SCHWANNOMA TUMORS
A schwannoma is a tumor that grows from the Schwann cells in the peripheral nervous system or nerve roots. The majority of schwannomas are benign; however, occasionally they might become malignant.
At the Southwest Scoliosis and Spine Institute, our expert Schwannoma Tumor Doctors and Surgeons are dedicated to diagnosing and treating spinal problems in children and adults to ensure comprehensive care tailored to each patient’s needs. With advanced techniques and a compassionate approach, our team diagnoses, treats, and cares for patients suffering from Schwannoma Tumors.
3 percent of individuals with progressive curvature may eventually experience severe problems that can include scoliosis and back pain, spinal problems, and nerve compression causing numbness, weakness, and leg pain.
Schwannoma Tumors
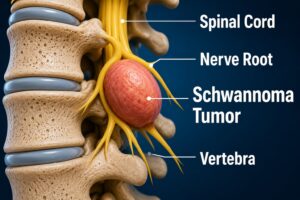 A schwannoma forms a tumor from Schwann cells in your peripheral nervous system or nerve roots. Most schwannomas stay benign (noncancerous), but some turn malignant (cancerous). Schwann cells aid nerve impulse transmission. They encircle peripheral nerves to offer support and protection. Your peripheral nerves send and receive messages from your spinal cord and brain to the body.
A schwannoma forms a tumor from Schwann cells in your peripheral nervous system or nerve roots. Most schwannomas stay benign (noncancerous), but some turn malignant (cancerous). Schwann cells aid nerve impulse transmission. They encircle peripheral nerves to offer support and protection. Your peripheral nerves send and receive messages from your spinal cord and brain to the body.
Cancerous schwannomas often harm the sciatic nerve in your leg, the brachial plexus in your arm, and the sacral plexus. This nerve bundle affects your lower back. Your intestines or bladder may hurt or feel uneasy at this stage.
Who do Schwannomas Tumors Affect?
Schwannoma tumors strike people aged 50 to 60 most often. They rarely hit children. Healthy individuals develop schwannomas sporadically. Hereditary disorders like neurofibromatosis 2 (NF2), schwannomatosis, or Carney complex trigger schwannomas. Schwannomas affect fewer than 200,000 people yearly in the U.S.
Types of Schwannomas
Vestibular schwannomas, or acoustic neuromas, make up about 60% of benign schwannomas. Spinal schwannomas rank as another common type. These benign nerve sheath tumors grow within the spinal canal, often from spinal nerve roots. Spinal schwannomas top the list of spine nerve sheath tumors. They form 15–50% of intradural extramedullary spinal tumors.
Vestibular and spinal schwannomas share traits, but location and involved nerves vary symptoms and treatment. Schwannomas appear most often in cervical (neck) and lumbar (lower back) spine regions. They develop along nerve roots in these busy zones. This can cause pain, numbness, or muscle weakness.
Questions and Answers
How serious is a Schwannoma Tumor?
Doctors consider Schwannoma tumors as benign tumors that arise from Schwann cells, which support and insulate nerve fibers. While schwannomas are typically non-cancerous and slow-growing, their impact and seriousness can vary depending on their location, size, and proximity to vital structures. In some cases, schwannomas may cause symptoms or affect nerve function, leading to pain, weakness, or sensory disturbances. Patients with a Schwannoma tumor on their spine should seek the very best spine specialists like those at the Southwest Scoliosis and Spine Institute.
What is the life expectancy of a person with a Schwannoma Tumor?
Schwannomas, by themselves, do not significantly affect life expectancy. Since they are usually benign and slow-growing tumors, they generally do not pose a direct threat to a person’s life. However, life expectancy can be influenced by factors such as the location of the schwannoma and its potential impact on surrounding structures or organs. If a schwannoma causes complications or requires surgical intervention, the prognosis and recovery will depend on several factors, including the individual’s overall health, the extent of the tumor, and the success of the treatment.
Should a surgeon remove a Schwannoma Tumor?
The decision to remove a schwannoma depends on various factors, including its location, size, symptoms, rate of growth, and potential risks or complications. In some cases, small schwannomas that are not causing any symptoms or affecting nerve function may be monitored over time through regular imaging tests. However, if a schwannoma is causing significant symptoms, growing rapidly, or threatening nearby structures or nerves, surgical removal may be recommended. The aim of surgery is to alleviate symptoms, prevent further complications, and ensure the best possible outcome for the patient. The necessity of removal will be determined on an individual basis by a medical professional specializing in the management of schwannomas.
Important Topics to Review Alongside Spinal Schwannomas?
Explore related conditions and tumor types to understand spinal schwannomas better. Key areas include:
- Other spinal canal tumors, like meningiomas or ependymomas, share symptoms or imaging traits.
- Intradural extramedullary tumors, including schwannomas, are found within the dura but outside the spinal cord.
- Spinal nerve sheath tumors, covering schwannomas, neurofibromas, and malignant types, to recognize as nerve-related tumors.
Reviewing these topics clarifies how schwannomas compare to other diagnoses. It highlights the need for expert evaluation.
What are the Typical Symptoms of Schwannoma Tumors?
Schwannomas often hide symptoms until they grow large enough to press nerves. The affected nerve region may cause discomfort. Common symptoms include:
- A visible bump under the skin.
- Piercing, throbbing, or searing pain.
- Tingling or pins-and-needles sensation.
- Muscle tremor.
- Numbness.
- Nighttime neck or back pain.
Symptoms vary by location, affecting the face, arms, legs, or torso. As the tumor grows, symptoms may change. Spinal schwannomas stay silent until large. Pressure on nearby nerves or the spinal cord triggers:
- Pain, numbness, or weakness in limbs.
- Balance issues.
- Poor coordination, especially in the hands.
- Back or neck pain waking you at night.
Vestibular schwannomas, or acoustic neuromas, grow on the nerve linking your inner ear to your brain. These add symptoms like:
- Ringing in one or both ears.
- Balance and coordination loss.
Knowing specific symptoms aids early detection and management. Prompt action with healthcare pros matters.
What Causes a Schwannoma?
Schwannoma remains unknown in most cases. About 90% occur sporadically. Inherited disorders like Carney complex, neurofibromatosis 2 (NF2), and schwannomatosis lead to schwannomas. Genetic studies show the NF2 gene on chromosome 22 drives schwannoma development. Parents pass this tendency to kids, who may pass it on.
Risk Factors of Schwannoma Tumors
Schwannomas lack clear risk factors:
- Tumors can hit any age or gender.
- Women may develop schwannomas more often with neurofibromatosis 2.
- Parents passing schwannomas to kids remains a factor. Genetic risks still need study.
Genetic Influences and Sporadic Cases
Schwannomas are tied to inherited conditions like neurofibromatosis II (NF2) and schwannomatosis. These genetic disorders raise schwannoma risk, including spinal ones.
- Neurofibromatosis II (NF2): Causes multiple schwannomas, often affecting cranial and spinal nerves.
- Schwannomatosis: A rarer condition linked to these tumors.
Without NF2 or schwannomatosis, schwannomas turn “sporadic.” They arise without clear risks. These common nerve sheath tumors typically form alone. One tumor rarely leads to another.
Recurrence Risk: NF2 vs. Sporadic Schwannomas
While schwannomas are typically slow-growing and rarely become cancerous, the risk of developing additional tumors varies depending on the underlying cause. For most people with sporadic, single schwannomas, removal of the tumor is usually curative, and the chances of the tumor coming back in the same spot are very low.
However, in individuals with neurofibromatosis II (NF2), the outlook is somewhat different. Because NF2 is an inherited disorder affecting tumor-suppressing genes, these patients have a much higher likelihood of developing new schwannomas over time. Even after successful surgical removal, new tumors can appear elsewhere along the nervous system, making long-term monitoring essential for those living with NF2.
Understanding the difference in recurrence risk helps patients and their healthcare providers plan for ongoing care and follow-up, especially for those with known genetic predispositions.
Demographic Considerations
- Gender and Age: Both men and women are equally susceptible, with most cases occurring in middle-aged individuals. However, schwannomas can also present in children and older adults, albeit less frequently.
Understanding these factors provides a clearer picture of the risk landscape for schwannoma tumors, aiding in earlier recognition and treatment.
Diagnosis of Schwannoma Tumors
Schwannoma symptoms mimic other illnesses, making diagnosis tough. Their slow growth keeps the symptoms faint. Your doctor asks about signs, reviews your medical history, and performs a physical exam. A neurological assessment checks for schwannomas. If symptoms suggest a nerve tumor, your doctor may offer:
- MRI scans for detailed nerve images.
- CT scans for tumor growth assessment.
- An electromyogram (EMG) is used to record muscle activity.
- Nerve conduction tests to measure signal speed.
- Tumor biopsy to examine cells.
- Nerve biopsy for conditions like neuropathy.
These tools pinpoint spinal schwannomas for informed treatment.
Magnetic Resonance Imaging (MRI)
MRI creates a detailed 3-D image of your nerves and tissue. It uses magnets and radio waves. MRI excels at spotting spinal schwannomas as small as a few millimeters. A contrast agent, given intravenously, brightens schwannomas on scans. This separates them from tumors like meningiomas or ependymomas.
Differential Diagnosis
Spinal tumors may look similar on imaging. Key conditions to consider include:
- Neurofibroma
- Meningioma
- Paraganglioma
- Myxopapillary ependymoma
- Intradural extramedullary metastases
Each shows unique MRI traits like location or enhancement. Careful analysis ensures the right diagnosis for proper treatment.
Melanotic Schwannomas: Unique MRI Features
Unlike typical schwannomas, melanotic schwannomas appear distinctly on MRI scans. These tumors often show up as bright (hyperintense) on T1-weighted images and dark (hypointense) on T2-weighted images—essentially the reverse of what is expected with most schwannomas. Recognizing this unusual imaging pattern helps radiologists and healthcare professionals distinguish melanotic schwannomas from other nerve sheath tumors and spinal lesions.
Computerized Tomography (CT)
To take many pictures of your body, a CT scanner revolves around it. For your doctor to assess how your tumor’s growth could harm you, a computer utilizes the photos to create a comprehensive depiction of it.
Electromyogram (EMG)
In this test, a doctor inserts a small needle into a muscle so that an electromyograph records the muscle’s electrical activity when it tries to move it. Examination of nerve conduction. You may have this test taken with your EMG. It measures how quickly nerves transmit electrical signals to muscles.
Tumor Biopsy
If imaging tests reveal a nerve tumor, your doctor may take a tiny sample of cells (biopsy) from the tumor and examine them. You could require either local or general anesthesia for the biopsy, depending on the size and location of the tumor.
Nerve Biopsy
Your doctor could do a nerve biopsy if you have a disease like increasing peripheral neuropathy or swollen nerves that resemble nerve tumors. Depending on the magnitude of the tumor development, the course of therapy will start once the diagnosis has been made.
By leveraging these diagnostic tools, particularly the detailed imaging offered by MRIs, healthcare providers can effectively pinpoint the presence and specifics of spinal schwannomas, leading to informed decisions about treatment.
Radiographic Features of Spinal Schwannomas
Spinal schwannomas have some distinct features on imaging studies that set them apart from other nerve sheath tumors and aid in accurate diagnosis. While often difficult to distinguish from neurofibromas based solely on appearance, certain radiographic characteristics help identify spinal schwannomas.
- Location and Shape:
Most spinal schwannomas are found within the dura but outside the spinal cord itself (intradural extramedullary), with the majority occurring in the cervical and lumbar regions. These tumors tend to be well-circumscribed and rounded, sometimes causing nearby bone to remodel due to slow, persistent growth. Larger schwannomas may extend along the length of the spinal cord, forming elongated, sausage-like masses that can span several vertebral levels. In other cases, they extend outward through the neural foramina, taking on a characteristic “dumbbell” shape.
- MRI Findings:
Magnetic resonance imaging is particularly valuable in characterizing spinal schwannomas:
- On T1-weighted images, Most schwannomas appear the same color (isointense) as spinal cord tissue, while a smaller proportion looks darker (hypointense).
- On T2-weighted images, the overwhelming majority appear brighter than surrounding tissue (hyperintense), often featuring areas with mixed signals.
- After contrast injection (T1 with contrast): Schwannomas show robust and almost universal enhancement, making them stand out clearly against adjacent structures.
It’s worth noting that some schwannomas display unique internal changes, such as bleeding, cyst formation, or fatty transformation—features less commonly seen in neurofibromas.
- Special Type – Melanotic Schwannomas:
Though rare, melanotic schwannomas may defy typical patterns and will instead appear brighter than normal tissue on T1-weighted images and darker on T2-weighted scans. Together, these imaging features—especially when combined with clinical context—play a critical role in the assessment, classification, and management planning for patients with suspected spinal schwannomas.
Classification of Spinal Schwannomas
Spinal schwannomas, a type of tumor affecting the protective membrane around nerves, are categorized primarily based on three factors: size, location, and their relationship with the dura. The dura is a delicate membrane that encloses essential components, including the spinal cord and parts of the spinal nerves.
Type I
These tumors lie entirely within the dura. This is the most common type of spinal schwannoma, remaining enclosed without extending beyond the membrane’s confines.
Type II
Initially arising within the dura, these tumors grow along a spinal nerve’s path and exit the spinal canal through the neural foramen—a channel allowing nerves to pass from the spine to the body. Due to their configuration, they feature a component inside and another outside the canal, forming what’s known as a dumbbell shape.
Type III
These are located entirely outside the spinal canal and are often referred to as paraspinal nerve sheath tumors. They do not breach the dura at any point.
Type IV
Originating outside the spinal canal, these tumors develop similarly to Type III but eventually infiltrate the spinal canal through the foramen. Like Type II, they take on a dumbbell shape, with sections inside and outside the spinal canal.
Understanding these classifications helps in assessing the nature and potential treatment approaches for schwannomas. Each type presents distinct challenges based on its position and growth pattern, directly influencing surgical and therapeutic strategies.
Treatment
To search for any indicators of Schwannoma, the oncologist, a cancer expert, will ask about the patient’s whole medical history and evaluate all outward skin irritation. Treatment for schwannomas is based on the location of the abnormal growth, as well as whether it hurts or is enlarging rapidly. Options for treatment include:
- Your doctor might advise keeping an eye on your condition over time. Regular checks and an MRI or CT scan every few months to monitor the tumor’s growth will greatly help the doctor understand the patient’s condition.
- Because these are benign, slow-growing lesions, they are indicated for patients over the age of 70 with very small lesions and severe systemic or asymptomatic disease.
Surgery
If the tumor is hurting or expanding rapidly, a skilled peripheral nerve surgeon can remove it. Under general anesthesia, surgery on schwannomas is performed. Some patients can leave the hospital the day after surgery, depending on the location of the tumor. Some individuals may require a one- or two-day hospital stay. A tumor can come back even after it has been successfully removed after surgery. Surgery may often remove schwannomas with minimal possibility of them coming back until they are big enough to obstruct nerves or surrounding structures or to disfigure a person. Schwannomas tend to stay rather small; therefore, standard surgery may completely remove the tumor.
The surgeon exposes the nerve, isolates the schwannoma from the healthy nerve tissue using precise microsurgical methods, and then eliminates it. It is crucial to seek the advice of a skilled surgeon like those at the Southwest Scoliosis and Spine Institute with experience in treating nerve tumors, since some schwannoma surgical operations may need nerve restoration if the tumor’s removal will damage a nerve.
The nerve function may improve quickly following successful surgery for treatments on peripheral nerve schwannomas, but if the schwannoma damages muscles, they could take longer to mend. Muscle dysfunction or weakness can occasionally last a lifetime. After surgery to remove a vestibular schwannoma, symptoms including facial paralysis, hearing loss, and headaches may last for weeks or even months before getting better.
Surgical Techniques for Removing Spinal Schwannomas
When it comes to the removal of spinal schwannomas, the approach largely depends on various factors such as the tumor’s size, location, and the symptoms presented by the patient.
Observation vs. Surgery
- Observation: If a spinal schwannoma is small, asymptomatic, and not exerting pressure on surrounding tissues, doctors can monitor it through regular monitoring with MRI scans.
- Surgery: For larger tumors, causing symptoms, or showing growth, surgical intervention is often necessary.
Microsurgical Techniques
The most effective approach for removing spinal schwannomas involves microsurgical techniques. These techniques allow for the precise removal of tumors:
- Surgical Microscopes: Surgeons employ high-powered microscopes to gain a clear and magnified view of the tumor and surrounding nerves, which facilitates meticulous dissection and removal.
- Fine Instruments: The use of very fine, specialized instruments ensures accuracy and minimizes damage to the surrounding healthy tissue.
- Microsurgical Techniques: An array of microsurgical techniques is utilized to carefully separate and excise the tumor from nerve fibers or spinal structures.
These advanced techniques not only aim to completely remove the tumor but also prioritize preserving neurological function. Many patients experience improvements in their symptoms post-surgery, highlighting the effectiveness of these methods.
Radiation therapy
Radiation therapy is used to control tumor growth and improve symptoms. Along with surgery, radiation often will help the patient. Stereotactic radiosurgery (SRS) uses many precisely focused beams to destroy a tumor. If the tumor is near vital blood vessels or nerves, the doctor may recommend radiation therapy instead of surgery to avoid potential complications.
Stereotactic radiosurgery
A method known as stereotactic body radiation treatment may reduce harm to healthy tissue if the tumor appears close to important nerves or blood arteries. With this method, medical professionals may accurately apply radiation to a tumor without cutting the skin. Therefore, only microsurgery, which works for medium and large-sized tumors, can result in a full cure. A 12 to 24-hour stay in an intensive care unit is necessary after the treatment, along with continuous neurophysiological monitoring. It is possible to mix radiosurgery with microsurgery.
What is the Outlook for Schwannoma Tumors?
The prognosis for schwannoma relies on several variables, including:
- The location of the tumor.
- The tumor’s size.
- How much of the tumor was removed during surgery, if any?
- A benign or cancerous tumor.
The outlook for schwannoma is often favorable. When a tumor is eliminated, it often doesn’t return (recur). In most patients, doctors can completely remove these tumors using a surgical microscope, very fine instruments, and an array of microsurgical techniques. This precise approach not only ensures the safe removal of the tumor but also significantly contributes to the improvement in neurological function that many patients experience post-surgery.
However, the majority of schwannoma problems usually develop following tumor removal surgery. The following situations considerably increase the likelihood of postoperative complications:
- If the tumor is significant.
- When the tumor is deep in the interior of the body.
- If your ulnar nerve is the site of the tumor (one of the three main nerves in your arm).
Despite these potential challenges, the advanced surgical techniques employed tend to minimize risks and enhance recovery, offering a hopeful prognosis for those undergoing treatment.
What Possible Side Effects Might Schwannoma Tumors Cause?
Finally, by sticking to the treatment plan that you and your healthcare provider specifically created for you, you can reduce your chance of experiencing major consequences. Schwannoma complications include:
- Adverse consequences of schwannoma treatment
- Loss of function, most often hearing loss, in the afflicted area
- In the afflicted region, numbness
- The afflicted region is in pain.
- In the afflicted region, paralysis
- Cancer returning
While recurrence is rare, it remains a possibility, particularly if the tumor was not completely removed. The slow growth of these tumors means symptoms can develop gradually over time, potentially impacting quality of life before diagnosis or intervention. As with any condition affecting nerves, early detection and a tailored treatment plan are essential to minimize lasting effects.
When a Patient is Diagnosed With a Schwannoma Tumor on their Spine, Who Should They See?
At the Southwest Scoliosis and Spine Institute, we focus on Scoliosis Diagnosis, Treatment, & Care for our Patients. Our fellowship-trained, board-certified expert orthopedic scoliosis surgeons, Richard Hostin, MD, Devesh Ramnath, MD, Ishaq Syed, MD, Shyam Kishan, MD, and Kathryn Wiesman. If a patient has been diagnosed with a schwannoma tumor on their spine, seeking care at the Southwest Scoliosis and Spine Institute, with offices in Dallas, Plano, and Frisco, Texas, can offer several benefits. Here are a few reasons why:
Expertise in Spine Conditions
The Southwest Scoliosis and Spine Institute specializes in treating various spine conditions, including schwannomas. They have a team of experienced spine specialists who are well-versed in diagnosing and treating these tumors. Their expertise ensures patients receive accurate evaluations, tailored treatment plans, and optimal care for their conditions.
Comprehensive Treatment Options
The institute offers a wide range of treatment options for schwannomas, including both non-surgical and surgical approaches. They can assess the tumor’s characteristics and location to determine the most suitable treatment strategy. This may involve monitoring the tumor’s growth, utilizing targeted therapies, or considering surgical removal when necessary.
Individualized Care and Support
The Southwest Scoliosis and Spine Institute prioritizes personalized care for each patient. They understand that schwannomas can have varying impacts and complexities, and they take the time to listen to patients’ concerns and provide compassionate support throughout the treatment journey. Their multidisciplinary team works together to address all aspects of the condition, from diagnosis to rehabilitation, ensuring the best possible outcome for the patient.
Collaboration and Advanced Technology
The institute emphasizes collaboration among specialists and utilizes advanced technology and diagnostic tools to provide precise evaluations and treatment planning. This enables them to offer the most effective and innovative treatment options available for schwannoma tumors.
Focus on Quality of Life
The Southwest Scoliosis and Spine Institute recognizes the importance of preserving and improving patients’ quality of life. They aim to alleviate symptoms, minimize the impact of the tumor on spinal function, and restore mobility and overall well-being. Their holistic approach takes into account the physical, emotional, and functional aspects of the patient’s condition, aiming for the best possible long-term outcomes.
It is important to consult with the Southwest Scoliosis and Spine Institute or a trusted healthcare professional for a thorough evaluation and to discuss personalized treatment options based on the specific characteristics of the schwannoma tumor and the individual patient’s needs. To get an appointment within 24 hours. Call us.
Citations: WebMD – Neurofibrosarcoma and Schwannoma
The medical content on this page has been carefully reviewed and approved for accuracy by the Southwest Scoliosis and Spine Institute’s qualified healthcare professionals, including our board-certified physicians and Physician Assistants. Our team ensures that all information reflects the latest evidence-based practices and meets rigorous standards of medical accuracy, with oversight from our expert spine doctors to guarantee reliability for our patients.
We’re here to help STOP THE PAIN
If you are an adult living with scoliosis or have a child with this condition and need a doctor who specializes in orthopedic surgery,
call the Southwest Scoliosis and Spine Institute at 214-556-0555 to make an appointment today.


