The Doctors at the Southwest Scoliosis and Spine Institute believe that spinal injections and medications will limit and remove Pain.
Therapeutic Use Of Spinal Injections & Medications
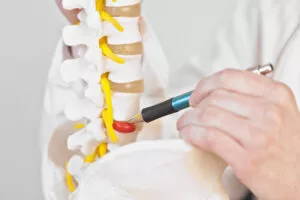 In many cases of chronic back pain, doctors use spinal injections to discover the genesis of the pain and to treat it. Doctors refer to these two separate uses of spinal injections as diagnostic and therapeutic. If an injection provides pain relief in the injected area, it means that this area appears as the source of the problem. Injections provide a therapeutic effect by providing temporary relief from pain. Your doctor at the Southwest Scoliosis and Spine Institute will always consider conservative management of back pain first. He or she might order a spinal injection to help with identifying the pain source as well as reducing the pain.
In many cases of chronic back pain, doctors use spinal injections to discover the genesis of the pain and to treat it. Doctors refer to these two separate uses of spinal injections as diagnostic and therapeutic. If an injection provides pain relief in the injected area, it means that this area appears as the source of the problem. Injections provide a therapeutic effect by providing temporary relief from pain. Your doctor at the Southwest Scoliosis and Spine Institute will always consider conservative management of back pain first. He or she might order a spinal injection to help with identifying the pain source as well as reducing the pain.
This webpage discusses spinal injections, including:
- Injected medications
- The types of injections
- Why you might choose to get an injection
- Why you might choose not to get an injection
Spinal Medications
With most spinal injections, the doctor injects a local anesthetic (numbing medication) called lidocaine (also known as Xylocaine) into a specific area of the spine. Lidocaine is a fast-acting drug, but the effects wear off within about two hours. That is why lidocaine is more useful as a diagnostic tool rather than a long-lasting pain reliever. Bupivacaine (also known as Marcaine) is another type of anesthetic that a doctor can use. It is slower to take effect, but it lasts longer, giving the patient more relief from pain.
Cortisone is a strong anti-inflammatory steroid medication. It is commonly injected along with a local anesthetic to reduce inflammation in the affected areas. Cortisone is long-lasting and released slowly to give the best possible benefits of pain relief. Cortisone may not begin working for several days following the injection, but the effects can last for months. Sometimes, doctors mix a narcotic medication such as morphine or fentanyl with cortisone and an anesthetic to get more pain relief.
Questions and Answers
What are Spinal Injections and how do they work?
Spinal injections refer to a medical procedure in which medications get injected directly into the spine to alleviate pain, reduce inflammation, and improve mobility. These injections can target different areas of the spine, such as the epidural space, facet joints, or nerve roots. The injected medications, which often include a combination of local anesthetics and anti-inflammatory steroids, help block pain signals and reduce inflammation, providing relief to patients with various spinal conditions.
Are Spinal Injections safe and what are their potential risks?
Spinal injections provide a safe and effective method to stop pain when performed by qualified healthcare professionals. However, as with any medical procedure, potential risks exist. Common risks include infection, bleeding, nerve damage, allergic reactions, and temporary increases in pain. It’s important to discuss your medical history and any existing conditions with your healthcare provider before undergoing spinal injections to ensure your safety and minimize risks.
How long do the effects of Spinal Injections last and how often do doctors administer the drugs
The duration of pain relief from spinal injections varies depending on the individual, the type of injection, and the underlying condition. Some patients experience significant relief that lasts for several months, while others may require more frequent injections. The number of injections administered over time may be limited due to potential side effects and the desire to avoid the overuse of steroids. Your healthcare provider will work with you to determine the appropriate treatment plan based on your specific needs.
We’re here to help STOP THE PAIN
Call (214) 556-0555 or Email Us to make an appointment with our expert spine doctors.
Types of Steroids Used in Epidural Injections
While cortisone is frequently used, several other steroids may be utilized in epidural steroid injections. The most commonly used steroids include:
- Dexamethasone
- Betamethasone
- Methylprednisolone
- Triamcinolone
The choice of steroids and dosage is tailored based on various factors such as patient-specific conditions, response to prior injections, the region of the spine being treated, and the epidural approach. These steroids are selected for their potent anti-inflammatory properties, which help in reducing pain and swelling around spinal nerves. The administration method ensures that the medication is delivered precisely to the inflamed area, providing targeted relief. By understanding the variety of steroids available and how they are chosen, patients can have more informed discussions with their healthcare providers about the best treatment options for their specific conditions.
What Are Epidural Steroid Injections Used For?
Epidural steroid injections are commonly used to treat back pain caused by several specific conditions:
- Herniated disc (slipped disc)
- Lumbar or cervical radiculopathy
- Spinal stenosis
- Sciatica
Corticosteroids are strong anti-inflammatory medications. When placed into the epidural space, they can significantly reduce inflammation around an irritated nerve that is causing back and leg pain and discomfort. This targeted approach helps alleviate pain and improve mobility, allowing patients to engage in physical therapy and other activities essential for recovery.
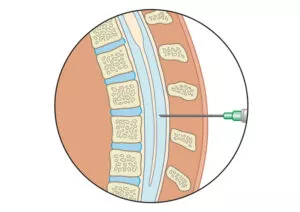 Spinal Injections
Spinal Injections
- Facet Joint Injections
- Hardware Injections
- SI Joint Injections
- Differential Lower Extremity Injections
- Epidural Steroid Injection (ESI)
With most spinal injections, the doctor injects a local anesthetic (numbing medication) called lidocaine (also known as Xylocaine) into a specific area of the spine. Lidocaine is a fast-acting drug, but the effects wear off within about two hours. That is why lidocaine is more useful as a diagnostic tool rather than a long-lasting pain reliever. Bupivacaine (also known as Marcaine) is another type of anesthetic that a doctor can use. It is slower to take effect, but it lasts longer, giving the patient more relief from pain.
When it comes to epidural steroid injections, a local anesthetic is injected into the skin to numb the area where the epidural needle is then placed. This helps to ensure that patients experience minimal discomfort during the procedure. While some mild discomfort may be felt, severe pain is generally not expected.
This combined approach of using local anesthetics such as lidocaine or bupivacaine ensures that patients remain as comfortable as possible throughout the injection process, providing both immediate and extended relief. The choice of anesthetic and its application is tailored to optimize patient comfort and diagnostic accuracy. There are three different ways to perform an epidural injection:
- caudal block
- Translumbar
- Transforaminal
Caudal Block
The surgeon places a caudal block through the sacral gap (a space below the lumbar spine near the sacrum). And then he places the injection into the epidural space. This type of block usually affects the spinal nerves at the end of the spinal canal near the sacrum. This collection of nerves refers to the cauda equina. One of the benefits of this type of injection normally does not puncture the dura.
Translumbar
The translumbar approach is the most common way of performing an epidural injection. The surgeon performs this type of injection by placing a needle between two vertebrae from the back. And, he inserts the needle between the spinous processes of two vertebrae. You can feel the bumps that make up the spinous process by feeling along the back of your spine.
Transforaminal
The transforaminal approach is a very selective injection around a specific nerve root. The foramina are small openings between your vertebrae through which the nerve roots exit the spinal canal and enter the body. By injecting medication around a specific nerve root, the doctor can determine if this nerve root is causing the problem. This type of epidural injection is useful for diagnostic purposes and is commonly injected into the neck.
Are Spinal Injections Safe And What Are Their Potential Risks?
Spinal injections provide a safe and effective method to stop pain when performed by qualified healthcare professionals. However, as with any medical procedure, potential risks exist. Common risks include infection, bleeding, nerve damage, allergic reactions, and temporary increases in pain. It’s important to discuss your medical history and any existing conditions with your healthcare provider before undergoing spinal injections to ensure your safety and minimize risks.
Specific to epidural steroid injections, the risks in any procedure involving a needle include bleeding, infection, and nerve damage. When performed properly, the risk of any of these is exceedingly low and usually outweighed by the potential benefit of the procedure.
Some Contraindications For Performing Epidural Steroid Injections Include:
- Bleeding disorders or anticoagulation
- Medication allergies (rare)
- Systemic infection or localized infection overlying the area
Additionally, the risks and benefits of repeated epidural steroid injections should be weighed on a case-by-case basis for patients who have or are at risk for osteoporosis, as some evidence suggests repeated steroid injections can accelerate bone loss. By understanding both the general and specific risks associated with spinal injections, patients can make informed decisions in consultation with their healthcare providers.
How Do Epidural Corticosteroid Injections Work?
Epidural steroid injections work by delivering a potent anti-inflammatory to the site of nerve impingement in the spine. Injected medications may include steroids, local anesthetics, and saline, and they can vary in volume and concentration on an individual basis. This customization ensures that the treatment is tailored to the specific needs of each patient.
To ensure correct, effective, and safe deposition of the injected medications, epidural steroid injections for pain management are routinely performed with fluoroscopic or X-ray guidance. This imaging technology helps doctors accurately target the site of nerve impingement, minimizing risks and enhancing the efficacy of the treatment. In select cases, CT or ultrasound guidance may be used as alternatives, depending on the specific circumstances of the patient.
Epidural injections for other applications may not require such precise image guidance, but for pain management, this step is crucial. By directly addressing the inflammation at the nerve root, these injections can provide significant relief and improve the quality of life for individuals suffering from spinal conditions.
Who Can Benefit From an Epidural Steroid Injection?
Patients with several common conditions, including:
- Lumbar disc herniation
- Degenerative disc disease
- Lumbar radiculopathy
- Sciatica
- Lumbar spinal stenosis
- Postherpetic neuralgia
- Facet/synovial cysts
These patients may benefit from an epidural steroid injection. This treatment can be an effective nonsurgical option or may aid in surgical planning, offering much-needed relief and improving patient outcomes. By understanding both the mechanism of action and the specific conditions that can benefit from an ESI, patients can make more informed decisions about their treatment options. This dual approach ensures that they receive the most comprehensive care tailored to their specific needs.
Facet Joint Injections
Facet joint injections are useful to localize and treat low back pain. These problems arise due to facet joints. These joints are located on each side of the vertebrae. They join the vertebrae together and allow the spine to move with flexibility. The facet joint injections form a pain block that allows the doctor to confirm that a facet joint is causing the pain. The medication used also decreases the inflammation that occurs in the joint from arthritis and joint degeneration.
It is important to make sure that the injection goes directly into the facet joint. Fluoroscopy is useful to confirm that the needle is in the right position before the surgeon injects any medication. A fluoroscope uses X-rays to show a TV image. Your doctor can watch on the screen as he places the needle into the joint and magnifies the image to increase accuracy.
There are two types of facet joint injections.
Intra-articular injections are injected directly into the joint to block the pain and reduce inflammation. Nerve blocks help determine whether the joint is indeed a source of pain by blocking the small nerves that connect with the joint.
Specific Indications for Spinal Injections and Medications
A facet joint injection is perhaps the best way to diagnose facet joint syndrome. Joints that look abnormal on an X-ray may not produce pain, while joints that look fine may cause pain. This rather simple procedure causes little risk.
Hardware Injections
Your doctor may need to determine whether the metal hardware used during the surgery causes your discomfort. Doctors perform a hardware injection by injecting lidocaine alongside the spinal hardware that was placed in the spine during surgery. If the pain is removed temporarily by the injection, it may indicate that the hardware is causing your pain.
Specific Indications: These injections are used to determine whether a specific piece of hardware is causing the pain and may need removal.
SI Joint Injections
Sacroiliac (SI) joint pain is easily confused with back pain from the spine. The SI joint is located between the sacrum and pelvic bones. Sometimes, injecting the SI joint with lidocaine may help your doctor determine whether the SI joint is the source of your pain. If doctors inject the joint and your pain does not go away, it is probably coming from somewhere else.
And, if the pain goes away immediately, your doctor may also inject cortisone into the joint before removing the needle. Also, cortisone is added to treat inflammation from SI joint arthritis. The injection usually gives temporary relief for several weeks or months. Specific Indications: SI joint injections are useful in both cases, for pain treatment and determining the source of the pain. Usually, this injection requires the use of fluoroscopic guidance or a CT scan. This helps to ensure that the surgeon places the needle correctly into the joint.
Differential Lower Extremity Injections
Various types of injections into certain areas of the lower extremities can help your doctor decide where the pain is starting. Pain that comes from problems with the back and spinal nerves can mimic many other conditions. Sometimes it is impossible to tell if the pain you are experiencing is due to a back condition or a problem in your hip, knee, or foot.
To help determine whether a joint of your lower limb is causing you pain, your doctor may suggest injecting medication, such as lidocaine, into the joint to numb the area. Once the doctor injects medication and the pain goes away immediately, you must know that the specific joint is more likely the source of the pain than your back. Your doctor can then focus on finding the problem in the joint.
What Are The Side Effects Of Epidural Steroid Injections?
Spinal injections provide a safe and effective method to stop pain when performed by qualified healthcare professionals. However, as with any medical procedure, potential risks exist. Common risks include infection, bleeding, nerve damage, allergic reactions, and temporary increases in pain. It’s important to discuss your medical history and any existing conditions with your healthcare provider before undergoing spinal injections to ensure your safety and minimize risks.
Common side effects include mild injection site pain, temporary worsening of usual pain, flushing, insomnia, or increased blood sugar. These are usually self-limited and resolve within one to three days. A less common side effect is headache. By understanding both the general risks and specific side effects, you can make a more informed decision about your treatment options. Always consult with your healthcare provider to discuss any concerns and to tailor the procedure to your individual health needs.
General Contraindication for Spinal Injections and Medications
When certain medical conditions are present, doctors may determine it is unsafe to perform a spinal injection. Your doctor will discuss any concerns with you before making a final decision.
Bleeding Tendencies
If you tend to have heavy bleeding or are on anticoagulant therapy (medication that prevents blood clotting), you are not a good candidate for spinal injections. The physician might ask you to stop all medications such as aspirin and ibuprofen five days before the injection. These medications can decrease the ability of the blood to clot and lead to problems. Make sure your provider has a list of your medications well ahead of your scheduled procedure.
Infections
If you have a local or systemic infection, a spinal injection may put you at greater risk of spreading the infection into the spine, causing meningitis (inflammation in the covering that surrounds the spinal cord). Make sure to tell your healthcare provider if you have any infected wounds, boils, or rashes anywhere on your body.
Unstable Medical Conditions
Injections are usually an elective procedure. Doctors offer injections to patients without life-threatening conditions. It is necessary to treat the medical condition of a medically unstable patient before giving any elective injections.
General Precautions for Spinal Injections and Medications
Finally, consider these basic warnings before choosing to have a spinal injection. If you are chronically taking a platelet-inhibiting drug, such as aspirin or NSAIDs (non-steroidal anti-inflammatory drugs), you have an increased risk of bleeding, and the doctor might suspend such drugs for a couple of days so that you can get a spinal injection to relieve the pain. If you are hypersensitive or have certain allergies to medications, you may have a negative reaction to the drugs used in the injection. Make sure to give your provider a list of your allergies.
If you have an accompanying medical illness, you should discuss the risks of spinal injections with your physician. For instance, patients with diabetes mellitus might experience an increase in blood sugar after an injection of cortisone. Patients with congestive heart failure, renal failure, hypertension, or a significant cardiac disease may have problems due to the effects of fluid retention several days after injection.
How Long Do Epidural Injections Last For Back Pain?
The duration of pain relief from spinal injections varies depending on the individual, the type of injection, and the underlying condition. Some patients experience significant relief that lasts for several months, while others may require more frequent injections. The number of injections administered over time may be limited due to potential side effects and the desire to avoid the overuse of steroids. Your healthcare provider will work with you to determine the appropriate treatment plan based on your specific needs. Epidural steroid injections are typically recommended up to three to six times per year. For cases involving a new disc herniation, injections may be scheduled only weeks apart, aiming for a quick and complete resolution of symptoms. In contrast, for chronic conditions, it is common to get injections spaced three to six months or more apart.
By considering both the general guidelines and your health scenario, your healthcare provider can help ensure that you receive the most effective and safe treatment plan tailored to your needs. For more specific time frames, epidural steroid injections can help resolve pain permanently in patients with a new disc herniation who respond favorably. For those dealing with chronic pain or recurrent disc herniations, the desired duration of effect typically ranges from three to six months or more.
Understanding these time frames can help you set realistic expectations and work collaboratively with your healthcare team to manage your back pain effectively.
By tailoring the treatment plan to your unique condition, the goal is to maximize the benefits while minimizing potential risks.
Find Top Scoliosis and Spine Experts – Orthopedist
The Southwest Scoliosis and Spine Institute is known as the Dallas Metroplex and the North Texas premier Scoliosis practice. Also, our doctors, who have offices in Dallas, Plano, and Frisco, Texas, specialize in diagnosing and treating Scoliosis, Complex Spine Issues, and Spine Revision corrections.
Our board-certified, fellowship-trained surgeons have diagnosed and treated more than 100,000 patients. In addition, we have successfully performed more than 16,000 surgeries for scoliosis, including complicated spine cases and revision surgeries. If you live with the pain of scoliosis or a spine condition, the Southwest Scoliosis and Spine Institute will provide the expertise and surgical competence to provide solutions based on years of study. Please contact us. There is no reason to live in pain, and our doctors want to help.
_____________________
Citation: National Library of Medicine – Spinal Injections
The medical content on this page has been carefully reviewed and approved for accuracy by the Southwest Scoliosis and Spine Institute’s qualified healthcare professionals, including our board-certified physicians and Physician Assistants. Our team ensures that all information reflects the latest evidence-based practices and meets rigorous standards of medical accuracy, with oversight from our expert spine doctors to guarantee reliability for our patients.
If you or a loved one suffers from spinal pain, you owe it to yourself to call Southwest Scoliosis and Spine Institute at 214-556-0555 to make an appointment.


