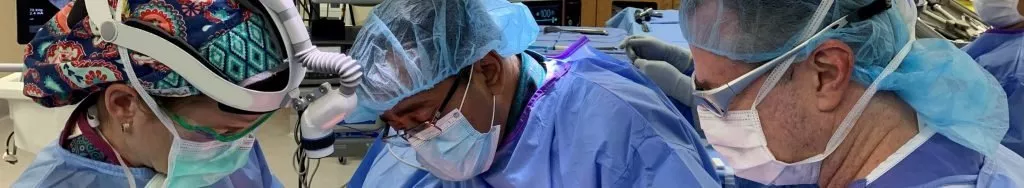
LUMBAR HERNIATED DISC
At the Southwest Scoliosis and Spine Institute, our expert Lumbar Herniated Disc Doctors are dedicated to diagnosing and treating spinal problems in children and adults and ensuring comprehensive care tailored to each patient’s needs. With advanced techniques and a compassionate approach, our team is here to diagnose, treat, and care for patients suffering from Lumbar Herniated Discs.
3 percent of individuals with progressive curvature may eventually experience severe problems that can include scoliosis and back pain, spinal problems, and nerve compression causing numbness, weakness, and leg pain.
Lumbar Herniated Disc Explained
Watch Dr. Devesh Ramnath explain “Is a fairly common condition that people will come to see me for. It is when the gel between your vertebra herniate out and will compress the nerve canal.”
Lumbar Herniated Disc
 Southwest Scoliosis and Spine Institute’s board-certified, fellowship-trained orthopedic doctors, Richard Hostin, MD, Devesh Ramnath, MD, Ishaq Syed, MD, Shyam Kishan, MD, and Kathryn Wiesman, MD, have years of experience treating thousands of patients with complex spine conditions, including herniated lumbar discs.
Southwest Scoliosis and Spine Institute’s board-certified, fellowship-trained orthopedic doctors, Richard Hostin, MD, Devesh Ramnath, MD, Ishaq Syed, MD, Shyam Kishan, MD, and Kathryn Wiesman, MD, have years of experience treating thousands of patients with complex spine conditions, including herniated lumbar discs.
A herniated disc normally happens due to aging or normal wear and tear. The outer layer of tissue holding the disc in place can gradually degrade over time (a condition known as degenerative disc disease). Also, a herniated lumbar disc may result from a traumatic injury, but this is less common.
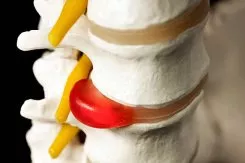
To understand how a herniated disc differs from other back pain issues, it’s helpful to know more about the spine’s anatomy. The intervertebral discs are positioned between each vertebra and act as shock absorbers. Each disc comprises a strong outer ring called the annulus and a soft, jelly-like center known as the nucleus pulposus. A disc herniation occurs when the annulus tears and the nucleus pulposus material pushes out, potentially pressing on nerves in the spinal canal.
Question and Answer
What are the Symptoms of a Lumbar Herniated Disc?
The symptoms of a lumbar herniated disc can include lower back pain, leg pain, numbness or tingling in the legs or feet, and weakness in the legs. The severity of the symptoms can vary depending on the location and severity of the herniation.
How do you diagnose a Lumbar Herniated Disc?
Doctors typically diagnose a lumbar herniated disc through a combination of physical examination, imaging tests such as MRI or CT scans, and nerve function tests. Your doctor may also ask about your medical history and any other symptoms existing..
What are the non-surgical treatments for a Lumbar Herniated Disc?
Non-surgical treatments for a lumbar herniated disc may include physical therapy, pain management, and the use of lumbar traction or braces to support the back.
Understanding How a Herniated Disc Occurs
To fully understand how a herniated disc occurs, it’s helpful to delve into the anatomy of the spine, particularly the intervertebral discs. These discs serve as essential shock absorbers between each vertebra, ensuring smooth movement and flexibility. Each disc has two main parts:
- Annulus Fibrosus: The disc’s tough outer ring, composed of strong fibers, acts as a ligament connecting each vertebra. This part provides structural integrity and strength to the disc.
- Nucleus Pulposus: The inner, jelly-like core, primarily made of water and collagen fibers, this component acts as the main shock absorber.
A herniated disc happens when the annulus fibrosus is damaged, allowing the nucleus pulposus to rupture out of its normal space. If the annulus tears near the spinal canal, the nucleus material can intrude into this area, potentially causing pain and other symptoms. Understanding these anatomical features is crucial for understanding how the spine functions and what happens when it suffers a herniated disc.2
Causes of Herniation
A herniated disc normally happens due to aging or normal wear and tear. The outer layer of tissue holding the disc in place can gradually degrade over time (a condition known as degenerative disc disease). Also, a herniated lumbar disc may result from a traumatic injury, but this is less common.3
While children rarely experience herniated discs, young and middle-aged adults are more prone to this condition. In older adults, the natural degenerative changes that occur with aging actually reduce the likelihood of developing a true herniated disc. The following identifies the most common occurrences:
- Sudden Trauma: A disc can rupture if subjected to excessive pressure suddenly. For example, falling from a height and landing awkwardly can apply immense force on the spine, potentially leading to a disc rupture or even a vertebral fracture.
- Everyday Activities: Actions like bending over or lifting heavy objects also exert significant pressure on spinal discs. If the force is too great, it can cause a disc to rupture.
- Cumulative Injury: Repeated minor injuries over time can weaken the annulus fibers of the disc. As these fibers degrade, a seemingly minor movement or lift can apply too much pressure, causing the weakened disc to rupture.
In summary, while age-related wear is a common cause, other factors such as sudden injuries and cumulative stress from repeated activities also contribute to the risk of a herniated disc. Understanding these causes can aid in adopting preventive measures to protect spinal health.
Lumbar Herniated Disc Symptoms
Symptoms of a herniated lumbar disc include:
- Lower back pain
- Difficulty lifting the feet when walking or standing, which is called foot drop
- Painful tingling or feelings like electric shocks, usually in the buttocks and legs
- Pain radiating into one or both legs
- Numbness or tingling in the leg areas
- Muscle weakness in certain leg muscles
- Loss of reflexes in one or both legs
The symptom’s location can help pinpoint which disc is affected, as they correlate to specific nerve roots in the lumbar spine. By understanding the specific causes, doctors can better differentiate it from other types of back pain, allowing for more accurate diagnosis and treatment.4
The Lumbar Spine
Usually, the first (and by far the most common) symptom of a herniated lumbar disc is located in the lumbar spine. This part of the spine is located in the lower back area. This condition also normally presents with pain in the lower back. When a lumbar disc herniation presses on the nerves, it can lead to a condition known as sciatica. The discs in your back are like shock absorbers. When these shock absorbers lose the fluid inside, the bones start to rub together. Sometimes it may pinch the closest nerve and cause pain. Hence, it will cause pain and possibly numbness, tingling, or weakness in the buttocks and down the back of the legs.5
When a herniated disc presses on nearby nerves, it can cause pain, numbness, and weakness where the nerve(s) travel. If it isn’t pressing on a nerve, you may only experience minor pain or even no pain at all. In severe cases, this condition can lead to a loss of bladder or bowel control. While this is rare, doctors will recognize this as a serious condition requiring immediate medical attention.
Complications Before Surgery
Even before surgery, a herniated disc can lead to significant complications. One of the most serious is the development of cauda equina syndrome. This occurs when a large fragment of disc material ruptures into the spinal canal, affecting the nerves that control bowel and bladder functions.
What to Watch For
- Permanent Nerve Damage: Pressure on these nerves can cause irreversible damage, potentially leading to a loss of bowel and bladder control. This is a critical issue that necessitates emergency medical intervention.
- Urgency of Treatment: If cauda equina syndrome is suspected, surgery is often recommended immediately to relieve the pressure on these crucial nerves.
Fortunately, such severe complications are rare, but awareness and prompt attention are key to preventing lasting effects.
Diagnosing a Lumbar Herniated Disc
When you come to Southwest Scoliosis and Spine Institute, your doctor will start by going over your medical history and performing a thorough physical exam, looking for any difficulty walking or pain in the lower back. Furthermore, they may ask you to do a leg raise test to see if you are experiencing a ‘foot drop’ or other neurological symptoms.
The doctor will confirm a diagnosis of lumbar disc herniation using X-ray imaging, computed tomography (CT) scans, and/or magnetic resonance imaging (MRI). Because X-ray imaging can only show issues with the bones themselves and not the soft tissue, the doctor may order a CT or MRI scan to confirm the condition.
Our practice uses an advanced low-dose radiation X-ray imaging system that takes high-quality images of patients in under a minute. In addition, it can also take X-rays of patients in multiple positions, and it’s conveniently located inside our Dallas location, which means that you and your doctor can review the X-rays right after they are taken, during your appointment.
When evaluating the sources of pain, particularly in cases where MRI results are inconclusive, doctors may order additional tests. If there’s doubt about whether a herniated disc is causing discomfort, healthcare providers often suggest further testing to gather a comprehensive understanding.
Myelogram
A myelogram, typically used alongside a CT scan, is among these recommended examinations. This approach can uncover details that an MRI might miss, ensuring a more accurate diagnosis. In situations where pinpointing nerve damage is crucial, doctors may order tests such as Electromyography (EMG) or Somatosensory Evoked Potentials (SSEP). These electrical tests are instrumental in confirming that leg pain is indeed nerve-related.
Such in-depth testing can provide critical insights needed before making decisions about surgical interventions.6
Treatment for Lumbar Disc Herniation At Our Offices in Dallas, Plano, and Frisco, TX
Fortunately, most patients do not require surgery for a herniated lumbar disc. Similarly, they will improve with nonsurgical treatment over a period of days or weeks. In most cases, patients fully recover within 2-4 months, though the pain may return on and off while they recover.
Nonsurgical Treatment
At the Southwest Scoliosis and Spine Institute, our physicians always try to take a conservative approach to treatment before considering surgery. Above all, the doctor will consider all options, and treatment will depend largely on the patient’s age, health, and condition.7
Moreover, non-surgical treatments for lumbar disc herniation include:
- Staying active. The best way to help reduce swelling and ease the pain is just to do low-intensity activities like walking. Staying off your feet for a few days is usually advised, but most doctors do not recommend bed rest for more than 1-2 days. It’s also important to avoid sitting for long periods of time. Observation and Rest as a Recovery Strategy:
- Monitor Progress: Keep an eye on your symptoms. If your pain is manageable and there’s no increase in weakness or numbness, doctors might decide to observe the patient. This approach allows you to gauge whether the issue is stabilizing or requires further intervention.
- Balancing Rest and Activity: If the pain intensifies, consider taking a break from work and reducing your activities temporarily. This initial rest period can help manage severe discomfort.
- Gradual Mobilization: After a few days of rest, begin to gently mobilize yourself. Start with a walking program, gradually increasing your distance each day. This helps in maintaining flexibility and preventing stiffness while still respecting your body’s need to heal.
Management
By integrating careful observation with a balanced rest and activity plan, you can effectively manage your recovery process and support your body’s natural healing mechanisms.
- Physical therapy. Your doctor may recommend that you see a physical therapist. However, your doctor may recommend exercises to help strengthen and stabilize the muscles of the lower back and abdomen.
- Non-steroidal medications. Over-the-counter medications help reduce swelling and pain. Your doctor may also prescribe extra-strength versions for a short period of time.
- Epidural steroid injection. Injections of steroidal drugs near affected nerves can help by providing short-term pain relief and further reducing inflammation.
What Types of Pain Medications Are Used to Manage Herniated Disc Pain?
When managing herniated disc pain, there are several types of medications available, each with its own benefits and considerations.
Over-the-Counter Options
- Non-Prescription Pain Relievers: These include drugs like ibuprofen and acetaminophen, which reduce mild to moderate pain and inflammation. Always adhere to dosage instructions to prevent any adverse effects.
Prescription Medications
- Non-Narcotic Pain Medications: These are typically prescribed when over-the-counter options are not sufficient. While less addictive, they will not control pain as compared to their narcotic counterparts.
- Narcotic Pain Relievers: For severe pain, doctors might prescribe narcotic medications. These are potent in managing pain but come with a high risk of addiction. Physicians generally limit their use to short durations.
Each medication type provides varying levels of pain control, and the choice largely depends on the severity of the pain and the patient’s medical history. Always consult with a healthcare professional to determine the best approach for your specific situation.
Surgery for Lumbar Herniated Disc
Only a small percentage (about 10-15%) of patients with lumbar disc herniation require surgery. Herniated disc surgery is typically recommended if nonsurgical treatment has not relieved painful symptoms.
Surgical treatment includes:
- Lumbar discectomy. This procedure involves removing any affected disc(s) through an incision in the back. This surgery is often the best option when there is more than one herniated disc on different levels of the spine.
- Microdiscectomy. Typically used when there is just a single herniated disc, a microdiscectomy is a minimally invasive version of a discectomy. Using a much smaller incision, the surgeon operates with the use of a thin tube with a microscopic camera on the end. Like the regular discectomy, any herniated portion of the disc is removed.
- Lumbar laminectomy. This procedure commonly accompanies a discectomy/microdiscectomy, as it gives the surgeon access to the herniated disc. During a laminectomy, a small opening is made in the lamina, which is the back part of the vertebra that covers the spinal canal.
The surgical procedure begins with an incision along the center of the back over the affected area. Once the incision is made, muscles are gently moved aside to expose the vertebrae. Surgeons may use X-rays to ensure they are working on the correct vertebra. A key step in the procedure involves creating a small opening between the vertebrae where the disc has ruptured, allowing the surgeon to see into the spinal canal.8
Conclusion
During the procedure, the surgeon carefully moves the nerve roots to locate and remove the disc material that has protruded into the spinal canal, alleviating any pressure on the spinal nerves. In addition, any excess nucleus pulposus material inside the disc is removed to help prevent future herniations.
Spinal stabilization
After the disc is removed through a discectomy, the spine may need stabilization via a spinal fusion procedure. The doctor uses bone grafts, screws, rods, etc., to hold the vertebrae in place while they heal.
Once the operation is complete, the muscles are returned to their natural position, and the skin incision is closed using sutures or metal staples, ensuring a secure and neat closure. This comprehensive approach ensures that the surgery not only addresses the immediate issue but also reduces the risk of future complications.
What Complications Might Occur During Surgery for a Herniated Disc?
Undergoing surgery for a herniated disc carries certain risks, as with any surgical procedure. The primary concerns are linked to anesthesia and potential complications during the operation itself.
Anesthesia Risks
Every surgery requires anesthesia, which carries its own set of potential risks. These may include allergic reactions or adverse effects on the heart and respiratory system.
Nerve Damage
One significant risk is nerve injury. Surgeons must navigate around the intricate web of spinal nerves while removing the disc. Accidental damage to these nerves could lead to permanent issues, such as:
- Numbness: Loss of sensation in certain areas.
- Weakness: Diminished muscle strength.
- Chronic Pain: Persistent discomfort where the nerve pathways extend, especially in the legs.
Dural Tear
The spinal cord and nerves are encased in a protective layer called the dura mater. During the operation, a tear in this protective covering may occur, which is not uncommon in spinal surgeries. If noticed during the procedure, repairs can occur promptly. Failure to detect and fix the tear might lead to:
- Spinal Fluid Leak: Continuous leakage can cause headaches.
- Infection Risk: Continued leakage increases the chance of infections such as spinal meningitis.
In cases where a dural tear does not heal naturally, doctors will schedule a follow-up surgery to correct the issue.
Conclusion
Being aware of these potential complications helps in understanding the risks associated with herniated disc surgery. Always discuss these possibilities with your healthcare provider to make informed decisions.
Complications of Herniated Disc Surgery
When considering surgery for a herniated disc, understanding the potential complications is crucial for informed decision-making. Let’s delve into what you might encounter before, during, and after the procedure.
Before Surgery
Even before the surgical intervention, there are risks associated with a herniated disc. One serious risk is cauda equina syndrome. This occurs when a large fragment of the disc presses on the nerves that manage essential functions like bowel and bladder control. Though rare, it can lead to permanent loss of these functions if not addressed promptly with surgery.
During Surgery
Surgical procedures carry inherent risks, and disc surgery is no exception. One primary concern is complications from anesthesia, which are present in any surgery. Specific issues related to herniated disc removal include:
- Nerve Injury: Navigating the delicate spinal nerves to access the disc can sometimes lead to nerve damage. This might result in long-term numbness, weakness, or even pain in an affected leg.
- Dural Tear: The spinal cord and nerves are enveloped by a protective sleeve called the dura mater. A tear in this covering can occur during the procedure. Although often repairable during surgery, if unnoticed, it may lead to spinal fluid leaks, causing headaches and potentially increasing the risk of infections like spinal meningitis.
After Surgery
Post-surgical complications might arise immediately or might only become apparent after several months:
- Infection: There’s a risk of infection at the incision site, within the disc, or surrounding spinal nerves. Superficial infections usually respond well to antibiotics, while deeper infections may necessitate additional surgery.
- Re-herniation: The same disc might recur in about 10-15% of cases, especially within the first six weeks post-surgery. If symptomatic, this might require another surgical intervention.
- Persistent Pain: Surgery does not guarantee pain relief. Pre-existing nerve damage from the herniated disc might not fully resolve, or scar tissue could develop and mimic pre-surgery pain. Additionally, untreated back issues might continue to cause discomfort.
- Degenerative Disc Disease: Surgery can lead to degeneration at the operated spinal segment. This degeneration might necessitate further surgical treatment if severe pain develops over time.
Being aware of these potential complications will help you weigh the risks and benefits with your healthcare provider and make an informed decision regarding your treatment.
Understanding Re-Herniation and Its Management After Surgery
When it comes to spinal surgery, particularly for herniated discs, there’s always some risk of re-herniation. Statistically, the likelihood ranges between 10 and 15 percent. This recurrence is more probable within the first six weeks post-operation, although it can happen at any time.
Managing Re-Herniation
- Post-Operative Care: Following your surgeon’s recovery guidelines diligently can reduce the risk. This includes rest, physical therapy, and a gradual return to daily activities.
- Monitoring Symptoms: Stay vigilant for symptoms such as recurring pain, numbness, or weakness. Early detection can lead to quicker management.
- Potential for Re-Operation: If re-herniation occurs and symptoms significantly impact your quality of life, a second surgical intervention may become necessary.
Preventive measures and early intervention strategies are essential for optimal recovery and management. Collaborate closely with your healthcare provider to ensure the best outcomes after initial surgery.
Why Is Rehabilitation Important After Surgery for a Herniated Disc?
Rehabilitation plays a crucial role in the recovery process following surgery for a herniated disc. Engaging with a physical therapist and adopting a structured exercise regimen is essential not just for immediate recovery but for long-term spinal health.
The Importance of Exercise in Recovery
Exercise is indispensable in the recovery journey for a herniated disc. Regular physical activity aids in bolstering the muscles surrounding the spine, providing necessary support and stability. Here’s how exercise helps:
- Strength Building: Strengthening your back, abdominal, arm, and leg muscles helps to minimize strain on the spine, which is essential for reducing pain and preventing future injuries.
- Improved Mobility: Stretching and flexibility exercises decrease the chances of muscle spasms and improve overall mobility.
- Pain Management: Engaging in aerobic exercises, which increase heart rate and circulation, can naturally alleviate pain. This is due to the release of endorphins, the body’s natural painkillers, which can help reduce discomfort.
Long-Term Benefits
Beyond the initial recovery, rehabilitation through exercise plays a role in maintaining spine health, aiding in risk reduction for further complications:
- Injury Prevention: A well-designed exercise routine tailored to your specific needs can significantly lower the likelihood of falls and related injuries.
- Bone Health: Weight-bearing exercises are particularly beneficial in preventing bone loss due to osteoporosis, thus reducing the risk of compression fractures.
Embracing rehabilitation as part of your lifestyle is not just about healing from surgery—it’s about fostering resilience against future spinal issues. By making exercise a permanent part of your health management strategy, you invest in a healthier, more active life.
Understanding Persistent Pain and Degenerative Disc Disease Post-Surgery
Even after undergoing surgery, some individuals continue to experience pain, and this occurs due to several factors:
- Nerve Damage: The nerves might have sustained damage due to the initial pressure from a herniated disc, and unfortunately, they may not fully recover.
- Scar Tissue Formation: Following the procedure, scar tissue can develop around the nerves. This sometimes mimics the pre-surgery pain, and doctors find it particularly difficult to manage.
- Unaddressed Back Issues: In some cases, pain could stem from other underlying back problems that surgery did not resolve.
The Role of Degenerative Disc Disease
Injury to a disc, including surgical intervention, can accelerate degeneration of the spinal segment involved. Here’s why:
- Disc Injury and Subsequent Degeneration: A surgically altered disc has indeed been injured, raising the likelihood of degeneration.
- Increased Risk of Further Complications: Over time, the area where a disc was removed is more susceptible to additional issues, potentially necessitating further surgery. Especially if the degenerative process leads to severe pain.
These post-surgery challenges highlight the importance of a comprehensive treatment plan and ongoing care to manage potential complications.
How Does an Endoscopic Discectomy Work, and What Are Its Advantages?
Endoscopic discectomy is a cutting-edge surgical technique that has transformed spinal surgery. This minimally invasive procedure involves inserting a tiny, specialized camera, called an endoscope, into the spinal canal. It does so through a small incision—typically about 1/4 inch. This endoscope is equipped with magnification capabilities that provide surgeons with a clear, detailed view of the spinal discs on a monitor.
The Procedure
- Insertion: A small incision is made, and the endoscope, along with other precise surgical instruments, is inserted into the spinal area.
- Visualization: Instead of relying on a traditional microscope, the surgeon views the site on a TV screen. This allows for accurate maneuvering and removal of problematic disc material.
- Action: Specially designed instruments are directed to the affected area to carefully excise the disc material causing issues.
Advantages of Endoscopic Discectomy
- Minimally Invasive: Because it utilizes smaller incisions, there’s minimal disruption to surrounding tissues.
- Quicker Recovery: This gentle approach often results in faster healing times compared to traditional methods.
- Reduced Complications: With less tissue damage comes a lower risk of complications post-surgery.
This procedure is an evolution in the field of spine surgery. It parallels advancements seen with the arthroscope in knee surgeries and the laparoscope in gallbladder removals. Although still gaining widespread adoption, its potential for minimizing tissue damage and expediting recovery positions it as a promising development for those requiring spinal surgery.
Why Choose Southwest Scoliosis and Spine Institute

The Spine is the specialty of our doctors and surgeons at the Southwest Scoliosis and Spine Institute. We understand your concerns and can answer your questions regarding your condition. We know how to use our specialized knowledge, skills, and abilities to stop the pain. Our doctors and staff have many years of training and experience in Spine and Back Pain. We treat kids, adolescents, and adults and can help them get back to living the life they love.
The following are just a few of the many reasons why patients might choose Southwest Scoliosis and Spine Institute.
- Expertise in the spine: The team of specialists is spine experts. They specialize in the diagnosis and treatment of spinal conditions, ensuring the best possible care for their patients.
- Cutting-edge technology: Our practice uses the latest technology and techniques to diagnose and treat a wide range of conditions. In addition, we use minimally invasive procedures that reduce pain and promote faster recovery.
- Comprehensive care: Our practice offers a full range of services, from diagnostic imaging and physical therapy to surgery. We ensure that patients receive complete, seamless care for their spinal conditions.
- Dedicated facilities: Southwest Scoliosis and Spine Institute is dedicated to providing patients with a safe and comfortable environment.
Finally, our board-certified physicians and fellowship-trained orthopedic surgeons use the full range of treatments to treat our spine patients. Southwest Scoliosis and Spine Institute Doctors and Surgeons are Spine experts with offices in Dallas, Plano, and Frisco, Texas.
We offer cutting-edge technology, comprehensive care, and dedicated facilities to ensure the best possible care for our patients. Call today to make an appointment.
____________________
Citations
- Mayo Clinic – Herniated disk overview
- Cleveland Clinic – Herniated disk
- American Academy of Orthopaedic Surgeons – Herniated disk in the lower back
- MedlinePlus – Herniated disk
- Johns Hopkins Medicine – Herniated disk
- American Association of Neurological Surgeons – Herniated disc
- National Institute of Neurological Disorders and Stroke – Herniated disk information page
- North American Spine Society – Lumbar disc herniation clinical guideline
The medical content on this page has been carefully reviewed and approved for accuracy by the Southwest Scoliosis and Spine Institute’s qualified healthcare professionals, including our board-certified physicians and Physician Assistants. Our team ensures that all information reflects the latest evidence-based practices and meets rigorous standards of medical accuracy, with oversight from our expert spine doctors to guarantee reliability for our patients.
We’re here to help STOP THE PAIN
If you are an adult living with scoliosis or have a child with this condition and need a doctor who specializes in orthopedic surgery,
call the Southwest Scoliosis and Spine Institute at 214-556-0555 to make an appointment today.


