ANKYLOSING SPONDYLITIS
Ankylosing Spondylitis (AS), a chronic inflammatory type of progressive arthritis, leads to chronic inflammation of the spine and sacroiliac (SI) joints. AS can lead to pain and serious impairment of strength and ability to function.
At the Southwest Scoliosis and Spine Institute, our expert Ankylosing Spondylitis Doctors and Surgeons are dedicated to diagnosing and treating spinal problems in children and adults to ensure comprehensive care is tailored to each patient’s needs. With advanced techniques and a compassionate approach, our team diagnoses, treats, and cares for patients suffering from Ankylosing Spondylitis.
The Scoliosis and Spine Institute doctors are experts in treating Ankylosing Spondylitis
ANKYLOSING SPONDYLITIS (AS)
Southwest Scoliosis and Spine Institute’s board-certified, fellowship-trained orthopedic physicians Richard Hostin, MD, Devesh Ramnath, MD, Ishaq Syed, MD, Shyam Kishan, MD, and Kathryn Wiesman, MD have years of experience treating thousands of patients with complex spine conditions. As an example, Ankylosing Spondylitis can become a very debilitating disease. In addition, patients who suffer from the pain associated with this condition, begin complaining of low back pain and pain in the buttocks. (Sieper et al., 2015)
Ankylosing Spondylitis (AS) primarily affects the axial skeleton (bones of the head and trunk), including the ligaments and joints. Furthermore, inflammation due to AS can also affect other joints and organs in the body, such as the eyes, lungs, kidneys, shoulders, knees, hips, heart, and ankles. Unfortunately, AS causes changes throughout the body.
One way to understand what Ankylosing Spondylitis does to the body is to look at the words “ankylosing” and “spondylitis.” So, Ankylosing means stiffening and the word comes from the Greek word “angkylos,” which means bent. Also, Spondylitis means inflammation of the spine and this word comes from the Greek word “spondylos,” which means spinal vertebrae. In essence, AS causes your spine to stiffen due to inflammation of the joints and may cause the vertebrae to fuse together. Moreover, it may also cause a kyphosis of the spine, which gives your spine a forward curve.
Questions and Answers
What is Ankylosing Spondylitis?
Ankylosing spondylitis appears as a chronic inflammatory disease that primarily affects the spine, causing pain, stiffness, and progressive fusion of the vertebrae. It belongs to a group of conditions known as spondyloarthropathies and can also affect other joints and organs. A person with AS suffers from inflammation of the spinal joints, leading to the formation of new bone and fusion, resulting in reduced mobility and deformity. (van der Heijde et al., 2017)
What are the common symptoms of Ankylosing Spondylitis?
The most common symptoms of Ankylosing Spondylitis include persistent low back pain and stiffness, which becomes worse in the morning or after periods of rest. The pain and stiffness typically improve with physical activity or exercise. Other symptoms may include pain and stiffness in the hips, shoulders, or other joints, fatigue, loss of appetite, weight loss, and eye inflammation (uveitis). The symptoms can vary in severity and may come and go over time.
What are the treatment options for Ankylosing Spondylitis?
- The treatment of Ankylosing Spondylitis aims to alleviate symptoms, improve function, and slow down the progression of the disease. The main treatment approaches include:
- Medications: Nonsteroidal anti-inflammatory drugs (NSAIDs) are often prescribed to reduce pain and inflammation. In more severe cases, disease-modifying antirheumatic drugs (DMARDs), such as sulfasalazine or biologic agents, may be recommended to target the underlying inflammatory process.
- Exercise and Physical Therapy: Regular exercise and physical therapy are crucial to maintain flexibility, improve posture, and strengthen the muscles supporting the spine. Activities like swimming, walking, and specific stretching exercises can be beneficial.
- Posture and Lifestyle Modifications: Maintaining good posture, using ergonomic aids, and practicing proper body mechanics can help manage symptoms and reduce strain on the spine. Quitting smoking and maintaining a healthy weight are also important lifestyle factors.
- Education and Support: Learning about the condition, attending support groups, and seeking emotional support can be helpful in managing the challenges associated with Ankylosing Spondylitis.
A Healthy Spine
A healthy spine moves in multiple directions, allowing the body to bend, turn, and twist. The spinal bones are joined together by flexible ligaments and are separated by cushiony discs, which allow a lot of movement. Movement can become impossible if the ligaments calcify and the bones fuse together, and this can disable a person in its advanced stages.
Learn about Ankylosing Spondylitis, including:
- What causes the condition
- What are the symptoms associated with Ankylosing Spondylitis
- How to diagnose AS
- What treatment options are available
Anatomy
In order to understand your symptoms and treatment options, it helps to begin with a basic understanding of spinal anatomy. Therefore, this includes becoming familiar with the various parts that make up the spine and how these parts work together.
Learn more about the anatomy of the spine.
Often, the first sign of Ankylosing Spondylitis (AS) occurs with the inflammation of the sacroiliac (SI) joints. Specifically, the SI joints are the two joints that connect the lower spine to the pelvis. Also, you can feel these joints about two inches to either side of the spine in the lower back.
With this disease, inflammation eventually moves to the spine. As a result, long-term inflammation of the spinal joints (called spondylitis) leads to calcium deposits forming in the ligaments around the intervertebral discs (the cushions between your spinal vertebrae) and the ligaments that hold the vertebrae together. When these ligaments calcify, movement becomes restricted. Eventually, the vertebrae may fuse together.
Ankylosing Spondylitis Causes
At this time, the origin of AS remains unknown. However, we know a lot about how Ankylosing Spondylitis progresses and why it causes spinal stiffening, which may affect the movement of other parts of the body. When AS first appears, an inflammation of the bones (called osteitis) occurs around the edges of the joints. In these areas, the number of special cells (called inflammatory cells) begins to increase. Because inflammatory cells produce chemicals that damage the bone, bones begin to dissolve and weaken around the edge of each joint.
Once damage to the bone starts, the body continually tries to repair the damage with scar tissue and new bone tissue. As the process continues, the bone becomes weaker and weaker. When the inflammation finally “burns out” and begins to disappear, the body attempts to heal the bone by producing calcium deposits around the area of the damage. For some unclear reason, as the bone heals itself, the calcium deposits spread to the ligaments and discs between the vertebrae. Meanwhile, this leads to a fusion of the spine, sometimes referred to as bony ankylosis.
Those Affected
AS primarily affects younger adult males in adolescence or early adulthood. Furthermore, AS occurs three times more in males than in females. Although AS can strike people of any age, race, or sex, the onset occurs more often in Caucasian men between the ages of 17 and 35. In women, the symptoms of AS often begin to appear during pregnancy.
Also, evidence appears to suggest that AS passes genetically from parents to children. Research reveals a specific gene — the HLA-B27 gene — is present in 80 to 90 percent of people who have the disease. Fortunately, this does not mean that if you have the gene, you will automatically get AS. About eight percent of Americans have this gene, but only about one percent of those will develop the disease.
Ankylosing Spondylitis Pain and Symptoms
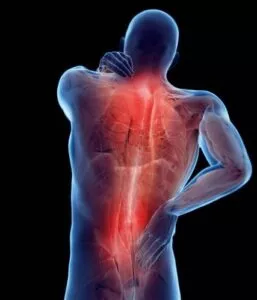 Like other forms or types of arthritis, the symptoms of AS are from the effects of inflammation. Initially, the symptoms may come and go for weeks or months at a time.
Like other forms or types of arthritis, the symptoms of AS are from the effects of inflammation. Initially, the symptoms may come and go for weeks or months at a time.
- The first sign of AS occurs with a patient diagnosed with sacroiliitis or inflammation of the sacroiliac joints. This condition causes pain in the lower back and buttocks.
- People with Ankylosing Spondylitis usually complain of severe lower back pain, along with buttock, hip, and thigh pain on one or both sides. It usually comes on gradually and gets worse with time.
- Stiffness and lower back pain commonly occur in the morning and ease with activity over the course of the day.
- Prolonged rest worsens the symptoms of AS, which differs from some other forms of low back pain that are eased with rest.
- AS reduces spinal flexibility, which can cause the body to bend forward and backward.
- In the mid-back, AS can affect the joints where the ribs connect to the vertebrae. These are called the costotransverse and costovertebral joints. Inflammation in these joints can cause pain in the chest wall and abdomen.
- Symptoms in the neck include stiffness, pain, and limited neck motion.
- Because AS attacks the joints of the body, synovitis can occur. Synovitis is a term used to describe inflammation of the synovial membrane (lining of the joints). Symptoms of synovitis include pain, stiffness, and swelling in any joint in the body.
Other Organ Symptoms
- AS will affect breathing as the condition progresses. The disease can make the mid-back curve forward, a deformity called kyphosis. When this occurs, it can compress the lungs and make it increasingly difficult to take a breath. Also, when the disease affects the joints between the ribs and spine, the chest loses its ability to expand enough to take a full breath. Inflammation of the lungs can also occur with AS, making it even harder to breathe (van der Heijde et al., 2017).
- AS can affect the eyes by causing eye inflammation. About 25 percent of AS patients develop iritis, a condition caused by inflammation of the iris. The eye may become red with some pain, but usually, vision loss does not occur.
- Eventually, the spine bones may grow together, fusing into one continuous column of bone. This occurs with the calcification of the ligaments and discs between each vertebra. If the vertebrae fuse together, the spine’s mobility decreases, leaving the vertebrae brittle and vulnerable to fractures. When the spine becomes completely fused together, the pain in the spinal area usually goes away. This does not signal a remission of the disease. However, patients are left with no spinal mobility and brittle bones that are more likely to fracture. If pain suddenly reappears in the back after a long period of no pain, the doctor should look for a possible fractured vertebra.
Ankylosing Spondylitis Diagnosis
In the early stages of AS, the disease makes it difficult to make a definite diagnosis. Therefore, Ankylosing Spondylitis doctors will request a history of your health and perform a physical exam. Other diagnostic tests include X-rays and lab tests. Then, doctors will consider the following to make a diagnosis of AS:
- The onset of back pain before age 35-40
- gradual onset not caused by a trauma
- pain that has lasted more than three to six months
- improvement with exercise and motion
- spinal stiffness in the mornings
- family history of AS
X-rays
As previously mentioned, doctors may order X-rays of the spine and pelvis if indications of AS occur. If examination of the X-rays reveals that the vertebral bodies are deformed and have a square shape, then AS is present. Doctors refer to this as a “bamboo spine,” as the spine appears very symmetrical and segmented.
For early-onset AS, X-ray findings will confirm the disease on both sides of the SI joint. Specifically, these signs will include patchy osteoporosis (loss of bone mass), poorly defined joint margins, a widening of the SI joint space, and erosion of the joint. In advanced cases of AS, the X-rays will show many changes, including calcium deposits in the ligaments and discs, complete spinal fusion, and sometimes old spinal fractures.
Lab Tests
If your doctor suspects that you have AS, a blood test can determine if the HLA-B27 gene is present. As of this date, a specific blood test does not exist to determine if a person has AS. You may see AS referred to as a seronegative spondyloarthropathy. This refers to a patient who has all the symptoms of AS but does not have the positive blood test for the gene that usually indicates AS. (The negative test is called the rheumatoid factor.) In addition, this is simply a way for doctors to classify AS from other forms of systemic arthritis. If you have the symptoms of AS and the HLA-B27 gene, AS is likely the correct diagnosis.
Additionally, the Erythrocyte Sedimentation Rate (ESR) blood test will show inflammation in the blood from any cause. Furthermore, the Ankylosing Spondylitis doctor may request a urinalysis to look for possible kidney abnormalities, which are another symptom of AS.
Ankylosing Spondylitis Treatment Options
Presently, a cure for AS does not exist, but effective treatments can help relieve pain and improve the condition. Ankylosing Spondylitis doctors should start with a conservative treatment plan, usually involving medication, physical therapy, and exercise. At some point, surgery may be necessary to treat problems caused by AS in the spine and other joints of the body.
Medication
As mentioned, doctors will suggest medications to reduce inflammation and pain. If they prove effective, NSAIDs are the preferred medication. It is best to take these medications as prescribed by your doctor. Possible side effects of NSAIDs include nausea, stomach upset, diarrhea, and abdominal pain. To avoid side effects, patients should take these drugs after eating.
If NSAIDs are not sufficient, your doctor may recommend a medication called sulfasalazine. Corticosteroids, such as prednisone, are also very effective at reducing inflammation, but their side effects can be serious if taken on a long-term basis.
If anti-inflammatory medications do not control the pain and inflammation sufficiently, there are medications available that block the immune system in order to reduce inflammation. These medications have many side effects, so patients who take them must be closely monitored.
Learn more about medications used to treat back problems
Physical Therapy
Your Ankylosing Spondylitis doctor may have you work with a physical therapist. In calming pain and inflammation, a well-rounded rehabilitation program assists by improving mobility and strength, and may play a role in helping with daily activities with greater ease and ability.
Conducting safe movements can improve spine mobility and posture, in view of the fact that physical therapy assists in pain control and the prevention of deformities from AS. Patients are advised against prolonged sitting and bed rest and encouraged to keep their spines straight, walk erect, and avoid stooping over for long periods. Therefore, doctors may schedule therapy sessions two to three times each week for up to six weeks.
The goals of physical therapy are to help you.
- Learn correct posture and body movements to counteract rounding of the upper back (kyphosis)
- Use appropriate sleep positions on a firm mattress and a thin pillow
- Maintain appropriate activity levels
- Implement daily stretching and strengthening exercises
- Learn ways to manage your condition
Learn more about spinal rehabilitation
Surgical Treatment
While surgery is not a cure for AS, it may be considered in certain cases to manage severe symptoms, correct deformities, or address complications. Here are some surgical procedures and methods that can be used to address Ankylosing Spondylitis:
- Spinal Fusion: Spinal fusion is a surgical procedure that involves permanently connecting two or more vertebrae together. In AS, spinal fusion can help stabilize the spine and reduce pain caused by excessive movement and instability. The procedure aims to promote spinal alignment and prevent further deformity.
- Osteotomy: An osteotomy is a surgical procedure that involves cutting and reshaping the bones to improve alignment. In AS, osteotomy may be performed to correct spinal deformities, such as kyphosis (excessive forward curvature of the spine) or scoliosis (sideways curvature of the spine). By correcting these deformities, osteotomy can help improve posture and reduce pain.
- Total Hip Replacement: AS can affect the hip joints, leading to pain, stiffness, and loss of mobility. In cases where conservative treatments fail to provide relief, total hip replacement surgery may be considered. This procedure involves replacing the damaged hip joint with an artificial joint (prosthesis) to improve function and reduce pain.
- Total Knee Replacement: Similarly, AS can also affect the knee joints, causing pain, swelling, and difficulty in walking. If conservative measures are ineffective, total knee replacement surgery may be recommended. This procedure involves removing the damaged knee joint surfaces and replacing them with artificial components, providing pain relief and improving knee function.
- Chest Expansion Surgery: In advanced cases of AS, the rigidity of the chest wall can restrict lung function, leading to breathing difficulties. Chest expansion surgery aims to improve lung capacity by releasing the fused ribs and correcting thoracic deformities. This procedure can help alleviate respiratory symptoms.
In conclusion
In conclusion, it is important to note that surgery is typically considered when conservative treatments, such as medication, physical therapy, and lifestyle modifications, have not provided sufficient relief. Surgery for Ankylosing Spondylitis (AS) is usually reserved for specific severe cases and is highly individualized.
When Surgery is Considered
Severe Spinal Deformity:
- Extreme Kyphosis: If AS has led to extreme kyphosis, which prevents standing and looking forward, a spinal osteotomy might be considered. This procedure involves cutting through the spinal bones and realigning them to allow the patient to stand upright. Importantly, the spinal cord is not cut; only the vertebrae are.
Hip Joint Damage:
- Artificial Hip Replacement: Surgery may also be necessary if the hip joints are severely damaged by the arthritis associated with AS. In such cases, an artificial hip replacement might be required, a fairly common procedure for patients with AS.
The decision to undergo surgery for Ankylosing Spondylitis should be made in consultation with a healthcare professional specializing in the management of AS. This ensures that the chosen treatment is tailored to the individual’s specific condition and needs.
Why Choose the Scoliosis and Spine Institute
Our Medical Practice at Southwest Scoliosis and Spine Institute, with offices in Dallas, Plano, and Frisco, Texas, has top-rated Ankylosing Spondylitis doctors with the experience and knowledge necessary to offer patients the best possible treatment. Additionally, we welcome new patients and invite you to make an appointment.
____________________
Citation: National Institute of Health – Ankylosing Spondylitis
The medical content on this page has been carefully reviewed and approved for accuracy by the Southwest Scoliosis and Spine Institute’s qualified healthcare professionals, including our board-certified physicians and Physician Assistants. Our team ensures that all information reflects the latest evidence-based practices and meets rigorous standards of medical accuracy, with oversight from our expert spine doctors to guarantee reliability for our patients.
If you or a loved one suffers from spinal pain, you owe it to yourself to call Southwest Scoliosis and Spine Institute at 214-556-0555 to make an appointment.


