PARS FRACTURES
Spondylolysis is a spine condition characterized by a defect or fracture in a specific part of a vertebra called the pars interarticularis. This small bone segment connects the facet joints, which are crucial for the spine’s flexibility and movement.
Often referred to as “pars defect” or “pars fracture,” this condition can compromise the structural integrity of the spinal column. The pars interarticularis links two other significant components of the vertebral ring—the pedicle and the lamina—which are essential for protecting the spinal cord located within the spine’s middle and posterior sections. Our Pars Fractures Doctors recognize the potential impact on spinal health and overall mobility.
Our Spine Center is staffed with Doctors, Specialists, Surgeons, Technicians and the very best nurses in the world.
Pars Fractures
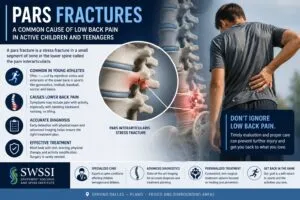
Pars fractures, also known as spondylolysis, are stress fractures that occur in the pars interarticularis. This is a small bony segment connecting the upper and lower parts of a vertebra. These fractures most commonly affect the lumbar spine (lower back) and can cause pain and instability. This comprehensive document aims to provide an in-depth understanding of the diagnosis and treatment of pars fractures.
 Pain and stiffness in the middle of the lower back indicate pars defect among other conditions as well. Pain normally gets worse with lumbar extension and twisting. Activity exacerbates symptoms, which subside with rest. Pain may radiate down one or both legs in certain patients. The nerves that exit the spinal canal near the fracture get compressed and irritated, resulting in discomfort. Numbness, tingling, and weakness in the legs are other possible side effects. The majority of individuals with a pars defect do not require surgery and can get relief through drugs and relaxation. Pain is treated with anti-inflammatory medicines and muscle relaxants. During the acute period of the injury, a patient should wear a lumbar corset back brace. When a patient gets diagnosed, physical therapy gets started. The therapist will begin PT by introducing a series of abdominal and low back muscle-building exercises.
Pain and stiffness in the middle of the lower back indicate pars defect among other conditions as well. Pain normally gets worse with lumbar extension and twisting. Activity exacerbates symptoms, which subside with rest. Pain may radiate down one or both legs in certain patients. The nerves that exit the spinal canal near the fracture get compressed and irritated, resulting in discomfort. Numbness, tingling, and weakness in the legs are other possible side effects. The majority of individuals with a pars defect do not require surgery and can get relief through drugs and relaxation. Pain is treated with anti-inflammatory medicines and muscle relaxants. During the acute period of the injury, a patient should wear a lumbar corset back brace. When a patient gets diagnosed, physical therapy gets started. The therapist will begin PT by introducing a series of abdominal and low back muscle-building exercises.
This page addresses the etiology, diagnosis, and treatment of various linked lumbar disorders. It explains and depicts the anatomy of the low back involved. By definition, facets are formed by two surfaces, one from each neighboring vertebra. And each vertebra has four separate joint surfaces in the back, two above the pedicles and two below the pars interarticularis (mirror images).
Questions and Answers
What constitutes a Pars Fracture?
A pars fracture, also known as spondylolysis, refers to a stress fracture that occurs in the pars interarticularis, a small bony segment connecting the upper and lower parts of a vertebra. It appears most commonly in the lower back (lumbar spine) and can result in instability and pain.
What Causes a Pars Fracture?
Repetitive stress or overuse of the spine appears as the most common cause of a pars fracture. As an example, all activities that involve hyperextension or repetitive twisting motions, such as gymnastics, football, weightlifting, or dance can cause a pars fracture. Traumatic injuries, such as falls or accidents, can also lead to pars fractures.
How do doctors diagnose and treat a Pars Fracture ?
Diagnosis of a pars fracture typically involves a combination of medical history, physical examination, and imaging studies. X-rays, CT scans, or MRI scans allow doctors to visualize the fracture and assess its severity. Treatment options vary depending on the severity of the fracture and the individual’s symptoms. Conservative treatment, including rest, activity modification, physical therapy, and bracing often becomes the first approach. In cases where conservative treatment fails or the fracture appears severe, doctors may recommend surgical intervention, such as a spinal fusion or direct repair of the pars defect.
Stress, Structural Forces, and Pars Interarticularis
The pars interarticularis connects the joints above and below one vertebra. Doctors refer to the bony bridge that connects these two upper and lower aspects as the pars interarticularis, which means “part between the articulations” in Latin. An isthmus is a thin strip of land that connects two larger bodies of land, as you may recall from geography. As a result, doctors refer to the pars interarticularis as an “isthmus” since the bone links between the two facet joints.
The pars interarticularis (Latin for “bridge between two joints”) is the portion of the bony arch that connects the facet joint of one level and the facet below. Biomechanically, this is the weakest part of the bony arch, and in some people, a stress fracture can occur through the pars. This pars fracture is called “spondylolysis.”
The bottom two vertebrae of the spine (L4-S1) face down like a sled on a ski slope, and they bear the whole weight of the spine above them. The inferior facets, sometimes known as “door stoppers,” are a buttress that keeps the lower vertebra from slipping down. The bony pars interarticularis connects these “doorstops” to the higher structures (pedicles). As you can expect, these structures do not do well with a great deal of stress, particularly when impact occurs. Contact sports, leaping, and particularly extension can cause overload forces (bending backward). The tiny bony structures (cortical bone and trabecula) that make up the pars interarticularis might become stressed and fractured as a result of this strain.
Three Types of Pars Fractures:
- Atrophic
- Hypertrophic
- Displaced
Atrophic fractures do not mend easily, and this normally occurs because of inadequate immobilization. In this case, the ends of the shattered bone appear very thin, and the body makes a feeble attempt to bring them together. Similarly, a displaced fracture occurs when the vertebra slips forward and the shattered fragment ends do not close and meld to each other. Unfortunately, both heal slowly.
The hypertrophic fracture refers to a thick, expanded, and co-opted fracture end (right next to each other). Furthermore, a brace gives these fractures the best chance of healing.
Unilateral (one-sided) fractures will heal quite well. However, healing without a brace and without limiting activity negatively affects the healing process for a broken pars fracture. Even with the greatest healing fractures (unilateral and hypertrophic), the success rate with a brace and three to six months of limited activity is around 50%. Consequently, children and adults can re-fracture a pars fracture if they resume their old level and kind of activity. Our doctors surgically treat these fractures with an excellent success rate.
Development of Pars Fractures
If the pars repeatedly get overloaded without enough time between episodes to enable healing, they will ultimately break (fracture) and become incompetent, similar to how bending a metal coat hanger causes it to fail. Genetics has a significant impact as well. These fractures usually affect both sides of the pars; however, they can also affect just one side (unilaterally). If only one side of the pars breaks, the opposing pars take the brunt of the stress and may eventually fracture. Because of the absence of protection to prevent shear stresses (slide forces) on discs, fractures can occur on both sides.
The crack may affect only one side, but it is not uncommon to have fractures on both sides of the vertebra. When fractures occur on both sides, one vertebra can translate or move forward or backward over the neighboring vertebra. This is called spondylolisthesis.
The disc acts as a shock absorber and serves as the primary cushion for spinal trauma. However, the disc has a low shear (slide) resistance. The disc is exposed to aberrant stresses that might harm it without the facets in the back protecting it. The unbroken facets prevent these stresses from occurring, and pars fractures can cause the disc to collapse.
When spondylolysis (pars defects) occurs, it creates a change in the biomechanics of the spinal segment. This happens because the connection between the facet joints is broken. As a result, the bone above can begin to gradually slip forward on top of the bone below. This ‘slip’ is known as isthmic spondylolisthesis.
Pars Fractures Progression
As the slip progresses, the disc between the bones is subjected to increased stress, leading to accelerated disc degeneration. Consequently, without the protective role of the facets, the disc becomes more vulnerable to damage, which can result in further spinal issues and pain. By understanding how spondylolysis alters spinal biomechanics, we can better appreciate the importance of early diagnosis and intervention to prevent severe complications.
The disc can stretch and subsequently tear under extreme tension. Consequently, the above-mentioned vertebra then begins to slide forward on the one below. (The L5 vertebra, in particular, can begin to move forward on the sacrum.) An isthmic Spondylolysis (lysis meaning “cut” or “break”) happens before the sliding commences. Doctors refer to the condition as isthmic spondylolysis if there is a slide accompanying it (olio-thesis means to slip in Latin). This fracture appears more common in teenagers who participate in contact sports or whose sport requires them to bend backward (wrestling and gymnastics come to mind).
Children with Pars Fractures
Pars interarticularis fractures affect one out of every twenty children. These fractures usually happen between the ages of 8 and 15. Many times, a child who develops a new fracture will not exhibit any severe symptoms at first or will disregard the discomfort and not inform parents, coaches, or trainers. In many children, the discomfort will subside until the disc gets injured.
In general, children with broken bones heal very quickly. Pars interarticularis fractures, on the other hand, do not heal well. The following three factors provide the reason for poor healing.
- These fractures display a relatively limited surface area.
- When extensive cancellous surface regions become exposed, the bone will heal faster. The “spongy bone” inside the hard cortical bone, cancellous bone, contains many bone-generating cells. Unfortunately, very little cancellous bone exists in the pars interarticularis.
- The spine endures some of the most extreme motion and shear pressures. Extreme pressure will cause a bone to crack. It’s tough to get an energetic youngster or teenager to relax in this location. A brace can help a youngster slow down, but it won’t immobilize the region, and mending bone cells don’t like mobility. The type of pars fracture you sustain will influence your rehabilitation.
What are the Symptoms of Spondylolysis?
Spondylolysis primarily manifests as pain and stiffness in the lower back, often exacerbated by physical activity and alleviated by rest. Overextending the lower back, such as with certain exercises or heavy lifting, can intensify the discomfort due to the stress on the spine’s affected area.
This condition is a stress fracture in a portion of the spine known as the ‘pars,’ often referred to as a ‘pars fracture’ or ‘pars defect.’ This stress fracture can lead to low back pain and may cause the affected bone to slip forward over the bone below it—a scenario called isthmic spondylolisthesis.
How It Leads to Pain and Instability
- Instability: The defect creates instability in the spinal bones, increasing the likelihood of pain.
- Slip Forward: When the bone slips forward, the condition worsens, leading to more pronounced symptoms.
- Disc Degeneration: The instability often results in disc degeneration, which exacerbates back pain.
- Nerve Issues: As the vertebra slips, it can pinch the nerve root behind it, causing radiating leg pain, numbness, or weakness.
Patients with isthmic spondylolisthesis tend to experience more severe back pain due to the compounded effects of bone instability and disc degeneration. Radiating symptoms such as leg pain, numbness, or weakness may also occur, further complicating the condition. Therefore, recognizing the signs early and understanding the underlying mechanisms will enable effective management and treatment.
Common Symptoms Include:
- Lower Back Pain and Stiffness: Persistent, worsens with movement, and improves with rest.
- Nerve-Related Sensations: These can range from a “pins and needles” feeling in one leg to numbness or weakness.
- Pain Distribution: Discomfort isn’t limited to the lower back; you might experience pain radiating to the neck, legs, thighs, or shoulders.
- Muscle Issues: Muscle spasms or generalized weakness can emanate from spondylolysis.
- Tingling and Numbness: These sensations are common in the back but can also affect other areas.
Identifying these symptoms early can facilitate better management and care, ensuring patient avoidance of activities that might exacerbate the condition.
Diagnosis
The diagnosis of pars fractures involves a combination of clinical evaluation, medical history, physical examination, and imaging studies. Doctors follow the following steps:
- Medical History: The healthcare provider will inquire about the patient’s symptoms, including the nature and location of pain, any recent trauma or activities that may have contributed to the injury, and a history of previous spine-related issues.
- Physical Examination: The doctor will perform a thorough physical examination, assessing the patient’s posture, range of motion, and tenderness around the affected area. They may also check for signs of nerve involvement or muscle weakness.
- X-rays: Plain X-rays of the lumbar spine can help identify pars fractures. A lateral view may reveal a “Scottie dog” appearance, with a fracture line visible in the pars interarticularis.
- CT Scan: Computed tomography (CT) scans provide detailed images of the spine and can confirm the presence and severity of a pars fracture. It helps assess bony integrity and identify any associated abnormalities.
- MRI Scan: Magnetic resonance imaging (MRI) scans provide doctors with images of the surrounding soft tissues and assess for any nerve compression or disc involvement.
Goals of Each Phase of Treatment for Spondylolysis and Isthmic Spondylolisthesis
1: Immediate Pain Relief and Inflammation Reduction
- Pain Management: Utilize medications such as NSAIDs and muscle relaxants to alleviate discomfort.
- Inflammation Control: Apply ice packs and encourage rest to minimize swelling and irritation.
- Activity Modification: Advise avoiding activities that exacerbate symptoms, focusing on low-impact exercises instead.
2: Restoring Function and Flexibility
- Physical Therapy: Engage in targeted exercises to enhance the strength and flexibility of the core and back muscles.
- Stretching Routines: Implement stretches that increase the range of motion and prevent stiffness.
- Manual Therapy: Incorporate chiropractic adjustments or massage therapy to improve spinal alignment and mobility.
3: Strengthening and Stabilization
- Strength Training: Focus on building up the muscles that support the spine, particularly the abdominal and lumbar regions.
- Postural Training: Educate on maintaining proper posture during daily activities to avoid undue strain.
- Core Development: Emphasize exercises that reinforce core stability, such as planks and pelvic tilts.
4: Gradual Return to Normal Activity
- Activity Resumption: Gradually reintroduce normal activities and sports, monitoring for any return of symptoms.
- Continued Support: Provide guidance on long-term strategies to prevent recurrence, including ongoing exercise routines and ergonomic adjustments.
- Follow-Up Care: Schedule regular check-ups to assess progress and make any necessary adjustments to the treatment plan.
By following these phased goals, individuals with spondylolysis and isthmic spondylolisthesis can work towards pain relief, improved function, and a sustainable return to their daily activities.
Treatment
The treatment of pars fractures depends on several factors, including the severity of the fracture, symptoms experienced by the patient, and their overall health.
Conservative Treatment:
- Rest and Activity Modification: Avoiding activities that exacerbate pain and stress on the spine, such as high-impact sports or heavy lifting, allows the fracture to heal.
- Physical Therapy: Specific exercises and stretching routines can help strengthen the surrounding muscles, improve flexibility, and provide stability to the affected area.
- Bracing: In some cases, doctors may recommend a brace to limit movement and provide support to the spine during the healing process.
- Nonsteroidal Anti-inflammatory Drugs (NSAIDs): These medications can help reduce pain and inflammation associated with pars fractures.
Surgical Treatment
If surgical treatment is necessary, the recovery timeline will depend on the particular spine surgery performed. Post-surgery, patients will still likely engage in physical therapy to support their recovery and ensure optimal outcomes.
By understanding the different factors that influence recovery time, patients can set realistic expectations and work closely with their healthcare providers to achieve the best possible results.
Steroid spinal injections may aid in more severe cases of discomfort. They may relieve symptoms of spondylolysis, but will not repair the bone fracture. This means that while patients might experience a reduction in pain and improved mobility, the underlying condition remains unhealed. Patients may need surgery if nonsurgical therapy does not relieve their symptoms. However, it’s important to understand that injections are a temporary solution, focusing on symptom management rather than a permanent fix.
Two surgical procedures for a pars deficiency involve Pars repair and lumbar fusion. The challenge with treating this disease in teenagers occurs because teenagers rarely express their grief, and the disorder does not have many symptoms. In addition, this condition may get overlooked by pediatricians, but athletic trainers will spot problems and seek referral sources. Treatment becomes more challenging if the condition continues month after month.
- In cases where conservative treatment fails to provide relief or if the fracture appears severe, doctors will consider surgery.
- When symptoms of spondylolysis persist despite physical therapy and activity modification, doctors may recommend surgical intervention.
- Surgery is typically considered when there is persistent back pain or when one or more vertebrae slip out of place (spondylolisthesis).
- In some cases, nerve pinching associated with spondylolysis might also warrant surgery.
Surgical options include:
- Direct Pars Repair: The surgeon directly repairs the fractured pars interarticularis using screws, wires, or bone grafts to promote healing and stability.
- Spinal Fusion: In more complex cases or when instability becomes an issue, doctors will perform a spinal fusion to join two or more vertebrae together, providing long-term stability.
When it comes to spinal fusion for treating spondylolysis and spondylolisthesis, doctors may consider several specific procedures:
- Laminectomy and Posterior Fusion: This procedure involves removing a portion of the vertebra to relieve pressure on the spinal nerves, followed by fusion of the affected vertebrae to stabilize the spine.
- Anterior Lumbar Interbody Fusion (ALIF): In this technique, the surgeon approaches the spine from the front (anterior) and removes the damaged disc, replacing it with a bone graft or implant to fuse the vertebrae.
- Minimally-Invasive Lumbar Fusion (MIS TLIF): This is a less invasive approach where the surgeon accesses the spine through smaller incisions, reducing recovery time and minimizing tissue damage.
Additionally, if there is pinching of a nerve, a laminectomy (spinal decompression surgery) may also relieve pressure on the nerve.
By understanding the variety of surgical options available, patients can make more informed decisions in consultation with their healthcare providers. Each procedure has its benefits and considerations, tailored to the individual’s specific condition and overall health.
Understanding the Recovery Time for Spondylolysis
The recovery time for spondylolysis largely depends on the treatment approach taken and the individual’s severity of the condition.
Nonsurgical Treatment
For nonsurgical treatments, recovery can range from a couple of weeks to several months. Bracing is often recommended and can last for three to four months while the fracture heals. During this time, physical therapy is typically included to help maintain and strengthen the abdominal and back muscles through specific exercises.
- Mild to Moderate Cases: Recovery from nonsurgical methods can range from a few weeks to several months. Factors such as the patient’s overall health and responsiveness to treatment influence this timeframe.
- Treatment Inclusions: Typically, this might involve activity restriction, bracing, and physical therapy. Doctors may recommend bracing for around three to four months to ensure proper healing.
Surgery
Working these core muscles allows patients to move more easily and reduces the likelihood of future discomfort and issues. Patients should anticipate being in therapy sessions for 6-8 weeks and a full recovery to take up to 6 months. However, the recovery period for spondylolysis can vary widely based on the severity of the condition and the type of treatment received.
- Severity-Based Recovery: If surgery is required, the recovery period will vary based on the specific procedure performed.
- Post-Surgery Care: Patients can expect a combination of bracing and a structured physical therapy program to help rebuild muscle strength and enhance flexibility in the abdomen and back.
Overall, spondylolysis recovery can be integrated as a multi-dimensional process that requires adherence to medical advice. Of course, consistent therapy efforts will assist in a successful return to normal activities.
Post-Treatment Rehabilitation
Rehabilitation plays a crucial role in the recovery process after treatment for pars fractures. The following aspects are typically addressed:
- Strengthening Exercises: Targeted exercises to improve core strength, stability, and flexibility of the spine and surrounding muscles.
- Posture and Body Mechanics: Educate the patient about proper body mechanics, ergonomics, and techniques to prevent future injuries or stress on the spine.
- Gradual Return to Activities: Guided progression back to normal activities, ensuring proper technique and monitoring for any recurrence of symptoms.
- Lifestyle Modifications: Encouraging healthy lifestyle choices, including weight management and regular exercise, to support overall spine health and prevent future injuries.
- Activity Modification: Providing guidance on modifying activities and avoiding high-impact or repetitive motions that may put excessive stress on the spine.
- Pain Management: Our doctors educate patients about pain management techniques. This includes the appropriate use of medications, hot/cold therapy, and self-care to alleviate discomfort during the healing process.
Follow-Up and Monitoring: Regular follow-up appointments with healthcare providers are essential to monitor the healing progress, evaluate treatment efficacy, and address any concerns or complications. Imaging studies will continue periodically to assess fracture healing and overall spine health.
Getting the Best Care for Spine Fractures
Potential patients with pars fractures should consider seeking care at the Southwest Scoliosis and Spine Institute for several reasons. Firstly, Doctors Richard Hostin, MD, Devesh Ramnath, MD, Ishaq Syed, MD, Shyam Kishan, MD, and Kathryn Wiesman, MD, specialize in all types of spine conditions, deformities, and scoliosis pain, and the institute is renowned for its expertise in treating spinal conditions, including pars fractures.
Secondly, the Southwest Scoliosis and Spine Institute with offices in Dallas, Plano, and Frisco, Texas. Provides a comprehensive and patient-centered approach to care. They understand the unique challenges and complexities associated with pars fractures and tailor treatment plans to meet individual needs. Whether it’s conservative management with physical therapy and bracing or surgical intervention, patients can trust that the institute will provide the most appropriate and evidence-based treatment options.
Lastly, the institute prioritizes patient education and involvement throughout the treatment process. They take the time to explain the diagnosis, discuss treatment options, and answer any questions or concerns. Our doctors empower our patients with knowledge about their condition. This enables them to make informed decisions about their care. With a focus on compassionate and personalized care, the Southwest Scoliosis and Spine Institute ensures that patients with pars fractures receive exceptional care and support on their journey to recovery.
Citation: National Institute of Health – Treatment of Pars Fracture
The medical content on this page has been carefully reviewed and approved for accuracy by the Southwest Scoliosis and Spine Institute’s qualified healthcare professionals, including our board-certified physicians and Physician Assistants. Our team ensures that all information reflects the latest evidence-based practices and meets rigorous standards of medical accuracy, with oversight from our expert spine doctors to guarantee reliability for our patients.


