CERVICAL KYPHOSIS
Cervical Kyphosis refers to an exaggerated curve in the neck. It can occur in children and adults. Cervical kyphosis usually occurs from a congenital condition or from trauma or aging — affecting both children and adults. Unfortunately, the symptoms range from mild pain to debilitating systemic deformity and pain.
At the Southwest Scoliosis and Spine Institute, our expert Cervical Kyphosis Doctors are dedicated to diagnosing and treating spinal conditions in children and adults, and ensuring comprehensive care tailored to each patient’s needs. With advanced techniques and a compassionate approach, our team is here to diagnose, treat and care for patients suffering from Cervical Kyphosis.
The Southwest Scoliosis and Spine Institute specializes in the spine. We treat all types of spine problems to include revision surgery that corrects another surgeon’s procedure.
Cervical Kyphosis
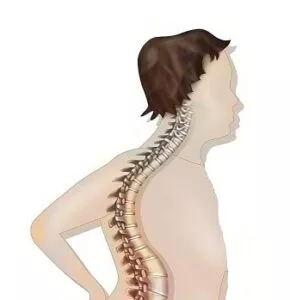 When viewed from the side, the normal cervical spine curves slightly inward and is referred to as lordosis. Kyphosis refers to a term used to describe a type of abnormal curve in the spine. Also, a kyphotic curve looks like the letter “C” with the opening of the C pointing toward the front. Consequently, this type of curve is the opposite of a normal lordotic curve, which has the opening facing the back. When we see larger abnormal curves, we see more serious problems.
When viewed from the side, the normal cervical spine curves slightly inward and is referred to as lordosis. Kyphosis refers to a term used to describe a type of abnormal curve in the spine. Also, a kyphotic curve looks like the letter “C” with the opening of the C pointing toward the front. Consequently, this type of curve is the opposite of a normal lordotic curve, which has the opening facing the back. When we see larger abnormal curves, we see more serious problems.
Cervical Kyphosis is also referred to as “Reverse Curve Neck”, also known as a “reversed cervical curve”. Reverse Curve Neck is often associated with poor posture, prolonged use of electronic devices, and traumatic injuries.
The cervical spine consists of seven vertebrae (C1 to C7), which provide support and mobility for the head and neck. Normally, the cervical spine has a slight lordotic curve, which helps distribute mechanical stress during movement. This natural curvature is essential for the spine’s function and flexibility.
Questions and Answers
What are the Symptoms of Cervical Kyphosis
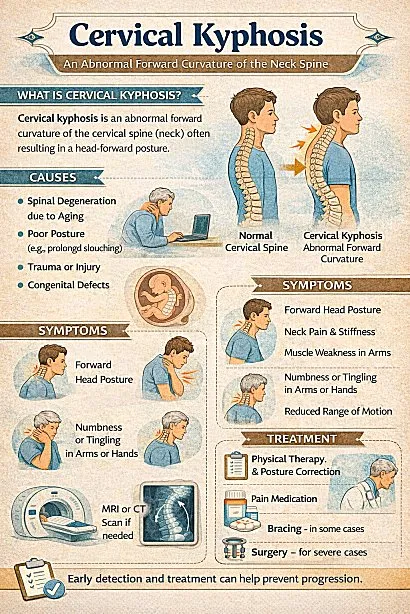
The symptoms of cervical kyphosis can vary depending on the severity of the condition. Common symptoms include neck pain, stiffness, loss of the natural neck curve (lordosis), restricted range of motion in the neck, headaches, muscle weakness or spasms, tingling or numbness in the arms or hands, and difficulty maintaining proper balance and posture. In severe cases, compression of the spinal cord or nerves may occur, leading to more pronounced neurological symptoms.
What Causes Cervical Kyphosis
Cervical kyphosis can have various causes. Some common factors include age-related degenerative changes, such as disc degeneration, osteoarthritis, or vertebral compression fractures. Traumatic injuries, such as fractures or dislocations of the cervical spine, can also lead to cervical kyphosis. Other causes may include congenital abnormalities, genetic conditions, tumors, infections, or certain medical conditions like ankylosing spondylitis or muscular dystrophy. Poor posture and prolonged neck flexion can contribute to the development of cervical kyphosis over time.
How is Cervical Kyphosis Treated
The treatment for cervical kyphosis depends on the severity of the condition, the underlying cause, and the presence of symptoms. Non-surgical treatment options may include physical therapy to improve neck strength and flexibility, postural training, pain management techniques (e.g., medication, heat/cold therapy), and wearing a cervical collar or brace to provide support. In cases where conservative measures are ineffective or if there is significant instability or neurological compromise, surgery may be considered. Surgical options may involve decompression (removing bone spurs or herniated discs) and fusion (joining vertebrae together) or more complex procedures like osteotomies (removing a wedge of bone to correct the curvature) or artificial disc replacement.
Tech Neck vs. Cervical Kyphosis
Tech neck and cervical kyphosis are often used interchangeably, but there’s a slight distinction between the two.
Cervical Kyphosis
- Medical term for an abnormal forward curve of the neck.
- Encompasses various causes beyond technology, such as arthritis, osteoporosis, or congenital conditions.
Tech Neck
- A more specific term referring to the forward head posture caused primarily by excessive use of electronic devices.
- A type of cervical kyphosis, but not all cervical kyphosis is tech neck.
In essence, tech neck is a specific type of cervical kyphosis. Both conditions share similar symptoms, including:
- Neck pain
- Headaches
- Shoulder pain
- Stiffness
- Numbness or tingling in arms or hands
Understanding the difference can help in determining the root cause of your discomfort and selecting appropriate treatment options.
Anatomy of the Spine
In order to understand symptoms and treatment choices, it helps to start with a basic understanding of the anatomy of the spine. This includes becoming familiar with the various parts that make up the neck and how they work together.
The normal Lordotic spine
As described earlier, the cervical spine normally has lordosis or inward curvature. However, kyphosis occurs when the normal inward curve reverses and causes an abnormal forward curve in the cervical spine. The normal range of the thoracic kyphosis, which is the curve in the middle section of the spine, is typically between 20 and 40 degrees. This curvature is a natural part of the spine’s structure, helping with overall balance and the ability to absorb shock. In contrast, the cervical spine, located in the neck, along with the lumbar spine at the lower back, both exhibit a lordotic curve. This curve resembles a backward ‘C’ and functions similarly in aiding the spine’s structural integrity and flexibility.
The stability of the cervical spine and its ability to stay in the lordotic position depend on other parts of the spine. Additionally, the vertebral bodies need strength to support the head and keep the normal shape of the spine. Furthermore, the facet joints, ligaments, and soft tissues in the back of the neck and back must remain strong. And the muscles in the back must resist the effect of gravity pulling the head forward. If damage to any of these three areas occurs, a kyphotic deformity can develop, and the weight of the head can cause a reversal of the normal curvature of the spine.
Causes of Cervical Kyphosis
This condition has several possible causes and can develop in both children and adults.
Iatrogenic Causes
Kyphosis can occur from the effects of surgery, specifically after laminectomy surgery. This procedure relieves pressure on the spinal cord or spinal nerves. During the procedure, surgeons remove the lamina bone that covers the spinal canal. Sometimes, part or all of the facet joints are also removed during the procedure. This can cause looseness between the problem vertebrae. When this happens, the spine may begin to tilt forward, which is medically referred to as an iatrogenic cause.
Kyphosis may also occur after cervical fusion surgery. In this case, the spine will begin to “bend” over the topmost part of the fusion. The forward tilt causes an imbalance that can lead to kyphosis. If the fusion fails to heal properly, similar problems can also arise. Even when a fusion heals normally, kyphosis can occur if the vertebrae heal with improper alignment.
Degenerative Disc Disease
Degeneration of the intervertebral disc can lead to kyphosis in the neck. In older adults, the wear and tear of aging can cause the discs to collapse. This may cause the head to tilt forward, making the neck bend forward too. This process may steadily get worse over many years and cause Adult Kyphosis. The weight of the head causes unbalanced forces to push the neck further and further forward. This slowly leads to a loss of the normal curve and may end with cervical kyphosis. Learn more about degenerative disc disease.
Congenital Kyphosis
Congenital kyphosis is a spinal condition that originates at birth due to developmental issues in the spine. This condition results from abnormalities in the spinal vertebrae’s formation, typically leading to a forward-curving spine. Such deformities occur when the vertebrae develop a wedge-like shape, compounding into a pronounced curve as they stack on top of each other.
Characteristics of Congenital Kyphosis
- Structural Deformities: The primary characteristic of congenital kyphosis is the malformed development of spinal vertebrae, which fail to form completely or form in a triangular shape.
- Associated Conditions: It’s common for individuals with this condition to have concurrent anomalies in other systems, such as the kidneys or the urinary tract, indicating a broader developmental issue.
Treatment Options for Congenital Kyphosis
Surgical Intervention:
The most effective treatment for managing congenital kyphosis is through surgical means.
- Early Surgery Benefits: Undertaking surgery at an early stage is crucial as it helps in achieving the best outcomes by preventing further progression of the spinal curve.
Monitoring and Follow-Up:
In cases where surgery is not immediately possible, meticulous and regular monitoring is imperative to manage the condition and avert severe complications.
Conservative Treatments:
Non-surgical approaches, including physical therapy and bracing, are generally less effective in correcting the spinal curvature in congenital kyphosis but may be utilized to alleviate symptoms.
In summary, congenital kyphosis is a complex condition with serious implications for physical development. Effective management usually requires surgical intervention, alongside continuous medical oversight to ensure optimal health outcomes.
Cervical kyphosis can occur by inheritance, which means that you are born with it. A person born with some sort of defect, such as the incomplete formation of part of the spine, may end up with an increasing kyphosis in the neck. Congenital kyphosis usually leads to a growth disturbance of the vertebrae. Instead of growing normally, the vertebrae grow into a triangular shape with the thin end pointing forward. Because the vertebrae are stacked on top of each other, the triangle shape causes the spine to have a forward curvature. When a child has congenital kyphosis, there are generally additional birth defects in other areas of the body, most commonly in the kidneys and urinary system.
Trauma
Cervical kyphosis can occur as a result of an injury to the neck. Vertebral compression fractures cause the vertebral body to collapse into the shape of a wedge. This causes the section of the spine to tip forward, and the resulting imbalance leads to a loss of the normal curvature of the neck. Other injuries that damage the ligaments along the back of the cervical spine can also cause kyphosis. If the kyphosis gets bad enough, it can narrow the spinal canal and put pressure on the spinal cord (spinal stenosis).
Other Causes
Other less common causes of cervical kyphosis include infections or tumors in the spine, systemic (whole-body) diseases that affect the spine, such as ankylosing spondylitis, and radiation therapy for cancer in the neck. Children, especially those who have had radiation therapy to the neck, may have altered growth in the cervical vertebrae, leading to future problems with kyphosis.
What Stretches and Exercises Can Help Prevent Cervical Kyphosis?
Simple Stretches
Performing regular stretches can go a long way in maintaining the natural curvature of your neck and preventing cervical kyphosis. Here are some effective ones:
- Shoulder Rolls: Gently roll your shoulders forward and backward in a circular motion to release tension in the upper back and neck.
- Neck Extensions: Slowly tilt your head back, looking up towards the ceiling, and hold for a few seconds. This helps to counteract forward head posture.
- Back Bends: Carefully lean backward from a standing position, placing your hands on your hips for support. This can help stretch the spine and improve posture.
Strengthening Exercises
Building strength in the upper body can support better posture and reduce the risk of cervical kyphosis. Consider incorporating the following exercises into your routine:
- Resisted Neck Flexion: Use a resistance band or your own hands to provide gentle resistance as you push your head forward. Repeat in all directions for balanced neck strength.
- Thoracic Extensions: Lie face down on a stability ball or a bench, extending your back upwards. This exercise strengthens the muscles that support the spine.
For More Intensive Work
For those who want to take it a step further, engaging in structured classes and advanced routines can offer greater benefits:
- Yoga: Participating in yoga classes can help improve your flexibility, strength, and posture. Poses like the “Downward Dog” or “Cobra” are particularly beneficial for spine health.
- Strength Training: Building overall upper body strength through weight lifting can support a healthy posture. Focus on exercises that target the back, shoulders, and neck.
By incorporating these stretches and exercises into your routine, you can significantly reduce the risk of developing cervical kyphosis.
Symptoms
The symptoms and severity of kyphosis vary. Symptoms range from minor changes in the shape of your spine to severe deformity, neurologic deficits, and chronic pain. Neck movement may become limited, making it difficult to turn the neck fully or to look up for very long. The abnormal forward curvature can eventually appear unattractive. Neck pain may appear, especially if the kyphosis stems from degenerative changes.
If the kyphosis becomes severe, pressure can occur on the spinal nerve roots or spinal cord. This can cause weakness in the arms or legs, loss of grip strength, or difficulty walking due to spasticity in the legs. Bowel or bladder control may become lost. In extremely severe cases that are left untreated, paralysis from the neck down may even result.
With a kyphotic deformity, the spinal cord can stretch when the spine bends forward. The spinal cord provides the body’s connection to the brain, and when damaged or compressed, the body loses some of its ability to function properly. If the pressure builds upon the spinal cord, it can cause cervical myelopathy. Myelopathy may impair normal walking, hand and finger use, and bowel and bladder function. Doctors take these symptoms very seriously because severe myelopathy may lead to permanent nerve damage. Pressure on the spinal cord can eventually lead to quadriplegia, paralysis of all four limbs.
We’re here to help STOP THE PAIN
Call 214-556-0555 or Email Us to make an appointment with our expert cervical kyphosis doctors.
Diagnosis
Diagnosing cervical kyphosis involves a comprehensive approach that starts with a detailed patient history followed by a physical examination, and is then supplemented with imaging tests. Here’s a breakdown of each step:
Gathering a Complete Patient History
The diagnostic process begins by capturing a thorough history of the patient’s condition. This includes filling out a detailed form that covers all aspects related to neck pain or discomfort. The patient will be asked to recall and document any relevant incidents, symptoms, or previous treatments. During the consultation, the physician will explore these details further by asking specific questions to clarify the onset, nature, and severity of the pain.
Conducting a Physical Examination
A physical exam is crucial to assessing the extent of the kyphosis and its impact on neck mobility. During this exam, the doctor will:
- Assess the range of motion in the neck, checking how well the patient can bend, roll, and twist their head.
- Look for any signs of tenderness or muscle spasms around the neck and shoulder areas.
- Evaluate the neurological functions that might be affected by cervical kyphosis, including testing for numbness in the arms and hands, checking reflexes, and assessing muscle strength in the arms, hands, and legs.
Imaging Tests
After the initial assessments, imaging tests play a pivotal role in confirming the diagnosis of cervical kyphosis. The first line of imaging is usually an X-ray, which provides clear images of the cervical spine’s bones. X-rays help in identifying any bone-related abnormalities such as fractures, infections, tumors, or degenerative changes. They also give insights into the degree of kyphosis and the presence of cervical spinal stenosis.
Through this systematic approach—combining patient history, physical examinations, and diagnostic imaging—a definitive diagnosis of cervical kyphosis can be formed. This allows for appropriate treatment plans to be developed aimed at managing symptoms and preventing further complications such as paralysis.
Additional Diagnostic Tests
In some cases, your doctor may require additional diagnostic tests to evaluate the functional impact of cervical kyphosis or to rule out other underlying conditions. These tests may include:
- Electromyography (EMG): EMG involves the measurement of electrical activity in the muscles. It can help determine if any nerve root or peripheral nerve abnormalities are contributing to muscle weakness or sensory deficits.
- Nerve Conduction Studies: Nerve conduction studies assess the speed and strength of electrical signals as they travel through the nerves. This test can identify any nerve damage or dysfunction that may be associated with cervical kyphosis.
- Blood Tests: Blood tests may rule out certain medical conditions that could contribute to spinal abnormalities, such as infections, inflammatory diseases, or metabolic disorders.
Non-Surgical Treatment Options
- Physical Therapy: Physical therapy plays a crucial role in the non-surgical management of cervical kyphosis. A skilled physical therapist will design a personalized exercise program to strengthen the neck muscles, improve flexibility, and promote better posture. These exercises can help alleviate pain, enhance stability, and enhance the range of motion in the cervical spine.
- Pain Management medications: In cases where cervical kyphosis causes significant pain and discomfort, your doctor will implement pain management techniques. Nonsteroidal anti-inflammatory drugs (NSAIDs) or muscle relaxants can help reduce inflammation and relieve muscle spasms. Additionally, the use of heat or cold therapy, transcutaneous electrical nerve stimulation (TENS), or ultrasound therapy may provide temporary relief.
- Bracing: For individuals with mild cervical kyphosis, our doctors may recommend wearing a cervical brace or collar. These devices help provide external support and restrict neck movement, allowing the spine to heal and gradually regain proper alignment. Bracing is often used in combination with physical therapy to achieve the best results.
- Heat and Ice Therapy: Applying heat can soothe stiff muscles, while ice can alleviate swelling and pain.
- Epidural Injections: These are often administered to manage inflammation and pain by delivering medication directly around the spinal nerves.
- Lifestyle Modifications: Adjusting daily habits, such as improving ergonomics of workstations and taking frequent breaks from screen time, can significantly reduce symptoms.
By combining these treatments, orthopedic surgeons aim to relieve discomfort and prevent future issues associated with tech neck.
Surgical Treatment Options:
If the kyphosis appears flexible, the decision to conduct surgery will depend on the progression of the curve and the amount of pain incurred. If the curve and pain are minor, surgery may not be recommended even if the deformity looks unattractive. Often, if the deformity appears severe and chronic pain exists, surgery may be a good option.
Doctors do not usually recommend surgery when the deformity appears fixed (inflexible but not worsening) and if there are no problems with the nerves or spinal cord. On the other hand, if a fixed deformity has problems from pressure on the spinal cord, the need for surgery becomes greater. To clarify, a surgical correction is a very difficult type of treatment and one that only skilled surgeons should perform for cervical kyphosis.
Surgery to treat cervical kyphosis usually involves spinal fusion combined with segmental instrumentation. This means that some type of metal (titanium) plate or rod holds the spine in the proper alignment to straighten it. Surgery may require two procedures during the same operation. First, surgery on the front of the spine will relieve the pressure on the spinal cord. The second procedure, done through the back, fuses the spine and prevents kyphosis from returning.
Methods and Procedures
- Decompression and Fusion: In cases where non-surgical methods fail to improve symptoms or when cervical kyphosis is severe, surgical intervention may be necessary. One common surgical procedure is decompression and fusion. During this procedure, the surgeon removes any bone spurs, herniated discs, or other structures that may be compressing the spinal cord or nerves. The affected vertebrae are then fused using bone grafts or implants to restore stability and alignment.
- Osteotomies: In certain situations, cervical kyphosis may require more extensive surgical correction, such as osteotomies. This procedure involves removing a wedge-shaped piece of bone from the vertebrae to allow for realignment. Osteotomies are typically performed in severe cases of cervical kyphosis where the abnormal curvature is significant.
- Artificial Disc Replacement: Another surgical option for cervical kyphosis is artificial disc replacement. This procedure involves replacing a damaged or diseased disc in the cervical spine with an artificial disc implant. Artificial disc replacement aims to preserve motion in the cervical spine while correcting abnormal curvature. This procedure is typically reserved for select cases and requires careful patient selection.
Post-Surgical Rehabilitation: Following surgery, a comprehensive rehabilitation program is crucial for optimal recovery. Physical therapy is typically prescribed to improve strength, flexibility, and range of motion. Rehabilitation aims to help patients regain function, adapt to the changes in the spine, and prevent future complications.
Physical Therapy
Your doctor may have you work with a physical therapist. A well-rounded rehabilitation program assists in calming pain and inflammation, improving your mobility and strength, and helping you do your daily activities with greater ease and ability.
Exercise has not proven helpful for changing the kyphotic curve in the neck. However, it can help provide pain relief. Therapy sessions may be scheduled two to three times each week for up to six weeks.
The goals of physical therapy are to help you
- learn correct posture and body movements to counteract the effects of kyphosis
- maintain appropriate activity levels
- maximize your neck range of motion and strength
- learn ways to manage your condition
Learn more about spinal rehabilitation.
Living with Cervical Kyphosis:
With proper treatment and lifestyle changes, many people with cervical kyphosis can manage their condition effectively and live active lives. Early diagnosis and intervention are key to preventing complications. Here are some tips for managing cervical kyphosis:
- Maintain good posture: Be mindful of your posture throughout the day, especially when sitting or using electronic devices.
- Strengthen your core: A strong core helps support your spine and reduce strain on the neck.
- Regular exercise: Staying active with exercises that promote flexibility and strength can be beneficial.
- Maintain a healthy weight: Excess weight can put additional strain on your spine.
- Use ergonomic aids: Invest in ergonomic chairs and workstations that promote good posture.
- Manage stress: Stress can worsen pain, so consider relaxation techniques like yoga or meditation.
Why Choose Southwest Scoliosis and Spine Institute
Part of diagnosing, evaluating, and treating a patient with cervical kyphosis requires a number of variables. Along with the patient’s age, curvature location, and type of scoliosis, regardless of severity, the sooner treatment starts, the better the prognosis for treatment. Unfortunately, a cure for cervical kyphosis does not exist, but the tools exist to treat it. At The Southwest Scoliosis and Spine Institute, with offices in Dallas, Plano, and Frisco, Texas, we tailor each and every treatment plan to suit the specifics of each patient’s condition.
We employ a variety of treatment modalities so that our patients may receive various types of care, and we also refer patients for physical therapy, rehabilitation, and corrective bracing specifically for cervical kyphosis. As we work with a patient during their treatment, we keep track of how they are progressing and adjust the treatment plan as needed based on their condition. If you are in pain, call us to make an appointment.
____________________
Citations: Medical News Today – Cervical Kyphosis
The medical content on this page has been carefully reviewed and approved for accuracy by the Southwest Scoliosis and Spine Institute’s qualified healthcare professionals, including our board-certified physicians and Physician Assistants. Our team ensures that all information reflects the latest evidence-based practices and meets rigorous standards of medical accuracy, with oversight from our expert spine doctors to guarantee reliability for our patients.
If you or a loved one suffers from spinal pain, you owe it to yourself to call Southwest Scoliosis and Spine Institute at 214-556-0555 to make an appointment.


