EPENDYMOMA TUMORS
An Ependymoma is a slow-growing tumor in the spinal cord. Because it originates in your spinal cord and spreads, it is known as a primary central nervous system tumor.
At the Southwest Scoliosis and Spine Institute, our expert Ependymoma Doctors and Surgeons are dedicated to treating spinal problems, We treat children and adults to ensure comprehensive care tailored to each patient’s needs. With advanced techniques and a compassionate approach, our team diagnoses, treats, and cares for patients suffering from an Ependymoma Tumor.
3 percent of individuals with progressive curvature may eventually experience severe problems that can include scoliosis and back pain, spinal problems, and nerve compression causing numbness, weakness, and leg pain.
Spinal Ependymoma
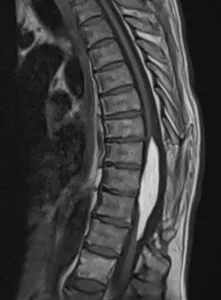 Ependymoma is a slow-growing tumor in the spinal cord. Because it originates in your spinal cord as opposed to somewhere else and spreads, it is known as a primary central nervous system tumor. Beyond your brain or spinal cord, these cancers often don’t metastasize. Children are more likely than adults to develop them as they grow. Ependymomas are intramedullary tumors, which implies that they develop within the actual spinal cord’s tissue.
Ependymoma is a slow-growing tumor in the spinal cord. Because it originates in your spinal cord as opposed to somewhere else and spreads, it is known as a primary central nervous system tumor. Beyond your brain or spinal cord, these cancers often don’t metastasize. Children are more likely than adults to develop them as they grow. Ependymomas are intramedullary tumors, which implies that they develop within the actual spinal cord’s tissue.
Including the cervical (neck), thoracic (upper back), and lumbar levels of the spinal cord, they can happen anywhere (lower back). The lower lumbar and sacral area (base of the spine, above the tailbone) is where certain ependymomas, sometimes referred to as myxopapillary filum terminals ependymomas, develop. Below the spinal cord, this structure is a thin, fibrous thread that aids in spinal cord stability. Only surgeons with vast experience should consider removing ependymomas in this region.
Types of Ependymomas
Your doctor at Southwest Scoliosis and Spine Institute will discuss the sort of ependymoma you or your child has. Based on where your tumor is located and how quickly it spreads, there are four different types.
Subependymomas (grade I)
These often develop slowly and appear close to a ventricle in the brain. Adults and elderly males experience them most frequently.
Myxopapillary Ependymomas (grade II)
These most frequently affect young adults’ spinal cords. Their growth is sluggish.
Ependymomas (grade III)
The brain is where this ependymoma tumor, which is the most prevalent kind, often develops.
Anaplastic Ependymomas (grade IV)
These tumors frequently have a bad prognosis and develop quickly. Additionally, they frequently grow in the region of the brain that houses the brain stem and cerebellum. The posterior fossa is the name given to this region of the brain.
Questions and Answers
What is a Spinal Ependymoma
A spinal ependymoma is a type of tumor that originates from the ependymal cells lining the spinal cord or the central canal within the spinal cord. These tumors are typically slow-growing and benign, meaning they are not cancerous in nature. However, in some cases, they can be malignant or have the potential to become cancerous.
What are the symptoms of Spinal Ependymoma
The symptoms of a spinal ependymoma can vary depending on the location and size of the tumor. Common symptoms may include:
- Back or neck pain: Pain in the affected region of the spine is a common symptom, often localized to the area where the tumor is present.
- Radiating pain: The tumor may compress or irritate nearby nerves, leading to radiating pain that can extend to the arms, legs, or other parts of the body.
- Sensory changes: Numbness or tingling sensations may occur in the areas supplied by the affected nerves.
- Muscle weakness: Weakness or difficulty with coordination and fine motor skills can result from the tumor’s pressure on the spinal cord or nerve roots.
- Bowel or bladder dysfunction: In some cases, spinal ependymomas can cause changes in bowel or bladder function, such as urinary incontinence or difficulty controlling bowel movements.
- Balance and gait problems: Tumors affecting the lower spinal cord can interfere with balance and walking.
How are Spinal Ependymomas diagnosed and treated?
Diagnosing and treating spinal ependymomas typically involves the following:
-
Diagnosis: The diagnostic process may include a thorough medical history review, physical examination, and imaging tests such as MRI or CT scans. These imaging studies can help visualize the tumor and determine its location, size, and relationship to surrounding structures.
-
Biopsy: In some cases, a biopsy may be performed to obtain a tissue sample for further analysis to confirm the diagnosis and determine the tumor’s grade or aggressiveness.
-
Treatment: The primary treatment for spinal ependymomas is the surgical removal of the tumor whenever feasible. The goal of surgery is to achieve complete resection while preserving neurological function. In cases where complete removal is not possible, radiation therapy may be used to control tumor growth or reduce the risk of recurrence. Chemotherapy may also be considered for certain cases, particularly for aggressive or metastatic tumors.
It’s important to note that not all spinal ependymomas require immediate intervention. Because many of these tumors are benign and slow-growing, some are discovered incidentally—meaning they are found during imaging for unrelated reasons and may not be causing any symptoms. If the tumor is small and not compressing the spinal cord, a “watch and wait” approach may be recommended. This involves close monitoring with regular MRI scans, sometimes annually, to track any changes in size or symptoms over time. Several years may pass before the tumor grows large enough to warrant treatment.
For tumors that are larger or begin to cause symptoms—such as pain, weakness, or neurological changes—timely treatment is generally advised to prevent further complications and to preserve spinal cord function.
Causes of Ependymoma
The average age at which a spinal ependymoma develops is 39 years. However, roughly one in four tumors appears before the age of 18. Males are more likely than females to develop a spinal ependymoma. However, it is unclear why this is the case. Spinal ependymomas are intramedullary tumors that form inside the spinal cord, as we noted above. They can grow in several different locations inside the cord, though.
The majority of ependymomas are present in the cervical cord, where they grow in roughly 44 percent of cases. The thoracic cord alone accounts for around 26% of the development. The cervical cord and upper thoracic cord together account for another 23%.
How Common are Ependymomas?
Nearly 22 out of every 100,000 persons, according to experts, have primary central nervous system malignancies. Ependymomas represent all main central nervous system tumor diagnoses:
- 2% or less of adult diagnoses.
- 4% of 15 to 19-year-old youngsters receive a diagnosis.
- Almost 6% of pediatric diagnoses from birth to age 14
Can Spinal Ependymomas Be Monitored Without Immediate Treatment?
Not all spinal ependymomas require immediate intervention. Because these tumors are often slow-growing and can remain benign for extended periods, doctors may recommend simply monitoring them, especially if you are not experiencing any symptoms. It’s common for spinal ependymomas to be discovered by chance during imaging for unrelated issues.
If the tumor is small and isn’t putting pressure on the spinal cord, your care team (such as at Southwest Scoliosis and Spine Institute) may suggest regular check-ups and annual MRI scans to watch for any changes. This “watchful waiting” approach can last for years without the need for surgery or other treatments, unless the tumor begins to grow or causes new symptoms. The goal is to avoid unnecessary procedures while ensuring your spine and nerves remain healthy.
Ependymoma Symptoms
Ependymal cells in the spinal cord’s inner core give birth to spinal ependymomas. They progressively exert pressure on the surrounding spinal cord by slowly expanding over an extended period of time, sometimes years. This compression of the spinal cord can cause pain symptoms at the tumor site. Numbness and tingling in the arms and legs; weakness and clumsiness in the arms and legs. The size and location of the spinal tumor affect the specific symptoms. In terms of onset and development, symptoms differ greatly.
They might be brief, sporadic, or persistently non-progressive. Since intramedullary spinal cord tumors are benign and slow-growing, they may go on for a long period without showing any symptoms. This may delay patient presentation for medical evaluation and diagnosis. Fortunately, most patients today are initially diagnosed with little or no neurological abnormalities. There are exceptions, and the onset and progression of symptoms may occur over a short period.
Diagnosis of Spinal Ependymomas
To determine if you have an ependymoma, the doctor could perform the following tests on you:
Physical exam
The doctor examines you and inquires about your health and past illnesses.
Neurological exam
To examine your spinal cord, brain, and nerves, the doctor will have you move about.
MRI
This scan takes detailed pictures of your organs. They will likely take pictures of the pigment that gathers around the cancer cells so that they are easier to see in the picture.
Spinal tap
In order to draw fluid from your spine, you will lie on your side while the doctor uses a needle. To look for cancers, lab technicians will examine them.
Biopsy
The only way to tell if a tumor is an ependymoma is to look for cancer cells on a small piece under a microscope. This happens during surgery. Also, the biopsy will tell your doctor about the type and grade of the tumor.
Ependymoma Risk Factors
Ependymoma’s origins are yet unknown. Both men and women are equally affected, and the majority of ependymomas develop between the ages of four and six. However, people of all ages, races, and sexes are susceptible to developing the tumors. Ependymomas are more likely to form in people with a hereditary disorder known as neurofibromatosis type 2.
While researchers still do not fully understand the causes of ependymoma, it’s important to note that these tumors can develop at any stage of life. Most commonly, they appear in adulthood—specifically during the fourth through sixth decades of life—but children and older adults can also be diagnosed. No clear environmental, lifestyle, or inherited factors have been identified aside from the increased risk seen in individuals with neurofibromatosis type 2. This rare genetic condition is known to predispose people to various types of tumors, including ependymoma.
In summary, ependymoma does not discriminate by gender, age, or ethnicity, and aside from certain genetic conditions, there are no known ways to predict who will develop this tumor.
Ependymoma Treatments
Treatments for Ependymoma include:
Ependymoma surgery to remove the tumor
To remove as much of the ependymoma as feasible, the Southwest Scoliosis and Spine Institute Orthopedic Surgeons will conduct surgery. The aim is to remove the entire spinal tumor, but occasionally the ependymoma lies close to delicate spinal tissue, making it too dangerous. Your child might not need any further therapy if the entire tumor is removed during surgery.
The neurosurgeon may suggest a different procedure to attempt to remove the remaining tumor if part of it is still present. For more aggressive cancers or in cases where the tumor cannot be completely removed, other therapies, such as radiation therapy, may be advised.
What does microsurgical removal of a spinal ependymoma involve?
Microsurgical removal is a common and effective approach for treating most spinal ependymomas, thanks to their typically slow-growing and noncancerous nature. During this procedure, the patient is placed under general anesthesia and carefully positioned—usually lying face down—to allow the surgeon optimal access to the spinal cord.
Using a high-powered surgical microscope and specialized, delicate instruments, the surgeon delicately opens the area around the spinal cord to expose the tumor. Throughout the operation, the surgical team closely monitors spinal cord function by employing advanced techniques, such as somatosensory evoked potentials (SSEP) and motor evoked potentials (MEP). These monitoring methods help ensure the safety of nearby nerves and reduce the risk of neurological complications during and after surgery.
The main goal is to remove the entire tumor while preserving as much normal neurological function as possible. In most cases, this technique allows for a thorough and precise excision, offering patients the best possible outcome with minimal impact on surrounding tissues.
How is spinal cord function monitored during surgery for spinal ependymoma?
During surgery to remove a spinal ependymoma, doctors use advanced monitoring techniques to help protect the spinal cord and nerves. Throughout the procedure, specialists track the spinal cord’s function with tools like somatosensory evoked potentials (SSEP) and motor evoked potentials (MEP). These methods allow the surgical team to watch for any changes in nerve signals in real-time. By closely observing these signals, the team can adjust their approach if needed, reducing the risk of injury and helping ensure the best possible outcome for the patient.
Radiation therapy
High-energy radiation, such as X-rays or protons, is used in radiation treatment to destroy cancer cells. During radiation therapy, your child lies on a table and a machine moves around your child, aiming beams at precise points in the spine. Radiation therapy may be recommended after surgery to prevent more aggressive tumor recurrence or if the neurosurgeon cannot completely remove the tumor.
A special technique helps the treatment irradiate the tumor cells, sparing as much of the surrounding healthy tissue as possible. Radiation treatment techniques, including conformal radiation therapy, intensity-modulated radiation therapy, and proton therapy, enable medical professionals to deliver radiation with care and accuracy.
Radiosurgery
Stereotactic radiosurgery, which is technically a form of radiation rather than surgery, concentrates several radiation beams on specific locations to destroy the tumor cells. When an ependymoma returns after surgery, doctors use radiation and radiosurgery to reduce and destroy the tumor.
Chemotherapy
To eliminate cancer cells, doctors will also use chemotherapy. Most instances of ependymoma don’t respond well to chemotherapy. Chemotherapy is only used after other treatments have failed, such as surgery and radiation, and is still pretty much trial and error. An example of this is when the tumor returns after treatment.
Clinical trials
Clinical trials are investigations of novel therapies. You have the opportunity to try the most recent treatments thanks to this research, but there may be unknown adverse effects. If your kid is qualified to take part in an FDA-approved research study, ask your doctor.
Targeted drug therapy
Drugs that target cancer cells are being investigated under approved FDA supervision. These could affect surrounding healthy cells less than other forms of treatment.
Ependymoma Recovery
Cancer treatment recovery can be a protracted and difficult process. Chemotherapy can make a person feel weak and nauseous. Sometimes after neurosurgery, patients feel worse than they did before the procedure. It’s typical to experience fatigue, confusion, weakness, and vertigo. However, if the procedure brings on the desired outcome, these other feelings will pass quickly.
Ependymoma Long-term Effects
In rare instances, ependymoma or surgical side effects might last a long time or be late. Anywhere in the body might experience these side effects, and they may appear months or years after surgery. Heart, lung, and secondary cancer issues are a few examples of the physical long-term impacts. Anxiety, sadness, or learning challenges are possible additional long-term impacts.
There may also be memory or cognitive problems. In order to check for any long-lasting effects, doctors will want to frequently follow a patient. In some cases, further examinations or tests are required to identify a problem. Different types of rehabilitation, such as physical treatment, hearing aids, or cognitive therapy, could be necessary for some people. In addition, hormonal imbalances and developmental problems may occur in children.
There is a 65 percent cure rate if the tumor can be entirely removed. Later on, though, more ependymomas may form. It may be challenging to treat recurrent ependymomas. A myxopapillary ependymoma often has a better prognosis than a classic or anaplastic variety. The prognosis for adults is often better than that of youngsters. However, with appropriate care, roughly 82% of those with ependymomas live for at least five years. Additionally, under FDA rules and regulations, there are ongoing clinical trials that evaluate novel therapies and examine ways to reduce the side effects of therapies.
Why Choose the Southwest Scoliosis and Spine Institute
Orthopedics and specifically the spine is a specialty of our doctors and surgeons. They understand your concerns, can answer your questions regarding your condition, and know how to use their specialized knowledge to assist you. Our Doctors and surgeons have many years of training and experience in Spine and Back Pain for kids, adolescents, and adults, and can help them get back to living the life they love.
The following are just a few of the many reasons why patients might choose the Southwest Scoliosis and Spine Institute.
- Expertise in the spine: They specialize in the diagnosis and treatment of spinal conditions, ensuring the best possible care for their patients.
- Cutting-edge technology: Our practice uses the latest technology and techniques to diagnose and treat a wide range of conditions. In addition, we use minimally invasive procedures that reduce pain and promote faster recovery.
- Comprehensive care: Our practice offers a full range of services, from diagnostic imaging and physical therapy to surgery. We ensure that patients receive complete, seamless care for their spinal conditions.
- Dedicated facilities: The Southwest Scoliosis and Spine Institute is dedicated to providing patients with a safe and comfortable environment.
Our Practice
Finally, our board-certified physicians and fellowship-trained orthopedic surgeons use the full range of treatments to treat their spine patients. Our fellowship-trained, board-certified expert orthopedic scoliosis surgeons, Richard Hostin, MD, Devesh Ramnath, MD, Ishaq Syed, MD, Shyam Kishan, MD, and Kathryn Wiesman, with offices in Dallas, Plano, and Frisco, Texas, offer cutting-edge technology, comprehensive care, and dedicated facilities to ensure the best possible care for their patients. Call today to make an appointment.
____________________
Citation: National Institute of Cancer – Spinal Ependymoma
The medical content on this page has been carefully reviewed and approved for accuracy by the Southwest Scoliosis and Spine Institute’s qualified healthcare professionals, including our board-certified physicians and Physician Assistants. Our team ensures that all information reflects the latest evidence-based practices and meets rigorous standards of medical accuracy, with oversight from our expert spine doctors to guarantee reliability for our patients.
We’re here to help STOP THE PAIN
If you are an adult living with scoliosis or have a child with this condition and need a doctor who specializes in orthopedic surgery,
call the Southwest Scoliosis and Spine Institute at 214-556-0555 to make an appointment today.



