Flatback Syndrome
 Judy Dorsett was diagnosed with scoliosis at age 16 and underwent multiple fusion surgeries to correct her double curve. Watch her video. click here.
Judy Dorsett was diagnosed with scoliosis at age 16 and underwent multiple fusion surgeries to correct her double curve. Watch her video. click here.
For many years, Judy was fine. However, as she grew older, she began to experience pain in her back, legs, and hips. In addition, she found that she could no longer stand up straight, limiting her ability to get around easily.
Dr. Richard Hostin diagnosed Judy with a condition known as Flatback Syndrome. He recommended revision surgery to correct the problem. Consequently, the very first day after surgery, she stood up… and she stood up straight. Then two weeks later she came back to follow up with Dr. Hostin, and she was pain-free!
What is Flatback Syndrome?
Flatback syndrome refers to a condition whereby the lower spine loses some of its natural curvatures. It causes a form of sagittal imbalance in the spine. Your back has several natural spinal curvatures that help balance the weight of your body, walk normally, and stand upright. These curves help in carrying the weight of the trunk, arms, and neck. The spine curves a little bit backward where it joins the pelvis. This curve is known as lordosis. Also, the spine curves slightly forward where it joins the ribs at the chest level. This curve is known as kyphosis.
Furthermore, these curves give the spine its characteristic “S” shape. Flatback posture occurs when a person loses the natural curve in their lower back, causing the spine to become straight. When your back loses its curves, this can lead to several symptoms. Some symptoms are pain, inability to stand upright, or having to take breaks when walking. Moreover, these symptoms lead doctors to diagnose flatback Syndrome.
The flatback syndrome occurs when there is no lordosis or kyphosis or both, thereby straightening the spine. Lordosis occurs naturally in two places in our spine. These include the lumbar section (lower back) and the cervical or neck section of the spine. Kyphosis is a severe rounding of the back. Patients with flatback syndrome usually appear stooped forward and may find it difficult to stand up straight.
Biomechanical Implications on the Heart and Spine
When straight-back syndrome is severe and/or left untreated, a variety of clinical cardiovascular manifestations can develop as the distance between the heart and the spine biomechanically decreases. This compression can affect the spine, the heart, and other important organs. Specific conditions that may arise include:
- Cardiac disease
- Valvular heart disease
- Atrial septal defect
- Cardiac murmurs
- Pseudo heart disease
These conditions underscore the critical nature of maintaining proper spinal curvature not only for skeletal health but also for the optimal functioning of major organs like the heart. The biomechanical changes in patients with straight back or flatback syndrome can have profound effects beyond simple discomfort or pain, leading to significant clinical implications that require timely medical attention.
Understanding and addressing these changes early can prevent the development of more severe complications, highlighting the importance of recognizing symptoms and seeking appropriate care for spinal disorders.
Your back has several natural spinal curvatures that help balance the weight of your body, walk normally, and stand upright. These curves help in carrying the weight of the trunk, arms, and neck. The spine curves a little bit backward where it joins the pelvis. This curve is known as lordosis. Also, the spine curves slightly forward where it joins the ribs at the chest level. This curve is known as kyphosis.
Flatback Posture
Furthermore, these curves give the spine its characteristic “S” shape. Flatback posture occurs when a person loses the natural curve in their lower back, and the spine becomes straight. When your back loses its curves, this can lead to several symptoms. Some symptoms are pain, inability to stand upright, or having to take breaks when walking. Moreover, these symptoms lead doctors to diagnose flatback Syndrome.
The flatback syndrome occurs when there is no lordosis or kyphosis or both, thereby straightening the spine. Lordosis occurs naturally in two places in our spine. These include the lumbar section (lower back) and the cervical or neck section of the spine. Kyphosis is a severe rounding of the back. Kyphosis Patients with the flatback syndrome usually appear stooped forward and may find it difficult to stand up straight.
How Do You Know If You Have Flatback Syndrome?
Those with flatback syndrome may not know that they have the condition since the spine has been gradually changing with time, or sometimes caused by incorrect surgery. Sometimes, patients can end up with flatback after surgery because the usual curves the spine needs are no longer present.
Patients with flatback syndrome lose lordosis in their spine. As a result, their body will adapt by tilting the pelvis and flexing the hips and knees, thereby allowing the patient to stand upright.
However, this adaptation comes with significant consequences. The body overcompensates for the spinal abnormality, leading to excess fatigue and difficulty maintaining proper posture. Many patients find that their symptoms worsen as they go about their day because these compensatory changes wear the body down. The muscles in the pelvis, hips, and knees exhaust their resources, causing substantial fatigue.
Patients with flatback syndrome usually visit spine centers due to symptoms such as back or leg pain and difficulties with carrying out daily activities. They may also experience poor posture that deteriorates over time, often resulting in the need for a cane or walking stick for support.
Key Symptoms and Consequences:
- Back or Leg Pain: Directly linked to the body’s attempt to correct posture.
- Fatigue: Particularly in muscles compensating for spinal imbalance.
- Worsening Posture: As the day progresses, compensatory mechanisms lead to increased muscle exhaustion.
These symptoms typically intensify as the day progresses, underscoring the toll that flatback syndrome takes on the body. Effective management and timely medical intervention are crucial to alleviating these issues and improving the quality of life.
In some cases, the patients may also have spinal stenosis (i.e., A narrowing around the spinal canal that causes nerve symptoms).
The chronic pain and stooped posture associated with Flatback Syndrome also mean that many patients require a cane or walker. These patients may develop pain in their neck and upper back as they strain to try and keep their eyes facing forward. In some cases, patients also experience symptoms of adult scoliosis, sciatica, or spinal stenosis. This causes pain and weakness in the legs that can get worse when walking.
In some cases, patients also experience symptoms of adult scoliosis, sciatica, or spinal stenosis. This causes pain and weakness in the legs that can get worse when walking. Furthermore, some patients report a degree of chronic pain in the cervical spine and upper back area, which can be debilitating over time. These symptoms may handicap the patient, leading them to require prescription pain medications as well as limiting their daily routine.
We’re here to help STOP THE PAIN
Call 214-556-0555 or Email Us to make an appointment with our expert flatback doctors.
What Causes This Ailment or Syndrome?
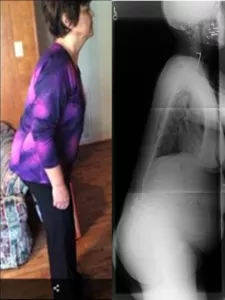 One of the more common reasons we see patients come in with flat back posture is a history of spinal fusion surgeries. Especially those fusions that used earlier surgical techniques and instrumentation. While most patients do well for decades after surgery, some patients lose their natural spine curves. Early fusion techniques could cause the discs below the fused section to quickly degenerate. When this happens, it could cause loss of natural spine curvature.
One of the more common reasons we see patients come in with flat back posture is a history of spinal fusion surgeries. Especially those fusions that used earlier surgical techniques and instrumentation. While most patients do well for decades after surgery, some patients lose their natural spine curves. Early fusion techniques could cause the discs below the fused section to quickly degenerate. When this happens, it could cause loss of natural spine curvature.
Flatback Syndrome causes difficulty in standing up straight. Unfortunately, this syndrome causes patients to stoop forward and leads to a host of other symptoms. Also, patients with a flat back posture often need to bend at the hips and knees to stand upright. And so, this leads to pain and fatigue in the legs that gets worse as the day goes on.
All of these symptoms can become exhausting and painful and may require patients to take prescription pain medications just to function.
With modern spinal fusion techniques and new types of instrumentation, surgeons are now able to preserve much more of the normal spinal alignment and curvature. As a result, the chances of developing Flatback Syndrome as a result of fusion surgery are much lower than in the past.
Flatback syndrome can also occur after a laminectomy (a form of spine surgery). Surgically implanted devices that were used to correct scoliosis in the past can flatten the lumbar spine, thereby leading to flatback syndrome. This complication has been reduced by advancements in surgical techniques.
Also, other conditions cause a reduction in the natural curvature of the back, causing Flatback Syndrome. These conditions are usually associated with aging and most often affect older adults, including:
Degenerative Disc Disease
As we age, the discs in our spine (which act as shock absorbers between the vertebrae) begin to deteriorate. These discs contribute to the normal curvature of the back, and this degeneration can cause the spine to flatten out.
Ankylosing Spondylitis
This arthritic inflammation of the spine can cause stiffness and, in advanced cases, lead to ankylosis. Ankylosis means new bone formation and fusion that causes sections of the spine to fuse in a flat, immobile position.
Vertebral Compression Fractures
A vertebral compression fracture occurs when one or more bones in the spine (vertebrae) become compressed and collapse. This may occur in anyone as a result of trauma, but we see this problem with older adults with osteoporosis.
Post-Laminectomy Syndrome
A surgeon performs a laminectomy to create space in the spinal canal (usually to relieve pressure on the spine) by removing a portion of the vertebra. In some cases, this procedure can cause a decrease in lordosis, leading to a Flatback Deformity.
Diagnosis of Flatback Syndrome
The Diagnosis of Flatback Syndrome occurs through a combination of the patient’s history, a physical examination, and X-rays of the spine. Patients with Flatback Syndrome typically present with a history of prior surgery, as well as difficulty standing upright and associated back and leg pain.
Then, a full-length X-ray of the spine is the next step. Southwest Scoliosis and Spine Institute has a state-of-the-art X-ray imaging system. This system takes high-quality images of patients in just 10-25 seconds. In addition, it takes these scans with smaller amounts of radiation than conventional X-ray systems. This system can also take X-rays of patients in a standing or seated position. It’s conveniently located inside our Dallas location, meaning you and your physician can review the X-rays immediately.
In addition to X-rays of the bones, your physician may also order an MRI or CT scan. This will identify any problems in the soft tissue. Such as the spinal cord, nerves, and/or discs to determine the best and safest course of treatment.
Why is the “S” Curve of the Spine Important?
The “S” curve of the spine plays a crucial role in maintaining balance and stability in the body. This natural curvature helps to evenly distribute gravitational forces, reducing the strain on any single part of the spine.
Benefits of the “S” Curve:
- Stability: The dual curves, located in the upper (thoracic) and lower (lumbar) regions, create a counterbalance that enhances overall stability.
- Shock Absorption: These curvatures act like shock absorbers, allowing the spine to better withstand the pressures from everyday movements such as walking, running, and lifting.
- Load Distribution: By distributing weight more evenly, the “S” curve helps to prevent excessive wear and tear on specific spinal discs and vertebrae.
When the natural “S” curve is disrupted, either through injury, poor posture, or degenerative conditions, the body’s center of gravity is thrown off. This misalignment can lead to significant issues, including chronic pain and reduced mobility.
Maintaining the integrity of the spine’s “S” curve is essential for a balanced and healthy musculoskeletal system. Proper posture, regular exercise, and ergonomic practices are key to preserving this natural alignment.
Understanding Chronic Pain in the Cervical Spine and Upper Back in Flatback Syndrome Patients
Flatback syndrome often leads to chronic pain in the cervical spine and upper back. This happens because the normal curvature of the spine is altered, causing an imbalance that places extra strain on these areas. Here are some key factors contributing to the pain:
- Muscle Fatigue: The muscles in the neck and upper back work harder to maintain a proper posture, leading to fatigue and discomfort.
- Nerve Compression: The abnormal spinal alignment can result in nerves being compressed, leading to persistent pain and discomfort.
- Joint Stress: The changes in posture and alignment can increase stress on the spinal joints, contributing to chronic pain.
Subsequently, patients may experience a combination of these issues, exacerbating their discomfort and requiring comprehensive treatment to address the underlying causes.
Why Is a “Straight” Spine Considered Abnormal in Flatback Syndrome?
A spine that appears perfectly straight in the lower back can be a sign of flatback syndrome, which is far from ideal. The lumbar spine should have a natural curve, known as lordosis. This curvature is crucial for distributing weight evenly and maintaining balance.
Consequences of a Straight Spine:
- Chronic Pain: Losing the lumbar curve forces the spine to handle weight and motion in unnatural ways, leading to persistent discomfort.
- Impaired Mobility: Flatback syndrome can make standing and everyday activities, like walking or lifting objects, extremely difficult.
- Postural Issues: A straight spine can upset your overall posture, causing additional strain on muscles and joints.
Maintaining the spine’s natural curvature is essential for a healthy, pain-free back.
How Do You Fix Flatback Syndrome?
The main aim of treatment for flatback syndrome is to improve the quality of the patient’s life by improving the symptoms. Some patients with Flatback Syndrome can undergo treatment that does not include surgery or minimal surgery, like in Judy’s case (watch the video below). The doctors at Southwest Scoliosis and Spine Institute always utilize the most conservative method to treat a condition before recommending surgery.
Non-Surgical Treatment
At the Southwest Scoliosis and Spine Institute, patients with straight back syndrome have access to a comprehensive range of non-surgical treatment options. The institute offers physical therapy tailored to each individual’s condition, incorporating corrective bracing to support proper posture and alignment.
Corrective Bracing for Optimal Support:
Corrective bracing plays a crucial role in the treatment plan by providing optimal spinal support and stabilization. This helps to maintain the spine’s correct positioning and prevents further progression of the syndrome. To further support our patients, we incorporate a variety of specific exercises to target the core, buttocks, neck, back, and shoulders. Common exercises include:
- Side-lying leg raises
- Planking
- Chest stretches
- Back extensions
- Chin-ups
Hamstring and abdominal stretches are particularly effective at restoring proper alignment of the lumbar spine. By addressing muscle imbalances, these exercises help reverse the patterns that contribute to the condition. Physical therapy sessions also integrate additional stretches and corrective bracing to ensure optimal spinal support and stabilization.
Through this multifaceted approach, our goal is to impact the condition on a structural level, improving posture and enhancing overall spinal health without the need for invasive surgery.
How Can Custom-Prescribed Home Exercises Help With Straight Back Syndrome?
Custom-prescribed home exercises play a crucial role in managing straight back syndrome, offering numerous benefits tailored specifically to your body’s needs. These exercises are designed not only to alleviate symptoms but also to address the root cause of the condition.
Strengthening Core Muscles
One of the primary goals of these exercises is to enhance the strength of your core muscles. A stronger core helps to support your spine, offering better stability and reducing strain on the back. This can lead to significant pain relief and improved posture.
Improving Spinal Alignment
Custom exercises focus on correcting and maintaining optimal spinal alignment. They include stretches and strength-building routines that target muscular imbalances, fostering a more natural spinal curvature. This can be especially helpful in reducing the flatness characteristic of straight back syndrome.
Enhancing Flexibility
Flexibility exercises are also a key component. They work to increase the range of motion in your spine and surrounding muscles. Greater flexibility helps in making daily activities less painful and more manageable.
Promoting Long-Term Health
Consistency in performing these exercises can prevent further deterioration of the spine and improve overall spinal health. Over time, your back becomes stronger and more resilient, making it easier to cope with the demands of everyday life.
Types of Effective Home Exercises
- Planks – Strengthen the core and support spinal alignment.
- Bridges – Target the lower back and glute muscles, enhancing spinal support.
- Cat-Cow Stretch – Improves flexibility and helps in spinal alignment.
Conclusion
Incorporating custom-prescribed home exercises into your daily routine can significantly aid in managing straight back syndrome. By enhancing core strength, improving spinal alignment, and increasing flexibility, these exercises offer a holistic approach to long-term spinal health.
Benefits of a Conservative Treatment Approach
A conservative chiropractic-centered treatment approach is particularly beneficial for several reasons:
- Preservation of Spine’s Strength and Function: This method helps maintain the overall health of the spine, ensuring it remains strong and functional over time.
- Structural Impact: By addressing the condition on a structural level, the treatment targets the root cause without resorting to invasive measures.
- Avoidance of Surgery: Patients can benefit from effective relief and management of their condition without the risks and recovery time associated with surgical interventions.
These benefits reinforce the value of non-surgical methods, demonstrating that a conservative approach can effectively manage straight back syndrome while preserving the spine’s integrity and improving the patient’s quality of life.
Surgery
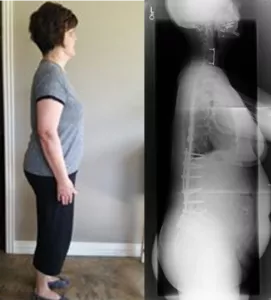 Surgical reconstruction for Flatback Syndrome is usually accomplished with an osteotomy procedure or a tweak of previous surgery hardware. When the spine is too straight, it can cause a pitched-forward posture that gives the appearance of being stooped over. This condition not only affects one’s appearance but also makes it challenging to stand up straight and/or remain standing for longer periods of time. The osteotomy procedure involves removing one or more wedge-shaped sections of bone from the spinal column to restore lordosis to the lumbar vertebrae. Doctors will sometimes also insert rods and screws to ensure that the spine is stable so that it can fuse and heal properly.
Surgical reconstruction for Flatback Syndrome is usually accomplished with an osteotomy procedure or a tweak of previous surgery hardware. When the spine is too straight, it can cause a pitched-forward posture that gives the appearance of being stooped over. This condition not only affects one’s appearance but also makes it challenging to stand up straight and/or remain standing for longer periods of time. The osteotomy procedure involves removing one or more wedge-shaped sections of bone from the spinal column to restore lordosis to the lumbar vertebrae. Doctors will sometimes also insert rods and screws to ensure that the spine is stable so that it can fuse and heal properly.
The operative treatment of flatback syndrome primarily aims to restore lordosis, thereby improving the overall alignment and quality of life of the patient. Our flatback treatment options are designed to stop the deformity from progressing, addressing both the structural and symptomatic aspects of the condition. By correcting the spinal curvature, patients often find relief in their ability to maintain proper posture and stand comfortably for extended periods.
Problems Arising from a Straight Lumbar Spine in Flatback Syndrome
Flatback syndrome occurs when the lumbar spine loses its natural curve and becomes unnaturally straight. This can lead to several issues:
- Chronic Pain: Without the lumbar curve, the spine’s ability to absorb and distribute mechanical stress is compromised, resulting in persistent pain.
- Difficulty Standing and Performing Routine Activities: An unnaturally straight lumbar spine can make it challenging to maintain an upright posture, hindering day-to-day tasks.
- Compensatory Muscle Use: To stand upright, individuals often overuse other muscles, which can lead to further problems over time, such as muscle fatigue and additional strain.
- Exacerbation of Symptoms: While compensatory mechanisms might offer temporary relief, they generally worsen the overall condition, leading to more severe pain and mobility issues.
Proper diagnosis and treatment are essential to manage and mitigate these problems effectively.
Southwest Scoliosis and Spine Institute Specializes in Treating Complex Spinal Conditions and Revision Surgery
At Southwest Scoliosis and Spine Institute, our spine specialists educate patients on their unique spinal conditions. They discuss the different treatment options (both surgical and non-surgical), and the risks and benefits of each. Since the flatback syndrome is a structural problem that involves either a former surgical technique or degenerative disc disease and instability in the spine, it may require surgical reconstruction.
Patients who fail non-surgical treatments or those with a severe deformity that is associated with other neurologic symptoms may require surgery. The goal of the operative treatment of flatback syndrome is to restore lordosis, thereby improving the overall alignment and quality of life of the patient. Our flatback treatment options will stop the deformity from progressing.
Make an Appointment
If you think you may have Flatback Syndrome, it is critical to consult a very skilled spine physician. Especially if it’s the result of an earlier surgery performed by someone else. At Southwest Scoliosis and Spine Institute, with offices in Dallas, Plano, and Frisco, Texas, our board-certified, fellowship-trained surgeons have performed more than 16,000 successful spine surgeries. Richard Hostin, MD, Devesh Ramnath, MD, Ishaq Syed, MD, Shyam Kishan, MD, and Kathryn Wiesman, MD, have the expertise and surgical skills necessary to diagnose and treat the most complex spine cases and revision surgeries.
If you have been told that there is no hope, call us for an evaluation at (214) 556-0555 or visit our contact page today!
____________________
Citation: Medical News Today: Flatback Syndrome
The medical content on this page has been carefully reviewed. It was approved for accuracy by the Southwest Scoliosis and Spine Institute’s qualified healthcare professionals. This includes our board-certified physicians and Physician Assistants. Our team ensures that all information reflects the latest evidence-based practices and meets rigorous standards of medical accuracy, with oversight from our expert spine doctors to guarantee the reliability of our information for our patients.

Recent Comments