LOW BACK PAIN IN ATHLETES
Low back pain in athletes occurs at an alarmingly high rate of athletes will experience low (lumbar) back pain during a competitive season.
At the Southwest Scoliosis and Spine Institute, our Sports Injury Doctors are dedicated to diagnosing and treating spinal problems in athletes and ensuring comprehensive care tailored to each patient’s needs. With advanced techniques and a compassionate approach, our team is here to diagnose, treat, and care for athletes suffering from Low Back Pain.
The Surgeons, Doctors, and Physician Assistants treat athletes with low back pain
 Our Doctors Treat Low Back Pain in Athletes
Our Doctors Treat Low Back Pain in Athletes
Southwest Scoliosis and Spine Institute’s board-certified, fellowship-trained orthopedic physicians, Richard Hostin, MD, Devesh Ramnath, MD, Ishaq Syed, MD, Shyam Kishan, MD, and Kathryn Wiesman, MD, have years of experience treating thousands of patients with low back pain and all types of complex spine conditions.
We see a lot of Athletes, and often with a complaint of low back pain. There can be a lot of factors for low back pain; our first step is to identify the source of the pain. Then we will know exactly how to treat it and get the patient back out in the game.
Athletes are at a Greater Risk of Injury
Athletes are at greater risk of sustaining a lumbar (lower) spine injury due to physical activity. Whether skiing, basketball, football, gymnastics, soccer, dance, running, golf, or tennis, the spine undergoes a lot of stress, absorption of pressure, twisting, turning, and even bodily impact. This strenuous activity puts stress on the back that can cause injury to even the finest and most fit athletes.
When playing sports, about five to ten percent of all athletic injuries occur in the lumbar spine. Therefore, many cases of low back pain in athletes develop because of a specific event or trauma, and other injuries occur because of repetitive minor injuries.
It is sometimes hard for an aggressive athlete to consider changing training schedules. Also, it is hard to accept the fact that a serious disease may exist. Although it is wishful thinking, all athletes who suffer from low back pain should seek medical advice. Consequently, some situations might require reducing or ceasing athletic activity until the healthcare problem goes away. The body’s ability to remain active is worth preserving.
On this page, you will learn about low back pain in athletes, including:
- The spine and back pain
- What generally causes low back pain in athletes
- How a doctor diagnoses back pain
- Available treatment options
Questions and Answers
How can athletes prevent Low Back pain?
Athletes can reduce the risk of low back pain by following these preventive measures:
- Maintaining proper posture during training and competition, including using correct form and technique.
- Incorporating regular strength and conditioning exercises that target the core muscles, including the abdominals, back extensors, and glutes.
- Practicing proper warm-up and cool-down routines to prepare the body for activity and promote muscle flexibility.
- Using appropriate protective equipment and gear, such as supportive footwear or braces, when necessary.
- Listening to their bodies and avoiding overtraining or excessive repetitive movements that can strain the back muscles and structures.
What are the causes of athletes getting Low Back Pain?
Athletes may experience low back pain due to several factors related to their sports activities, including:
- Muscle strains or sprains: Sudden or excessive movements, poor technique, or inadequate warm-up can lead to muscle strains or sprains in the back.
- Stress fractures: Repetitive impact or high-intensity training can cause stress fractures in the vertebrae, resulting in localized pain.
- Disc injuries: High-impact sports or twisting motions can lead to herniated discs or disc degeneration, causing low back pain.
- Spondylolysis: This is a stress fracture in a specific area of the vertebra called the pars interarticularis, commonly seen in sports involving repetitive hyperextension or rotational movements.
- Facet joint dysfunction: Overuse or trauma can cause inflammation or irritation in the facet joints of the spine, leading to pain and stiffness.
What are the treatment options for Athletes with Low Back Pain?
Treatment for low back pain in athletes may include:
- Rest and modified activity: Taking a break from intense training or modifying activity levels to allow the body time to heal.
- Physical therapy: Specific exercises and stretches to strengthen the core muscles, improve flexibility, and address any muscle imbalances or weaknesses.
- Manual therapy: Techniques such as chiropractic adjustments, massage therapy, or acupuncture may be beneficial in relieving pain and promoting healing.
- Pain management: Nonsteroidal anti-inflammatory drugs (NSAIDs) or other pain medications may be prescribed to manage pain and reduce inflammation.
- Rehabilitation: Gradual return-to-play programs that focus on functional movements, sport-specific training, and injury prevention strategies.
- In some cases, minimally invasive procedures or surgery may be considered, particularly for more severe or persistent cases of low back pain.

Anatomy
In order to understand your symptoms and treatment choices, the athlete should start with a basic understanding of the anatomy of the low back. This includes becoming familiar with the various parts that make up the lumbar spine and how they work together.
Click here to learn more about the anatomy of the lumbar spine.
Causes of Pain
Even though low back pain can sometimes be treated without major disruption to a person’s life, athletes are often reluctant to seek medical help. Many of them deny or minimize complaints to avoid consequences, such as having to decrease activity to recover, losing a position, or being removed from a team, missing a competition, or letting the team down.
Some athletes simply do not want to bother seeing a doctor for pain; they hope it will recover on its own.
Many athletes, from the weekend warrior to the elite professional, pop some over-the-counter pain medication and tolerate the pain for the sake of the game and personal enjoyment. But avoiding medical help can lead to further and more serious injury. Without medical help, the anatomic damage can sometimes lead to permanent exclusion from sporting activities.
By not seeking treatment, athletes risk a progression of their condition, which can become severe over time. What starts as a manageable discomfort might evolve into a debilitating issue, making it impossible to participate in sports. This exacerbation not only threatens an athlete’s current performance but also their future in the sport they love.
Ultimately, while the immediate relief from medication may seem sufficient, it’s crucial to address the root cause of the pain with professional medical intervention. This proactive approach can prevent the escalation of injuries and safeguard an athlete’s long-term health and career.
There are many causes of low back pain.
The most common causes in athletes are back strain, spondylolysis, spondylolisthesis, and herniated discs. However, the following factors will lead to lower back pain in athletes.
- Overuse.
- Being overweight.
- Having poor posture.
- Sitting in a poorly designed chair for a long time.
- A misalignment in the bones of your spine, or vertebrae.
- Arthritis in the spine.
- A small fracture, in rare cases.
In addition to these common causes, adolescent athletes may also face unique challenges due to growth-related issues. Conditions like scoliosis and Scheuermann’s kyphosis are particularly noteworthy.
Scoliosis
- Growth-Related: Scoliosis often appears with the onset of puberty, around age 11 in girls and age 13 in boys, coinciding with rapid growth spurts. – Genetic Factors: This condition tends to run in families and is more prevalent in girls. – Symptoms and Progression: While usually painless, scoliosis can cause discomfort during physical activity and may require intervention, such as bracing or even surgery, if it progresses.
Scheuermann’s Kyphosis
- Developmental Changes: This form of kyphosis occurs when vertebrae wedge into a triangular shape, leading to an exaggerated spinal curve. – Impact on Posture: Often described as a ’round-back’ or ‘hunch-back’ posture, it can affect an athlete’s ability to perform optimally.
Understanding these conditions is essential for adolescent athletes, as they can significantly impact performance and require specific management strategies to ensure continued participation in sports.
Back Strain
The medical term used to describe common back strain is musculoligamentous strain. This term refers to all injuries to the lumbar spine’s soft tissue. Soft tissues are the muscles, nerves, ligaments, tendons, and blood vessels around the spine. These are probably the most common types of sports injuries. Back strains are diagnosed by exclusion, which means the diagnosis excludes all other possibilities. These injuries are usually self-limiting. In other words, they do not continue to spread and get worse, they generally heal in time.
Spondylolysis and Spondylolisthesis
A crack in the bony ring of the spinal column is called spondylolysis. If the crack occurs on both sides of the bony ring, the spine can slip forward, a condition called spondylolisthesis. So far, there is no definitive cause of spondylolysis. Most physicians agree that bone defects appear in children mainly due to sports activities that put repeated stress on the pars interarticularis. Spondylolysis appears in younger and older adults as the result of excessive stresses on the spine, eventually causing a stress fracture.
Athletes can get spondylolysis because they frequently hyperextend the lumbar spine. Weightlifters also display a higher incidence of the disorder due to excessive stress on the spine. Spondylolysis does not always produce noticeable symptoms. When it does, chronic low back pain occurs. The pain can stem from mechanical (structural) or compressive (pressure on nerves) pain.
Progression to Spondylolisthesis
Spondylolisthesis occurs when the weakness caused by the spondylolysis causes one vertebra to slip forward over the one below it. Most cases of spondylolysis in athletes do not lead to vertebral slippage. However, if slippage does occur, it may continue. This situation requires more aggressive treatment and perhaps even surgery. The chance of progression occurs more in teenagers than adults, making it a particularly concerning development in younger individuals.
Symptoms and Treatment Options
Many cases appear non-symptomatic and do not cause any nerve problems. However, sometimes the slipped vertebra can press into the space of the spinal canal, leaving less room for the nerve roots. This neural pressure can lead to low back, buttock, and leg pain, as well as numbness in the foot. If the problem generates significant pain or neurological symptoms, doctors may recommend surgery as a potential solution.
By understanding the potential for progression from spondylolysis to spondylolisthesis and recognizing the symptoms that necessitate treatment, individuals can better manage their condition and seek appropriate medical advice when necessary.
Herniated Discs
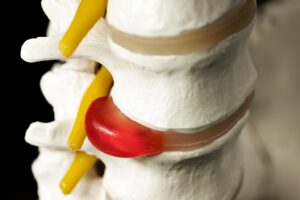
Many sports produce high amounts of pressure on the spine. Over time, these repeated stresses add up and begin to affect the discs in the spine. A herniated disc occurs when the pressure on a disc’s outer fibers (annulus) causes ripping, and the nucleus ruptures out of its normal space.
If it rips near the spinal canal, the bulging disc can push out of its space and into the spinal canal, placing inappropriate pressure on the spinal cord and nerve roots. If a disc bulges substantially or fragments into pieces that lie in the canal, then irritation of the nerves can be severe.
The compression to the nerves caused by herniation can lead to feelings of numbness, pain, a change in reflexes, and tingling in the arms or legs. In addition, if a disc ruptures, it releases chemicals that can irritate and inflame the nerve roots, which leads to extreme discomfort. Sometimes a herniated disc is referred to as a “slipped disc,” though the disc does not actually slip.
Diagnosis
In evaluating low back pain in athletes, your doctor will start by gathering information about the current problem and a complete history of any additional medical problems. Athletes tend to live with a certain amount of constant pain. This can cause them to ignore or minimize the severity of their pain. They may also be used to dealing with more pain than the average patient, which sometimes makes it harder to adequately assess their symptoms. This is why a thorough history of the athlete is needed.
Before determining a diagnosis and developing a treatment plan, your physician will need to know:
- your age
- the type(s) of sport(s) and level of competition in which you are involved
- all past and current medical problems
- the location of the pain and where it spreads
- when the pain began, along with the pain’s relation to any specific trauma
- what causes pain or relieves it
- about any drug or medication use
Doctors also focus on understanding the athlete’s lifestyle and any habitual movements that may contribute to or alleviate pain. This information is crucial in tailoring a treatment plan that aligns with the athlete’s needs and goals.
Physical Exam
Your doctor will examine your entire spine looking for signs of unusual curves, a rib hump, a tilted pelvis, and tilting of the shoulders. Your doctor will test your muscle strength as well as your reflexes, sensation, and ability to perform specific movements. Additional tests will include X-rays or MRI or CT scans to further pinpoint the diagnosis.
The examination process is thorough, assessing not only the spine but also the athlete’s overall physical condition. This comprehensive approach helps in identifying any underlying issues that may not be immediately obvious, ensuring a more accurate diagnosis and effective treatment plan.
Treatment Options
Conservative Treatment
The majority of low back pain in athletes can be treated with conservative means. Treatments will vary depending on the cause of pain. Back strains may simply require a short period of limited activity, medication, and ice applications. When symptoms ease, athletes are usually able to resume their sports activity gradually, applying concepts of proper conditioning and warm-ups.
Athletes with spondylolysis and spondylolisthesis may require the use of a brace, along with rigorous avoidance of sports activity. The brace is commonly prescribed for three months, after which athletes gradually return to their sports activities. The treatment for a herniated disc depends on the symptoms and degree of nerve irritation or dysfunction. In most cases, our doctors believe that Herniated discs do not need surgery to get better.
Medication
Your doctor may prescribe anti-inflammatory medications to reduce pain and swelling.
Ice
If the injury just happened, your doctor may instruct you to apply ice to the sore area. Cold packs are typically applied for 15 to 20 minutes. Some doctors recommend the use of contrast applications by alternating cold and hot packs every five minutes over the sore area.
Specific Rest
Immediately after a back injury, your back should rest, and it will normally get better. Meanwhile, rest will take the pressure off your spine and the muscles around it. Furthermore, you should rest in a comfortable position on a firm mattress. However, doctors usually advise against bed rest for more than two days. Also, staying in bed longer than two days can weaken key muscles of the trunk. In most cases of sudden back pain, the sooner you start moving again, the sooner your back pain will improve.
Bracing
If a spine specialist feels you may have a true stress fracture from athletic activity, you might use a back brace (24 hours a day) for several months to allow the fracture to heal. You will then gradually stop using the brace, and your doctor will advise that you can return to full activity. Surgery rarely occurs for these problems.
Physical Therapy
Your doctor may have you work with a physical therapist. A well-rounded rehabilitation program assists in calming pain and inflammation, improving your mobility and strength, and helping you get back to optimal performance with sports activities.
Athletes understand that exercise strengthens the abdominal, paraspinal, and pelvic muscles. Strong muscles in these areas can take the pressure off the spine and help prevent back injuries. A physical therapist can help a patient develop a beneficial routine of conditioning and rehabilitation that includes proper warm-ups (such as back stretching exercises) and aerobic exercise.
The goals of physical therapy are to help you:
- Apply proper conditioning, warm-ups, and cool-downs
- Use proper technique in your sports activity
- Choose appropriate equipment for your sport
- Maximize your flexibility and core strength
- Learn ways to manage your condition
These measures and exercises are essential components in both preventing and treating low back pain, ensuring athletes can maintain peak performance while safeguarding their spinal health.
Steroid Injections
Doctors recommend an epidural steroid injection (ESI) to stop severe pain from nerve root irritation due to a herniated disc. These steroid injections combine cortisone (a powerful anti-inflammatory steroid) and a local anesthetic that is given through the back into the epidural space. Recommendations for this medication do not occur unless conservative treatments do not work. An ESI becomes successful in reducing the pain from a herniated disc in about half the cases.
Learn more about Epidural Steroid Injection
Surgical Treatment for Low Back Pain
Surgical treatment for lower back pain becomes necessary only if conservative treatments fail to keep your pain at a tolerable level. In addition, the surgery must address the presence of mechanical and compressive symptoms.
Nerve pressure may require surgical decompression, called a decompressive laminectomy of the lumbar spine. To free up or “decompress” the nerves, the surgeon must remove a section of bone from the back of the spine (lamina). The surgeon may also have to remove a portion of the facet joints. The lamina and facet joints normally provide stability in the spine.
Removal of either or both can cause the spine to become loose and unstable. When this occurs, doctors will include fusion. Likewise, patients needing surgery for spinal instability due to spondylolisthesis typically require lumbar fusion.
Athletes with Low Back Pain Should See the Doctors at Southwest Scoliosis and Spine Institute
- The doctors at Southwest Scoliosis and Spine Institute are experts in the treatment of low back pain in athletes. They have extensive experience in diagnosing and treating a variety of spinal conditions that can cause low back pain in athletes, including spondylolysis, spondylolisthesis, and herniated discs.
- The doctors at Southwest Scoliosis and Spine Institute use a variety of conservative treatment methods to treat low back pain in athletes. These methods include physical therapy, exercise, and medications. If conservative treatment is not successful, the doctors may recommend surgery.
- The doctors at Southwest Scoliosis and Spine Institute are committed to helping athletes return to their sport as quickly and safely as possible. They work with athletes to develop a personalized treatment plan that will allow them to get back to their sport without further injury.
In addition to their expertise in the treatment of low back pain in athletes, the doctors at Southwest Scoliosis and Spine Institute also offer several other services, including:
- Scoliosis screening and treatment
- Kyphosis screening and treatment
- Spine surgery
- Pain management
- Rehabilitation
Schedule an Appointment
If you are an athlete with low back pain, it is recommended that you schedule an appointment with the doctors at Southwest Scoliosis and Spine Institute. They can help you diagnose the cause of your pain and develop a treatment plan that will get you back to your sport as quickly and safely as possible. Finally, please note that appointments are available within 24 hours.
Here are some additional reasons why athletes with low back pain should see the doctors at Southwest Scoliosis and Spine Institute:
- The institute is equipped with state-of-the-art technology, including an EOS X-ray system, which allows for low-dose imaging of the spine.
- The institute offers a variety of minimally invasive surgical procedures, which can help athletes return to their sport more quickly.
- The institute has a team of experienced physical therapists who can help athletes develop a personalized exercise program to strengthen their back and core muscles.
If you are an athlete with low back pain, we encourage you to contact Southwest Scoliosis and Spine Institute to schedule an appointment. The doctors at the institute can help you get back to your sport and enjoy a pain-free life.
____________________
Citation: American Society for Sports Medicine – Lower Back Pain in Athletes
The medical content on this page has been carefully reviewed. It was approved for accuracy by the Southwest Scoliosis and Spine Institute’s qualified healthcare professionals. This includes our board-certified physicians and Physician Assistants. Our team ensures that all information reflects the latest evidence-based practices and meets rigorous standards of medical accuracy, with oversight from our expert spine doctors to guarantee the reliability of our information for our patients.
If you or a loved one suffers from spinal pain, you owe it to yourself to call Southwest Scoliosis and Spine Institute at 214-556-0555 to make an appointment.


