence of degenerative spinal conditions. PubMed / National Institutes of Health.
- WebMD: Degenerative Disc Disease
- Healthline: Degenerative Disc Disease
Additional Material on Degenerative Disc Disease
For further information on Degenerative Disc Disease, please review the below pages on this website
Degenerative Disc Disease – Diagnosis and Treatment Options
Is Degenerative Disc Disease Considered a Disability?
Degenerative Disc Disease Treatment
Degenerative Disc Disease Solution
The medical content on this page has been carefully reviewed. It was approved for accuracy by the Southwest Scoliosis and Spine Institute’s qualified healthcare professionals. This includes our board-certified physicians and Physician Assistants. Our team ensures that all information reflects the latest evidence-based practices and meets rigorous standards of medical accuracy, with oversight from our expert spine doctors to guarantee reliability for our patients.
If you or a loved one suffers from spinal pain, you owe it to yourself to call
Southwest Scoliosis and Spine Institute at 214-556-0555 to make an appointment.


